Tuberculosis infection and disease in South African adolescents with perinatally acquired HIV on antiretroviral therapy: a cohort study
- PMID: 33719199
- PMCID: PMC7957181
- DOI: 10.1002/jia2.25671
Tuberculosis infection and disease in South African adolescents with perinatally acquired HIV on antiretroviral therapy: a cohort study
Abstract
Introduction: There are limited data on Tuberculosis (TB) in adolescents with perinatally acquired HIV (APHIV). We examined the incidence and determinants of TB infection and disease in the Cape Town Adolescent Antiretroviral Cohort (CTAAC).
Methods: Youth between nine and fourteen years on antiretroviral therapy (ART) for more than six months in public sector care, and age-matched HIV-negative adolescents, were enrolled between July 2013 through March 2015 and followed six-monthly. Data were censored on 31 October 2018. Symptom screening, chest radiograph, viral load, CD4 count, QuantiFERON (QFT) and sputum for Xpert MTB/RIF, microscopy, culture and sensitivity were performed annually. TB infection was defined by a QFT of >0.35 IU/mL. TB diagnosis was defined as confirmed (culture or Xpert MTB/RIF positive) or unconfirmed (clinical diagnosis and started on TB treatment). Analyses examined the incidence and determinants of TB infection and disease.
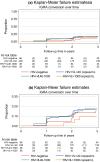
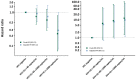
Results: Overall 496 HIV+ and 103 HIV-negative participants (median age at enrolment 12 years (interquartile range, IQR 10.6 to 13.3) were followed for a median of 3.1 years (IQR 3.0 to 3.4); 50% (298/599) were male. APHIV initiated ART at median age 4.4 years (IQR 2.1 to 7.6). At enrolment, 376/496 (76%) had HIV viral load <40 copies/mL, median CD4 count was 713 cells/mm3 and 179/559 (32%) were QFT+, with no difference by HIV status (APHIV 154/468, 33%; HIV negative 25/91, 27%; p = 0.31). The cumulative QFT+ prevalence was similar (APHIV 225/492, 46%; 95%CI 41% to 50%; HIV negative 44/98, 45%; 95% CI 35% to 55%; p = 0.88). APHIV had a higher incidence of all TB disease than HIV-negative adolescents (2.2/100PY, 95% CI 1.6 to 3.1 vs. 0.3/100PY, 95% CI 0.04 to 2.2; IRR 7.36, 95% CI 1.01 to 53.55). The rate of bacteriologically confirmed TB in APHIV was 1.3/100 PY compared to 0.3/100PY for HIV-negative adolescents, suggesting a fourfold increased risk of developing TB disease in APHIV despite access to ART. In addition, a positive QFT at enrolment was not predictive of TB in this population.
Conclusions: High incidence rates of TB disease occur in APHIV despite similar QFT conversion rates to HIV-negative adolescents. Strategies to prevent TB in this vulnerable group must be strengthened.
Keywords: HIV; adolescents; coinfection; incidence; perinatal; tuberculosis.
© 2021 The Authors. Journal of the International AIDS Society published by John Wiley & Sons Ltd on behalf of the International AIDS Society.
Figures

Similar articles
-
Association of prior tuberculosis with cardiovascular status in perinatally HIV-1-infected adolescents.Open Heart. 2024 Nov 14;11(2):e002960. doi: 10.1136/openhrt-2024-002960. Open Heart. 2024. PMID: 39542524 Free PMC article.
-
Cardiopulmonary dysfunction in perinatally HIV-infected South African adolescents on antiretroviral therapy: baseline findings from the Cape Town Adolescent Antiretroviral Cohort.J Int AIDS Soc. 2019 Jul;22(7):e25340. doi: 10.1002/jia2.25340. J Int AIDS Soc. 2019. PMID: 31291058 Free PMC article.
-
Screening for HIV-associated tuberculosis and rifampicin resistance before antiretroviral therapy using the Xpert MTB/RIF assay: a prospective study.PLoS Med. 2011 Jul;8(7):e1001067. doi: 10.1371/journal.pmed.1001067. Epub 2011 Jul 26. PLoS Med. 2011. PMID: 21818180 Free PMC article. Clinical Trial.
-
Mortality of children and adolescents co-infected with tuberculosis and HIV: a systematic review and meta-analysis.AIDS. 2024 Jul 1;38(8):1216-1227. doi: 10.1097/QAD.0000000000003886. Epub 2024 Mar 15. AIDS. 2024. PMID: 38499478
-
Incidence and prevalence of bacteriologically confirmed pulmonary tuberculosis among adolescents and young adults: a systematic review.Epidemiol Infect. 2018 Jun;146(8):946-953. doi: 10.1017/S0950268818000821. Epub 2018 Apr 15. Epidemiol Infect. 2018. PMID: 29655391 Free PMC article.
Cited by
-
3HP preventive treatment among children and adolescents with HIV and child household contacts of TB patients.IJTLD Open. 2024 Sep 1;1(9):413-417. doi: 10.5588/ijtldopen.24.0305. eCollection 2024 Sep. IJTLD Open. 2024. PMID: 39301128 Free PMC article.
-
The Impact of Tuberculosis on the Well-Being of Adolescents and Young Adults.Pathogens. 2021 Dec 8;10(12):1591. doi: 10.3390/pathogens10121591. Pathogens. 2021. PMID: 34959546 Free PMC article. Review.
-
Tuberculosis in Adolescents and Young Adults: Emerging Data on TB Transmission and Prevention among Vulnerable Young People.Trop Med Infect Dis. 2021 Aug 5;6(3):148. doi: 10.3390/tropicalmed6030148. Trop Med Infect Dis. 2021. PMID: 34449722 Free PMC article. Review.
-
HIV-Associated Tuberculosis in Children and Adolescents: Evolving Epidemiology, Screening, Prevention and Management Strategies.Pathogens. 2021 Dec 29;11(1):33. doi: 10.3390/pathogens11010033. Pathogens. 2021. PMID: 35055981 Free PMC article. Review.
-
HIV-associated lung disease.Nat Rev Dis Primers. 2023 Jul 27;9(1):39. doi: 10.1038/s41572-023-00450-5. Nat Rev Dis Primers. 2023. PMID: 37500684 Free PMC article. Review.
References
-
- Marais B, Gie R, Schaaf H, Hesseling AC, Obihara CC, Starke JJ, et al. The natural history of childhood intra‐thoracic tuberculosis: a critical review of literature from the pre‐chemotherapy era [State of the Art]. Int J Tuberc Lung Dis. 2004;8(4):392–402. - PubMed
-
- Snow KJ, Sismanidis C, Denholm J, Sawyer SM, Graham SM. The incidence of tuberculosis among adolescents and young adults: a global estimate. Eur Respir J. 2018;51:1702352. - PubMed
-
- Comstock GW, Livesay VT, Woolpert SF. The prognosis of a positive tuberculin reaction in childhood and adolescence. Am J Epidemiol. 1974;99(2):131–8. - PubMed
-
- Marais BJ, Gie RP, Schaaf HS, Hesseling AC, Obihara CC, Nelson LJ, et al. The clinical epidemiology of childhood pulmonary tuberculosis: a critical review of literature from the pre‐chemotherapy era [State of the Art]. Int J Tuberc Lung Dis. 2004;8(3):278–85. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials

