Profiles of Intraday Glucose in Type 2 Diabetes and Their Association with Complications: An Analysis of Continuous Glucose Monitoring Data
- PMID: 33720761
- PMCID: PMC9839354
- DOI: 10.1089/dia.2020.0672
Profiles of Intraday Glucose in Type 2 Diabetes and Their Association with Complications: An Analysis of Continuous Glucose Monitoring Data
Abstract
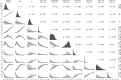
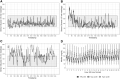
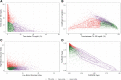
Aims: To identify profiles of type 2 diabetes from continuous glucose monitoring (CGM) data using ambulatory glucose profile (AGP) indicators and examine the association with prevalent complications. Methods: Two weeks of CGM data, collected between 2015 and 2019, from 5901 adult type 2 diabetes patients were retrieved from a clinical database in Chennai, India. Non-negative matrix factorization was used to identify profiles as per AGP indicators. The association of profiles with existing complications was examined using multinomial and logistic regressions adjusted for glycated hemoglobin (HbA1c; %), sex, age at onset, and duration of diabetes. Results: Three profiles of glycemic variability (GV) were identified based on CGM data-Profile 1 ["TIR Profile"] (n = 2271), Profile 2 ["Hypo"] (n = 1471), and Profile 3 ["Hyper"] (n = 2159). Compared with time in range (TIR) profile, those belonging to Hyper had higher mean fasting plasma glucose (202.9 vs. 167.1, mg/dL), 2-h postprandial plasma glucose (302.1 vs. 255.6, mg/dL), and HbA1c (9.7 vs. 8.6; %). Both "Hypo profile" and "Hyper profile" had higher odds of nonproliferative diabetic retinopathy ("Hypo": 1.44, 1.20-1.73; "Hyper": 1.33, 1.11-1.58), macroalbuminuria ("Hypo": 1.58, 1.25-1.98; "Hyper": 1.37, 1.10-1.71), and diabetic kidney disease (DKD; "Hypo": 1.65, 1.18-2.31; "Hyper": 1.88, 1.37-2.58), compared with "TIR profile." Those in "Hypo profile" (vs. "TIR profile") had higher odds of proliferative diabetic retinopathy (PDR; 2.84, 1.65-2.88). Conclusions: We have identified three profiles of GV from CGM data. While both "Hypo profile" and "Hyper profile" had higher odds of prevalent DKD compared with "TIR profile," "Hypo profile" had higher odds of PDR. Our study emphasizes the clinical importance of recognizing and treating hypoglycemia (which is often unrecognized without CGM) in patients with type 2 Diabetes Mellitus.
Keywords: Ambulatory glucose profile; Cluster analysis; Glycemic variability; Time in range.
Conflict of interest statement
No competing financial interests exist.
Figures
References
-
- Anjana RM, Deepa M, Pradeepa R, et al. : Prevalence of diabetes and prediabetes in 15 states of India: results from the ICMR-INDIAB population-based cross-sectional study. Lancet Diabetes Endocrinol 2017;5:585–596. - PubMed
-
- Siegelaar SE, Holleman F, Hoekstra JB, DeVries JH: Glucose variability; does it matter? Endocr Rev 2010;31:171–182. - PubMed
-
- Anjana RM, Kesavadev J, Neeta D, et al. : A multicenter real-life study on the effect of flash glucose monitoring on glycemic control in patients with type 1 and type 2 diabetes. Diabetes Technol Ther 2017;19:533–540. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

