Chromosomal mosaicism: Origins and clinical implications in preimplantation and prenatal diagnosis
- PMID: 33720449
- PMCID: PMC8176867
- DOI: 10.1002/pd.5931
Chromosomal mosaicism: Origins and clinical implications in preimplantation and prenatal diagnosis
Abstract
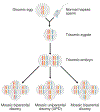
The diagnosis of chromosomal mosaicism in the preimplantation and prenatal stage is fraught with uncertainty and multiple factors need to be considered in order to gauge the likely impact. The clinical effects of chromosomal mosaicism are directly linked to the type of the imbalance (size, gene content, and copy number), the timing of the initial event leading to mosaicism during embryogenesis/fetal development, the distribution of the abnormal cells throughout the various tissues within the body as well as the ratio of normal/abnormal cells within each of those tissues. Additional factors such as assay noise and culture artifacts also have an impact on the significance and management of mosaic cases. Genetic counseling is an important part of educating patients about the likelihood of having a liveborn with a chromosome abnormality and these risks differ according to the time of ascertainment and the tissue where the mosaic cells were initially discovered. Each situation needs to be assessed on a case-by-case basis and counseled accordingly. This review will discuss the clinical impact of finding mosaicism through: embryo biopsy, chorionic villus sampling, amniocentesis, and noninvasive prenatal testing using cell-free DNA.
© 2021 John Wiley & Sons Ltd.
Conflict of interest statement
Figures


References
-
- Benn P, Grati FR. Aneuploidy in first trimester chorionic villi and spontaneous abortions: Windows into the origin and fate of aneuploidy through embryonic and fetal development. Prenat Diagn. 2020. - PubMed
-
- Chatzimeletiou K, Morrison EE, Prapas N, Prapas Y, Handyside AH. Spindle abnormalities in normally developing and arrested human preimplantation embryos in vitro identified by confocal laser scanning microscopy. Human reproduction. 2005;20(3):672–682. - PubMed
-
- Hardy K, Winston RM, Handyside AH. Binucleate blastomeres in preimplantation human embryos in vitro: failure of cytokinesis during early cleavage. J Reprod Fertil. 1993;98(2):549–558. - PubMed
-
- Levy B, Sigurjonsson S, Pettersen B, et al. Genomic imbalance in products of conception: single-nucleotide polymorphism chromosomal microarray analysis. Obstet Gynecol. 2014;124(2 Pt 1):202–209. - PubMed
MeSH terms
Supplementary concepts
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

