Comparison of Cancer Prevalence in Patients With Neurofibromatosis Type 1 at an Academic Cancer Center vs in the General Population From 1985 to 2020
- PMID: 33734413
- PMCID: PMC7974640
- DOI: 10.1001/jamanetworkopen.2021.0945
Comparison of Cancer Prevalence in Patients With Neurofibromatosis Type 1 at an Academic Cancer Center vs in the General Population From 1985 to 2020
Abstract
Importance: Neurofibromatosis type 1 (NF1) is a complex genetic disorder that is associated with not only neurofibromas, but also an increased susceptibility to other neoplasms.
Objective: To evaluate the prevalence of neoplasia and outcomes among patients with NF1.
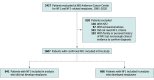
Design, setting, and participants: This cohort study was conducted among patients with NF1 at a single academic cancer center from 1985 to 2020 with median (range) follow-up of 2.9 years (36 days to 30.5 years). Of 2427 patients evaluated for NF1, 1607 patients who met the National Institutes of Health consensus criteria for NF1 were included. This group was compared with estimates from Surveillance, Epidemiology, and End Results (SEER) Cancer Statistics Review 1975 to 2015 and SEER participants database unless otherwise specified. Data were analyzed from August 2018 to March 2020.
Main outcomes and measures: Disease-specific survival (DSS) was measured from diagnosis date to date of neoplasm-specific death or censorship and calculated using the Kaplan-Meier method. Survival curves were compared using the log-rank test. Deaths from disease were considered a DSS end point; other deaths were considered censored observations. Secondary outcome measures were comparisons of (1) overall survival of patients with NF1 with neurofibroma neoplasms vs those without nonneurofibroma neoplasms, (2) neoplasm prevalence in the NF1 group vs general population estimates, and (3) age at diagnosis in the NF1 group vs general population estimates for the most common neoplasms in the NF1 group.
Results: Among 1607 patients with NF1, the median (range) age at initial visit was 19 years (1 month to 83 years) and 840 (52.3%) were female patients. Among 666 patients who developed other neoplasms in addition to neurofibromas (41.4%), 295 patients (18.4%) developed glioma and 243 patients (15.1%) developed malignant peripheral nerve sheath tumor (MPNST), the most common neoplasms. Patients with NF1, compared with the general population, developed several neoplasms at a younger mean (SD) age (low-grade glioma: 12.98 [11.09] years vs 37.76 [24.53] years; P < .0001; high-grade glioma [HGG]: 27.31 [15.59] years vs 58.42 [19.09] years; P < .0001; MPNST: 33.88 [14.80] years vs 47.06 [20.76] years; P < .0001; breast cancer: 46.61 [9.94] years vs 61.71 [13.85] years; P < .0001). Patients with NF1 developed neoplasms more frequently compared with the general population (odds ratio, 9.5; 95% CI, 8.5-10.5; P < .0001). Among patients with NF1, significantly lower 5-year DSS rates were found among those with undifferentiated pleomorphic sarcoma (1 of 5 patients [20.0%]), HGG (8 of 34 patients [23.1%]), MPNST (72 of 228 patients [31.6%]), ovarian carcinoma (4 of 7 patients [57.1%]), and melanoma (8 of 12 patients [66.7%]) compared with those who had neoplasms classified as other (110 of 119 patients [92.4%]) (all P < .001) .
Conclusions and relevance: This cohort study found that among patients with NF1, those who developed undifferentiated pleomorphic sarcoma, HGG, MPNST, ovarian carcinoma, or melanoma had significantly lower DSS rates compared with those who developed other neoplasms. This study also found that patients with NF1 developed some neoplasms more frequently and at a younger age compared with individuals without NF1. HGGs and MPNST were noteworthy causes of death among patients NF1. This information may be useful for NF1 patient counseling and follow-up.
Conflict of interest statement
Figures

Comment in
-
Cancer and Neurofibromatosis Type 1-Confirming What We Knew and Telling Us Something New.JAMA Netw Open. 2021 Mar 1;4(3):e211061. doi: 10.1001/jamanetworkopen.2021.1061. JAMA Netw Open. 2021. PMID: 33734408 No abstract available.
References
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

