A Nomogram Predicting the Prognosis of Children With Biliary Atresia After Hepatoportoenterostomy
- PMID: 33718307
- PMCID: PMC7943446
- DOI: 10.3389/fped.2021.641318
A Nomogram Predicting the Prognosis of Children With Biliary Atresia After Hepatoportoenterostomy
Abstract
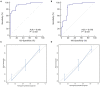
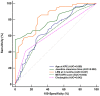
Background: Although Kasai portoenterostomy (KPE) is performed timely for most children with biliary atresia (BA), the native liver survival (NLS) is still poor due to the progressive liver fibrosis. Many children have to receive liver transplantation (LT) within 2 years after KPE. Early prediction of the prognosis permits the implementation of prophylactic treatments for BA children. However, studies about the prediction are limited. Objective: The purpose of this study is to establish a nomogram to predict the prognosis of BA children within 2 years after KPE. Methods: The follow-up data of 151 BA children were retrospectively reviewed, and were randomly divided into a training cohort for constructing a nomogram (n = 103) and a validation cohort (n = 48). In the training cohort, patients were divided into Group A and Group B according to whether death or LT were observed within 2 years post-KPE. Multivariate Cox regression based on the baseline characteristics, liver function indicators and LSM (liver stiffness measurement) values at KPE and 3 months after KPE was utilized for the establishment of the nomogram in predicting the prognosis of BA within 2 years after KPE. The discrimination and calibration of the nomogram were internally and externally validated. Results: Fifty-six BA children were included in Group A and 47 were included in group B. Age at KPE, METAVIR score F4, LSM at 3 months, first onset of cholangitis within 3 months, and jaundice clearance time were the independent predictors for the prognosis of BA children within 2 years after KPE (all P < 0.05). The developed nomogram based on these independent predictors showed good discrimination and calibration by the internal and external validation. Its performance was better than each predictor in predicting the prognosis (all P < 0.05). Conclusions: The established nomogram based on the indicators from the first 3 months after KPE may be useful for predicting the prognosis of BA children within 2 years post-KPE and helpful for the consideration of LT.
Keywords: LSM; biliary atresia; kasai portoenterostomy; liver transplantation; nomogram; prognosis.
Copyright © 2021 Liu, Chen, Zhou, Li, Tang and Zhou.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures

References
LinkOut - more resources
Full Text Sources
Other Literature Sources

