Prasugrel versus ticagrelor in patients with myocardial infarction undergoing percutaneous coronary intervention
- PMID: 33712510
- PMCID: PMC8257560
- DOI: 10.1136/heartjnl-2020-318694
Prasugrel versus ticagrelor in patients with myocardial infarction undergoing percutaneous coronary intervention
Abstract
Objective: The comparative efficacy and safety of prasugrel and ticagrelor in patients with myocardial infarction (MI) treated with percutaneous coronary intervention (PCI) remain unclear. We aimed to investigate the association of treatment with clinical outcomes.
Methods: In the SWEDEHEART (Swedish Web-system for enhancement and development of evidence-based care in heart disease evaluated according to recommended therapies) registry, all patients with MI treated with PCI and discharged on prasugrel or ticagrelor from 2010 to 2016 were included. Outcomes were 1-year major adverse cardiac and cerebrovascular events (MACCE, death, MI or stroke), individual components and bleeding. Multivariable adjustment, inverse probability of treatment weighting (IPTW) and propensity score matching (PSM) were used to adjust for confounders.
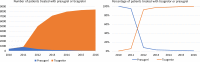
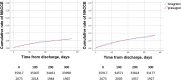
Results: We included 37 990 patients, 2073 in the prasugrel group and 35 917 in the ticagrelor group. Patients in the prasugrel group were younger, more often admitted with ST elevation MI and more likely to have diabetes. Six to twelve months after discharge, 20% of patients in each group discontinued the P2Y12 receptor inhibitor they received at discharge. The risk for MACCE did not significantly differ between prasugrel-treated and ticagrelor-treated patients (adjusted HR 1.03, 95% CI 0.86 to 1.24). We found no significant difference in the adjusted risk for death, recurrent MI or stroke alone between the two treatments. There was no significant difference in the risk for bleeding with prasugrel versus ticagrelor (2.5% vs 3.2%, adjusted HR 0.92, 95% CI 0.69 to 1.22). IPTW and PSM analyses confirmed the results.
Conclusion: In patients with MI treated with PCI, prasugrel and ticagrelor were associated with similar efficacy and safety during 1-year follow-up.
Keywords: acute coronary syndrome; percutaneous coronary intervention.
© Author(s) (or their employer(s)) 2021. No commercial re-use. See rights and permissions. Published by BMJ.
Conflict of interest statement
Competing interests: DV reports a grant from Boston Scientific, outside the submitted work. DE reports speaker fees from AstraZeneca and Bayer and serves in the advisor board for Bayer and Boehringer Ingelheim, outside the submitted work. EH reports grants and honoraria from Amgen, Sanofi, Bayer and NovoNordisk, outside the submitted work. LM reports consulting fees/lecture from AstraZeneca, Bayer, Boehringer Ingelheim Novartis, NovoNordisk, MSD, Sanofi and Amgen, outside the submitted work. EO reports institutional research grant from AstraZeneca and consulting fees from Novartis, MSD, AstraZeneca and Bayer, outside the submitted work. TJ reports research grants from MSD and Novartis, outside the submitted work. JA reports grants and lecture fees from AstraZeneca, Lilly, Pfizer, Bayer, Novartis and Boehringer Ingelheim, and serving on advisory board for AstraZeneca, Novartis and MSD, outside the submitted work.
Figures

Similar articles
-
Comparison of 1-year clinical outcomes between prasugrel and ticagrelor versus clopidogrel in type 2 diabetes patients with acute myocardial infarction underwent successful percutaneous coronary intervention.Medicine (Baltimore). 2019 Mar;98(11):e14833. doi: 10.1097/MD.0000000000014833. Medicine (Baltimore). 2019. PMID: 30882670 Free PMC article.
-
Safety and Efficacy in Prasugrel- Versus Ticagrelor-Treated Patients With ST-Elevation Myocardial Infarction.J Cardiovasc Pharmacol. 2018 Oct;72(4):186-190. doi: 10.1097/FJC.0000000000000609. J Cardiovasc Pharmacol. 2018. PMID: 29985284
-
Efficacy and Safety of Clopidogrel, Prasugrel and Ticagrelor in ACS Patients Treated with PCI: A Propensity Score Analysis of the RENAMI and BleeMACS Registries.Am J Cardiovasc Drugs. 2020 Jun;20(3):259-269. doi: 10.1007/s40256-019-00373-1. Am J Cardiovasc Drugs. 2020. PMID: 31586336
-
Prasugrel or ticagrelor relative to clopidogrel in triple-antiplatelet treatment combined with glycoprotein IIb/IIIa inhibitor for patients with STEMI undergoing PCI: a meta-analysis.BMC Cardiovasc Disord. 2020 Mar 12;20(1):130. doi: 10.1186/s12872-020-01403-6. BMC Cardiovasc Disord. 2020. PMID: 32164560 Free PMC article.
-
Switching to Clopidogrel in Patients With Acute Coronary Syndrome Managed With Percutaneous Coronary Intervention Initially Treated With Prasugrel or Ticagrelor: Systematic Review and Meta-analysis.Ann Pharmacother. 2019 Oct;53(10):997-1004. doi: 10.1177/1060028019845334. Epub 2019 Apr 18. Ann Pharmacother. 2019. PMID: 30999764
Cited by
-
Dual Antiplatelet Therapy: A Concise Review for Clinicians.Life (Basel). 2023 Jul 18;13(7):1580. doi: 10.3390/life13071580. Life (Basel). 2023. PMID: 37511955 Free PMC article. Review.
-
Sex-based Differences in Percutaneous Coronary Intervention Outcomes in Patients with Ischaemic Heart Disease.Eur Cardiol. 2023 Mar 2;18:e06. doi: 10.15420/ecr.2022.24. eCollection 2023. Eur Cardiol. 2023. PMID: 37456769 Free PMC article. Review.
-
Ticagrelor versus Prasugrel in Patients with Acute Coronary Syndrome Undergoing Percutaneous Coronary Intervention: Analysis from the Acute Coronary Syndrome Israeli Survey.Cardiology. 2022;147(2):113-120. doi: 10.1159/000521042. Epub 2021 Nov 22. Cardiology. 2022. PMID: 34808635 Free PMC article.
-
Reversal of Platelet Inhibition in Patients Receiving Ticagrelor.Rev Cardiovasc Med. 2022 Sep 5;23(9):300. doi: 10.31083/j.rcm2309300. eCollection 2022 Sep. Rev Cardiovasc Med. 2022. PMID: 39077695 Free PMC article. Review.
-
Potent P2Y12 Inhibitor Selection and De-escalation Strategies in Acute Coronary Syndrome Patients Undergoing Percutaneous Coronary Intervention: Systematic Review and Meta-analysis.CJC Open. 2023 Dec 5;6(5):677-688. doi: 10.1016/j.cjco.2023.11.024. eCollection 2024 May. CJC Open. 2023. PMID: 38846440 Free PMC article. Review.
References
-
- Gurbel PA, Bliden KP, Butler K, et al. . Randomized double-blind assessment of the onset and offset of the antiplatelet effects of ticagrelor versus clopidogrel in patients with stable coronary artery disease: the ONSET/OFFSET study. Circulation 2009;120:2577–85. 10.1161/CIRCULATIONAHA.109.912550 - DOI - PubMed
Publication types
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous
