Prediction of extubation outcome in mechanically ventilated patients: Development and validation of the Extubation Predictive Score (ExPreS)
- PMID: 33735250
- PMCID: PMC7971695
- DOI: 10.1371/journal.pone.0248868
Prediction of extubation outcome in mechanically ventilated patients: Development and validation of the Extubation Predictive Score (ExPreS)
Abstract
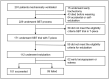
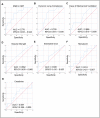
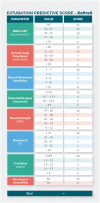
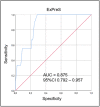
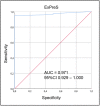
Despite the best efforts of intensive care units (ICUs) professionals, the extubation failure rates in mechanically ventilated patients remain in the range of 5%-30%. Extubation failure is associated with increased risk of death and longer ICU stay. This study aimed to identify respiratory and non-respiratory parameters predictive of extubation outcome, and to use these predictors to develop and validate an "Extubation Predictive Score (ExPreS)" that could be used to predict likelihood of extubation success in patients receiving invasive mechanical ventilation (IMV). Derivation cohort was composed by patients aged ≥18 years admitted to the ICU and receiving IMV through an endotracheal tube for >24 hours. The weaning process followed the established ICU protocol. Clinical signs and ventilator parameters of patients were recorded during IMV, in the end phase of weaning in pressure support ventilation (PSV) mode, with inspiratory pressure of 7 cm H2O over the PEEP (positive end expiratory pressure). Patients who tolerated this ventilation were submitted to spontaneous breathing trial (SBT) with T-tube for 30 minutes. Those who passed the SBT and a subsequent cuff-leak test were extubated. The primary outcome of this study was extubation success at 48 hours. Parameters that showed statistically significant association with extubation outcome were further investigated using the receiver operating characteristics (ROC) analysis to assess their predictive value. The area under the curve (AUC) values were used to select parameters for inclusion in the ExPreS. Univariable logistic regression analysis and ROC analysis were performed to evaluate the performance of ExPreS. Patients' inclusion and statistical analyses for the prospective validation cohort followed the same criteria used for the derivation cohort and the decision to extubate was based on the ExPreS result. In the derivation cohort, a total of 110 patients were extubated: extubation succeeded in 101 (91.8%) patients and failed in 9 (8.2%) patients. Rapid shallow-breathing index (RSBI) in SBT, dynamic lung compliance, duration of IMV, muscle strength, estimated GCS, hematocrit, and serum creatinine were significantly associated with extubation outcome. These parameters, along with another parameter-presence of neurologic comorbidity-were used to create the ExPreS. The AUC value for the ExPreS was 0.875, which was higher than the AUCs of the individual parameters. The total ExPreS can range from 0 to 100. ExPreS ≥59 points indicated high probability of success (OR = 23.07), while ExPreS ≤44 points indicated low probability of success (OR = 0.82). In the prospective validation cohort, 83 patients were extubated: extubation succeeded in 81 (97.6%) patients and failed in 2 (2.4%) patients. The AUC value for the ExPreS in this cohort was 0.971. The multiparameter score that we propose, ExPreS, shows good accuracy to predict extubation outcome in patients receiving IMV in the ICU. In the prospective validation, the use of ExPreS decreased the extubation failure rate from 8.2% to 2.4%, even in a cohort of more severe patients.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures


Similar articles
-
[Correlation analysis between mechanical power normalized to dynamic lung compliance and weaning outcomes and prognosis in mechanically ventilated patients: a prospective, observational cohort study].Zhonghua Wei Zhong Bing Ji Jiu Yi Xue. 2025 Jan;37(1):36-42. doi: 10.3760/cma.j.cn121430-20240126-00085. Zhonghua Wei Zhong Bing Ji Jiu Yi Xue. 2025. PMID: 39968584 Chinese.
