Reducing Pediatric ED Length of Stay by Reducing Diagnostic Testing: A Discrete Event Simulation Model
- PMID: 33718751
- PMCID: PMC7952107
- DOI: 10.1097/pq9.0000000000000396
Reducing Pediatric ED Length of Stay by Reducing Diagnostic Testing: A Discrete Event Simulation Model
Abstract
Quality improvement efforts can require significant investment before the system impact of those efforts can be evaluated. We used discrete event simulation (DES) modeling to test the theoretical impact of a proposed initiative to reduce diagnostic testing for low-acuity pediatric emergency department (ED) patients.
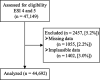
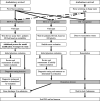
Methods: We modified an existing DES model, built at another large, urban, academic pediatric ED, to forecast the impact of reducing diagnostic testing rates on mean ED length of stay (LOS). The modified model included local testing rates for Emergency Severity Index (ESI) 4 and 5 patients and additional processes defined by local experts. Validation was performed by comparing model output predictions of mean LOS and wait times to actual site-specific data. We determined the goal reduction in diagnostic testing rates using the Achievable Benchmark of Care methodology. Model output mean LOS and wait times, with testing set at benchmark rates, were compared to outputs with testing set at current levels.
Results: During validation testing, model output metrics approximated actual clinical data with no statistically significant differences. Compared to model outputs with current testing rates, the mean LOS with testing set at an achievable benchmark was significantly shorter for ESI 4 (difference 19.1 mins [95% confidence interval 12.2, 26.0]) patients.
Conclusion: A DES model predicted a statistically significant decrease in mean LOS for ESI 4 pediatric ED patients if diagnostic testing is performed at an achievable benchmark rate compared to current rates. DES shows promise as a tool to evaluate the impact of a QI initiative before implementation.
Copyright © 2021 the Author(s). Published by Wolters Kluwer Health, Inc.
Figures
References
-
- McCarthy ML, Ding R, Pines JM, et al. . Provider variation in fast track treatment time. Med Care. 2012; 50:43–49 - PubMed
-
- Byczkowski TL, Fitzgerald M, Kennebeck S, et al. . A comprehensive view of parental satisfaction with pediatric emergency department visits. Ann Emerg Med. 2013; 62:340–350 - PubMed
-
- Crane J, Noon C. The Definitive Guide to Emergency Department Operational Improvement: Employing Lean Principles with Current ED Best Practices to Create the “No Wait” Department. 2011, 1st. New York, NY: Productivity Press
-
- Powell EC, Hampers LC. Physician variation in test ordering in the management of gastroenteritis in children. Arch Pediatr Adolesc Med. 2003; 157:978–983 - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources