Potential Link between Ossification of Nuchal Ligament and the Risk of Cervical Ossification of Posterior Longitudinal Ligament: Evidence and Clinical Implication from a Meta-Analysis of 8429 Participants
- PMID: 33719181
- PMCID: PMC8126919
- DOI: 10.1111/os.12938
Potential Link between Ossification of Nuchal Ligament and the Risk of Cervical Ossification of Posterior Longitudinal Ligament: Evidence and Clinical Implication from a Meta-Analysis of 8429 Participants
Abstract
Objective: The aim of the present paper was to evaluate the strength and the magnitude of the association between ossification of the nuchal ligament (ONL) and the risk of cervical ossification of the posterior longitudinal ligament (COPLL) and to determine whether there is a direct association or whether COPLL is a consequence of shared risk factors.
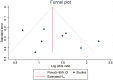
Methods: Medline, Web of Science, Cochrane Library, and Embase databases were searched for studies evaluating the association of COPLL-ONL published before July 2020. Eligible studies were selected based on certain inclusion and exclusion criteria. Two investigators independently conducted the quality assessment and extracted the data, including study designs, countries, patients' age, gender, body mass index (BMI), and the risk of COPLL between individuals with and without ONL. A meta-analysis of homogenous data, a sensitivity analysis, a publication bias assessment, and a subgroup analysis were performed using Stata 12.0 software.
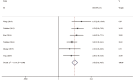
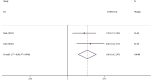
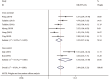
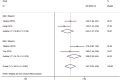
Results: A total of 10 cohort studies involving 8429 participants were incorporated into this analysis. Pooled results demonstrated a statistically significant association between the presence of ONL and the increased COPLL risk (odds ratio [OR] 3.84; 95% confidence interval [CI] 2.68-5.52, P < 0.001). Furthermore, subgroup analyses indicated that this association was independent of study design (6.36-fold in case-control studies vs 3.22-fold in cross-sectional studies), sex (6.33-fold in male-female ratio >2.5 vs 2.91-fold in male-female ratio <2.5), age (4.28-fold in age ≥55 years vs 3.45-fold in age <55 years), and BMI (3.88-fold in BMI ≥ 25 kg/m2 vs 2.43-fold in BMI < 25 kg/m2 ), which also indicated that obese, older male patients with ONL had a higher risk of OPLL. Moreover, combined two articles revealed that patients with larger-type ONL had a significantly higher risk of long-segment COPLL compared with controls (OR 1.86; 95% CI 1.41-2.47, P < 0.001).
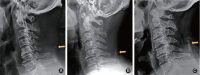
Conclusion: This is the first meta-analysis to demonstrate a strong and steady association between ONL and higher risk of COPLL. This association was independent of sex, age, and BMI. Considering that ONL is generally asymptomatic and easily detectable on X-ray, our findings implied that ONL might serve as an early warning sign of the onset of COPLL and provide clinicians an opportunity for early detection and early intervention.
Keywords: Cervical; Meta-analysis; Ossification of the nuchal ligament; Ossification of the posterior longitudinal ligament; Risk.
© 2021 The Authors. Orthopaedic Surgery published by Chinese Orthopaedic Association and John Wiley & Sons Australia, Ltd.
Figures






Similar articles
-
Radiographic analysis of the correlation between ossification of the nuchal ligament and sagittal alignment and segmental stability of the cervical spine in patients with cervical spondylotic myelopathy.Acta Radiol. 2019 Feb;60(2):196-203. doi: 10.1177/0284185118778866. Epub 2018 May 22. Acta Radiol. 2019. PMID: 29788751
-
Radiographic Features and Correlation Analysis of Location of Ossification in Patients with Cervical Ossification of the Posterior Longitudinal Ligament Combined with Ossification of the Nuchal Ligament.World Neurosurg. 2018 Aug;116:e929-e933. doi: 10.1016/j.wneu.2018.05.130. Epub 2018 May 28. World Neurosurg. 2018. PMID: 29852300
-
Association between ossification of the posterior longitudinal ligament and ossification of the nuchal ligament in the cervical spine.PLoS One. 2019 Nov 6;14(11):e0224729. doi: 10.1371/journal.pone.0224729. eCollection 2019. PLoS One. 2019. PMID: 31693687 Free PMC article.
-
Ossification of the Ligaments in the Cervical Spine, Including Ossification of the Anterior Longitudinal Ligament, Ossification of the Posterior Longitudinal Ligament, and Ossification of the Ligamentum Flavum.Neurosurg Clin N Am. 2018 Jan;29(1):63-68. doi: 10.1016/j.nec.2017.09.018. Neurosurg Clin N Am. 2018. PMID: 29173437 Review.
-
Comparison of clinical outcomes in decompression and fusion versus decompression only in patients with ossification of the posterior longitudinal ligament: a meta-analysis.Neurosurg Focus. 2016 Jun;40(6):E9. doi: 10.3171/2016.3.FOCUS1630. Neurosurg Focus. 2016. PMID: 27246492
Cited by
-
The role of miRNAs as biomarkers in heterotopic ossification.EFORT Open Rev. 2024 Dec 2;9(12):1120-1133. doi: 10.1530/EOR-22-0100. EFORT Open Rev. 2024. PMID: 39620561 Free PMC article. Review.
-
Effect of K-line (-) or (+) on surgical outcomes in cervical ossification of the posterior longitudinal ligament: A systematic and meta-analysis.Medicine (Baltimore). 2024 Nov 22;103(47):e40675. doi: 10.1097/MD.0000000000040675. Medicine (Baltimore). 2024. PMID: 39809181 Free PMC article.
-
Potential Influence of Sagittal Parameters in the Pathogenesis of Patients With the Thoracic Ossification of the Ligamentum Flavum.Orthop Surg. 2025 Jul;17(7):1956-1964. doi: 10.1111/os.70061. Epub 2025 May 26. Orthop Surg. 2025. PMID: 40420546 Free PMC article.
References
-
- Boody BS, Lendner M, Vaccaro AR. Ossification of the posterior longitudinal ligament in the cervical spine: a review. Int Orthop, 2019, 43: 797–805. - PubMed
-
- Shin J, Choi JY, Kim YW, Chang JS, Yoon SY. Quantification of risk factors for cervical ossification of the posterior longitudinal ligament in Korean populations: a nationwide population‐based case‐control study. Spine, 2019, 44: E957–E964. - PubMed
-
- Mori K, Yoshii T, Hirai T, et al. The characteristics of the patients with radiologically severe cervical ossification of the posterior longitudinal ligament of the spine: a CT‐based multicenter cross‐sectional study. J Orthop Sci, 2020, 25: 746–750. - PubMed
-
- Kawaguchi Y, Nakano M, Yasuda T, Seki S, Hori T, Kimura T. Ossification of the posterior longitudinal ligament in not only the cervical spine, but also other spinal regions: analysis using multidetector computed tomography of the whole spine. Spine, 2013, 38: E1477–E1482. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