-
Improvement in the Prediction of Ventilator Weaning Outcomes by an Artificial Neural Network in a Medical ICU.Respir Care. 2015 Nov;60(11):1560-9. doi: 10.4187/respcare.03648. Epub 2015 Sep 1. Respir Care. 2015. PMID: 26329358
-
A decision-tree model for predicting extubation outcome in elderly patients after a successful spontaneous breathing trial.Anesth Analg. 2010 Nov;111(5):1211-8. doi: 10.1213/ANE.0b013e3181f4e82e. Epub 2010 Sep 14. Anesth Analg. 2010. PMID: 20841406
-
Automatic Tube Compensation During Spontaneous Breathing Trials.Respir Care. 2022 Oct;67(10):1335-1342. doi: 10.4187/respcare.09920. Epub 2022 Jun 21. Respir Care. 2022. PMID: 36137582 Review.
-
Predictive factors of weaning from mechanical ventilation and extubation outcome: A systematic review.J Crit Care. 2018 Dec;48:56-62. doi: 10.1016/j.jcrc.2018.08.023. Epub 2018 Aug 20. J Crit Care. 2018. PMID: 30172034
Cited by
-
Development and validation of a mechanical power-oriented prediction model of weaning failure in mechanically ventilated patients: a retrospective cohort study.BMJ Open. 2022 Dec 15;12(12):e066894. doi: 10.1136/bmjopen-2022-066894. BMJ Open. 2022. PMID: 36521885 Free PMC article. Clinical Trial.
-
Work of Breathing During Proportional Assist Ventilation as a Predictor of Extubation Failure.Respir Care. 2023 Aug;68(8):1049-1057. doi: 10.4187/respcare.10225. Epub 2023 May 9. Respir Care. 2023. PMID: 37160340 Free PMC article.
-
Multitask learning to predict successful weaning in critically ill ventilated patients: A retrospective analysis of the MIMIC-IV database.Digit Health. 2024 Oct 8;10:20552076241289732. doi: 10.1177/20552076241289732. eCollection 2024 Jan-Dec. Digit Health. 2024. PMID: 39381828 Free PMC article.
-
Analysis of the Cardiorespiratory Pattern of Patients Undergoing Weaning Using Artificial Intelligence.Int J Environ Res Public Health. 2023 Mar 1;20(5):4430. doi: 10.3390/ijerph20054430. Int J Environ Res Public Health. 2023. PMID: 36901440 Free PMC article.
-
Biosignal-Based Digital Biomarkers for Prediction of Ventilator Weaning Success.Int J Environ Res Public Health. 2021 Sep 1;18(17):9229. doi: 10.3390/ijerph18179229. Int J Environ Res Public Health. 2021. PMID: 34501829 Free PMC article.
References
-
- MacIntyre NR, Cook DJ, Ely EW, Epstein SK, Fink JB, Heffner JE, et al.. Evidence-based guidelines for weaning and discontinuing ventilatory support: a collective task force facilitated by the American College of Chest Physicians; the American Association for Respiratory Care; and the American College of Critical Care Medicine. Chest. 2001;120: 375S–95S. 10.1378/chest.120.6_suppl.375s - DOI - PubMed
-
- Fernandez MM, González-Castro A, Magret M, Bouza MT, Ibañez M, García C, et al.. Reconnection to mechanical ventilation for 1 h after a successful spontaneous breathing trial reduces reintubation in critically ill patients: a multicenter randomized controlled trial. Intensive Care Med. 2017;43: 1660–1667. 10.1007/s00134-017-4911-0 - DOI - PubMed
-
- Quintard H, L’Her E, Pottecher J, Adnet F, Constantin J-M, De Jong A, et al.. Experts’ guidelines of intubation and extubation of the ICU patient of French Society of Anaesthesia and Intensive Care Medicine (SFAR) and French-speaking Intensive Care Society (SRLF). Ann Intensive Care. 2019;9: 13. 10.1186/s13613-019-0483-1 - DOI - PMC - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

