Relative and Absolute Risk to Guide the Management of Pulse Pressure, an Age-Related Cardiovascular Risk Factor
- PMID: 33687055
- PMCID: PMC8457427
- DOI: 10.1093/ajh/hpab048
Relative and Absolute Risk to Guide the Management of Pulse Pressure, an Age-Related Cardiovascular Risk Factor
Abstract
Background: Pulse pressure (PP) reflects the age-related stiffening of the central arteries, but no study addressed the management of the PP-related risk over the human lifespan.
Methods: In 4,663 young (18-49 years) and 7,185 older adults (≥50 years), brachial PP was recorded over 24 hours. Total mortality and all major cardiovascular events (MACEs) combined were coprimary endpoints. Cardiovascular death, coronary events, and stroke were secondary endpoints.
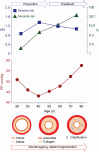
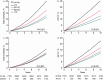
Results: In young adults (median follow-up, 14.1 years; mean PP, 45.1 mm Hg), greater PP was not associated with absolute risk; the endpoint rates were ≤2.01 per 1,000 person-years. The adjusted hazard ratios expressed per 10-mm Hg PP increments were less than unity (P ≤ 0.027) for MACE (0.67; 95% confidence interval [CI], 0.47-0.96) and cardiovascular death (0.33; 95% CI, 0.11-0.75). In older adults (median follow-up, 13.1 years; mean PP, 52.7 mm Hg), the endpoint rates, expressing absolute risk, ranged from 22.5 to 45.4 per 1,000 person-years and the adjusted hazard ratios, reflecting relative risk, from 1.09 to 1.54 (P < 0.0001). The PP-related relative risks of death, MACE, and stroke decreased >3-fold from age 55 to 75 years, whereas absolute risk rose by a factor 3.
Conclusions: From 50 years onwards, the PP-related relative risk decreases, whereas absolute risk increases. From a lifecourse perspective, young adulthood provides a window of opportunity to manage risk factors and prevent target organ damage as forerunner of premature death and MACE. In older adults, treatment should address absolute risk, thereby extending life in years and quality.
Keywords: arterial stiffness; blood pressure; cardiovascular disease; hypertension; mortality; population science; pulse pressure.
© The Author(s) 2021. Published by Oxford University Press on behalf of American Journal of Hypertension, Ltd.
Figures

Similar articles
-
Predictive power of 24-h ambulatory pulse pressure and its components for mortality and cardiovascular outcomes in 11 848 participants recruited from 13 populations.J Hypertens. 2022 Nov 1;40(11):2245-2255. doi: 10.1097/HJH.0000000000003258. Epub 2022 Aug 8. J Hypertens. 2022. PMID: 35950994 Free PMC article.
-
Do estimated 24-h pulse pressure components affect outcome? The Ohasama study.J Hypertens. 2020 Jul;38(7):1286-1292. doi: 10.1097/HJH.0000000000002366. J Hypertens. 2020. PMID: 32004208
-
Association of Blood Pressure Classification in Korean Young Adults According to the 2017 American College of Cardiology/American Heart Association Guidelines With Subsequent Cardiovascular Disease Events.JAMA. 2018 Nov 6;320(17):1783-1792. doi: 10.1001/jama.2018.16501. JAMA. 2018. PMID: 30398603 Free PMC article.
-
Association between high blood pressure and long term cardiovascular events in young adults: systematic review and meta-analysis.BMJ. 2020 Sep 9;370:m3222. doi: 10.1136/bmj.m3222. BMJ. 2020. PMID: 32907799 Free PMC article.
-
Blood pressure targets in adults with hypertension.Cochrane Database Syst Rev. 2020 Dec 17;12(12):CD004349. doi: 10.1002/14651858.CD004349.pub3. Cochrane Database Syst Rev. 2020. PMID: 33332584 Free PMC article.
Cited by
-
Elevated pulse pressure and cardiovascular risk associated in Spanish population attended in primary care: IBERICAN study.Front Cardiovasc Med. 2023 May 9;10:1090458. doi: 10.3389/fcvm.2023.1090458. eCollection 2023. Front Cardiovasc Med. 2023. PMID: 37229234 Free PMC article.
-
[Luces y sombras de la Guía Europea esc-2021 de Prevención de la Enfermedad Cardiovascular en la Práctica Clínica.].Rev Esp Salud Publica. 2023 Aug 16;97:e202308064. Rev Esp Salud Publica. 2023. PMID: 37921403 Free PMC article. Spanish.
-
Age-Dependent Associations Between Pulse Pressure and Long-Term Outcomes After Myocardial Infarction.J Clin Hypertens (Greenwich). 2025 Apr;27(4):e70043. doi: 10.1111/jch.70043. J Clin Hypertens (Greenwich). 2025. PMID: 40259740 Free PMC article.
-
Mortality and Cardiovascular End Points In Relation to the Aortic Pulse Wave Components: An Individual-Participant Meta-Analysis.Hypertension. 2024 May;81(5):1065-1075. doi: 10.1161/HYPERTENSIONAHA.123.22036. Epub 2024 Feb 23. Hypertension. 2024. PMID: 38390718 Free PMC article.
-
Prognostic Impact of 24-Hour Pulse Pressure Components in Treated Hypertensive Patients Older Than 65 Years.Diagnostics (Basel). 2023 Feb 23;13(5):845. doi: 10.3390/diagnostics13050845. Diagnostics (Basel). 2023. PMID: 36899989 Free PMC article.
References
-
- Staessen J, Amery A, Fagard R. Isolated systolic hypertension in the elderly. J Hypertens 1990; 8:393–405. - PubMed
-
- Verdecchia P, Schillaci G, Borgioni C, Ciucci A, Pede S, Porcellati C. Ambulatory pulse pressure: a potent predictor of total cardiovascular risk in hypertension. Hypertension 1998; 32:983–988. - PubMed
-
- Blacher J, Staessen JA, Girerd X, Gasowski J, Thijs L, Liu L, Wang JG, Fagard RH, Safar ME. Pulse pressure not mean pressure determines cardiovascular risk in older hypertensive patients. Arch Intern Med 2000; 160:1085–1089. - PubMed
-
- Khattar RS, Swales JD, Dore C, Senior R, Lahiri A. Effect of aging on the prognostic significance of ambulatory systolic, diastolic, and pulse pressure in essential hypertension. Circulation 2001; 104:783–789. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

