Metabolic Dyslipidemia and Cardiovascular Outcomes in Type 2 Diabetes Mellitus: Findings From the Look AHEAD Study
- PMID: 33728932
- PMCID: PMC8174364
- DOI: 10.1161/JAHA.120.016947
Metabolic Dyslipidemia and Cardiovascular Outcomes in Type 2 Diabetes Mellitus: Findings From the Look AHEAD Study
Erratum in
-
Correction to: Metabolic Dyslipidemia and Cardiovascular Outcomes in Type 2 Diabetes Mellitus: Findings From the Look AHEAD Study.J Am Heart Assoc. 2021 Jul 20;10(14):e020749. doi: 10.1161/JAHA.121.020749. Epub 2021 Jul 6. J Am Heart Assoc. 2021. PMID: 34227401 Free PMC article. No abstract available.
Abstract
Background Metabolic dyslipidemia (high triglyceride) and low high-density lipoprotein cholesterol (HDL-C) is highly prevalent in type 2 diabetes mellitus (T2DM). The extent to which diabetes mellitus-related abnormalities in the triglyceride-HDL-C profile associates with cardiovascular disease (CVD) risk is incompletely understood. We evaluated the associations of triglyceride and HDL-C status with CVD outcomes in individuals with T2DM. Methods and Results We analyzed data from 4199 overweight/obese adults with T2DM free of CVD with available data on triglyceride and HDL-C at baseline (2001-2004) in the Look AHEAD (Action for Health in Diabetes) study. We used Cox proportional models to estimate hazard ratios (HRs) and 95% CIs of: (1) composite CVD outcome (myocardial infarction, stroke, hospitalization for angina, and/or death from cardiovascular causes); (2) coronary artery disease events; and (3) cerebrovascular accidents (stroke). Of the 4199 participants, 62% (n=2600) were women, with a mean age of 58 years (SD, 7), and 40% (n=1659) had metabolic dyslipidemia at baseline. Over a median follow-up of 9.5 years (interquartile range, 8.7-10.3), 500 participants experienced the composite CVD outcome, 396 experienced coronary artery disease events, and 100 experienced stroke. Low HDL-C was associated with higher hazards of the composite CVD outcome (HR, 1.36; 95% CI, 1.12-1.64 [P=0.002]) and coronary artery disease events (HR, 1.46; 95% CI, 1.18-1.81 [P=0.001]) but not stroke (HR, 1.38; 95% CI, 0.90-2.11 [P=0.140]). Compared with patients with normal triglyceride and normal HDL, participants with metabolic dyslipidemia had higher risks of the composite CVD outcome (HR, 1.30; 95% CI, 1.03-1.63 [P=0.025]) and coronary artery disease events (HR, 1.48; 95% CI, 1.14-1.93 [P=0.003]) but not stroke (HR, 1.23; 95% CI, 0.74-2.05 [P=0.420]). Conclusions In a large sample of overweight/obese individuals with T2DM, metabolic dyslipidemia was associated with higher risks of CVD outcomes. Our findings highlight the necessity to account for metabolic dyslipidemia in CVD risk stratification among patients with T2DM. Registration URL: https://www.lookaheadtrial.org; Unique identifier: NCT00017953.
Keywords: cardiovascular disease; diabetes mellitus; metabolic dyslipidemia; type 2.
Conflict of interest statement
The Look AHEAD study was conducted by the Look AHEAD Investigators and supported by the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). The data from the Look AHEAD reported here were supplied by the NIDDK Central Repositories. This manuscript was not prepared in collaboration with Investigators of the Look AHEAD study and does not necessarily reflect the opinions or views of the Look Ahead Study, the NIDDK Central Repositories, or the NIDDK.
Look AHEAD was conducted by the Look AHEAD Research Group and supported by the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK); the National Heart, Lung, and Blood Institute (NHLBI); the National Institute of Nursing Research (NINR); the National Institute of Minority Health and Health Disparities (NIMHD); the Office of Research on Women's Health (ORWH); and the Centers for Disease Control and Prevention (CDC). The data (and samples) from Look AHEAD were supplied by the NIDDK Central Repositories. This manuscript was not prepared under the auspices of the Look AHEAD and does not represent analyses or conclusions of the Look AHEAD Research Group, the NIDDK Central Repositories, or the NIH
Figures
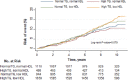

References
-
- Benjamin EJ, Muntner P, Alonso A, Bittencourt MS, Callaway CW, Carson AP, Chamberlain AM, Chang AR, Cheng S, Das SR, et al. Heart disease and stroke statistics‐2019 update: a report from the American Heart Association. Circulation. 2019;139:e56–e528. DOI: 10.1161/CIR.0000000000000659. - DOI - PubMed
-
- Pyŏrälä K, Pedersen TR, Kjekshus J, Faergeman O, Olsson AG, Thorgeirsson G. Cholesterol lowering with simvastatin improves prognosis of diabetic patients with coronary heart disease. A subgroup analysis of the Scandinavian Simvastatin Survival Study (4S). Diabetes Care. 1997;20:614–620. DOI: 10.2337/diacare.20.4.614. - DOI - PubMed
Publication types
MeSH terms
Substances
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

