Persistent Symptoms and Disability After COVID-19 Hospitalization: Data From a Comprehensive Telerehabilitation Program
- PMID: 33711279
- PMCID: PMC7943375
- DOI: 10.1016/j.apmr.2021.03.001
Persistent Symptoms and Disability After COVID-19 Hospitalization: Data From a Comprehensive Telerehabilitation Program
Abstract
Objective: To report symptoms, disability, and rehabilitation referral rates after coronavirus disease 2019 (COVID-19) hospitalization in a large, predominantly older population.
Design: Cross-sectional study, with postdischarge telemonitoring of individuals hospitalized with confirmed COVID-19 at the first month after hospital discharge, as part of a comprehensive telerehabilitation program.
Setting: Private verticalized health care network specialized in the older population.
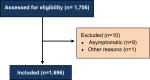
Participants: Individuals hospitalized because of COVID-19. We included 1696 consecutive patients, aged 71.8±13.0 years old and 56.1% female. Comorbidities were present in 82.3% of the cases (N=1696).
Interventions: Not applicable.
Main outcome measures: Dependence for basic activities of daily living (ADL) and instrumental activities of daily living (IADL) using the Barthel Index and Lawton's Scale. We compared the outcomes between participants admitted to the intensive care unit (ICU) vs those admitted to the ward.
Results: Participant were followed up for 21.8±11.7 days after discharge. During postdischarge assessment, independence for ADL was found to be lower in the group admitted to the ICU than the ward group (61.1% [95% confidence interval (CI), 55.8%-66.2%] vs 72.7% [95% CI, 70.3%-75.1%], P<.001). Dependence for IADL was also more frequent in the ICU group (84.6% [95% CI, 80.4%-88.2%] vs 74.5%, [95% CI, 72.0%-76.8%], P<.001). Individuals admitted to ICU required more oxygen therapy (25.5% vs 12.6%, P<.001), presented more shortness of breath during routine (45.2% vs 34.5%, P<.001) and nonroutine activities (66.3% vs 48.2%, P<.001), and had more difficulty standing up for 10 minutes (49.3% vs 37.9% P<.001). The rehabilitation treatment plan consisted mostly of exercise booklets, which were offered to 65.5% of participants. The most referred rehabilitation professionals were psychologists (11.8%), physical therapists (8.0%), dietitians (6.8%), and speech-language pathologists (4.6%).
Conclusions: Individuals hospitalized because of COVID-19 present high levels of disability, dyspnea, dysphagia, and dependence for both ADL and IADL. Those admitted to the ICU presented more advanced disability parameters.
Keywords: Activities of daily living; COVID-19; Deglutition disorders; Disabled persons; Dyspnea; Mental disorders; Rehabilitation; Telerehabilitation.
Copyright © 2021 The American Congress of Rehabilitation Medicine. Published by Elsevier Inc. All rights reserved.
Figures
References
-
- Ceravolo MG, Arienti C, De Sire A, et al. Rehabilitation and COVID-19: the Cochrane Rehabilitation 2020 rapid living systematic review. Eur J Phys Rehabil Med. 2020;56:642–651. - PubMed
-
- Curci C, Pisano F, Bonacci E, et al. Early rehabilitation in post-acute COVID-19 patients: data from an Italian COVID-19 rehabilitation unit and proposal of a treatment protocol. A cross-sectional study. Eur J Phys Rehabil Med. 2020;56:633–641. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical