Multi-organ Coordination of Lipoprotein Secretion by Hormones, Nutrients and Neural Networks
- PMID: 33743013
- PMCID: PMC8599201
- DOI: 10.1210/endrev/bnab008
Multi-organ Coordination of Lipoprotein Secretion by Hormones, Nutrients and Neural Networks
Abstract
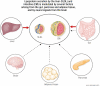
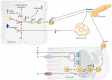
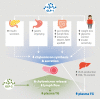
Plasma triglyceride-rich lipoproteins (TRL), particularly atherogenic remnant lipoproteins, contribute to atherosclerotic cardiovascular disease. Hypertriglyceridemia may arise in part from hypersecretion of TRLs by the liver and intestine. Here we focus on the complex network of hormonal, nutritional, and neuronal interorgan communication that regulates secretion of TRLs and provide our perspective on the relative importance of these factors. Hormones and peptides originating from the pancreas (insulin, glucagon), gut [glucagon-like peptide 1 (GLP-1) and 2 (GLP-2), ghrelin, cholecystokinin (CCK), peptide YY], adipose tissue (leptin, adiponectin) and brain (GLP-1) modulate TRL secretion by receptor-mediated responses and indirectly via neural networks. In addition, the gut microbiome and bile acids influence lipoprotein secretion in humans and animal models. Several nutritional factors modulate hepatic lipoprotein secretion through effects on the central nervous system. Vagal afferent signaling from the gut to the brain and efferent signals from the brain to the liver and gut are modulated by hormonal and nutritional factors to influence TRL secretion. Some of these factors have been extensively studied and shown to have robust regulatory effects whereas others are "emerging" regulators, whose significance remains to be determined. The quantitative importance of these factors relative to one another and relative to the key regulatory role of lipid availability remains largely unknown. Our understanding of the complex interorgan regulation of TRL secretion is rapidly evolving to appreciate the extensive hormonal, nutritional, and neural signals emanating not only from gut and liver but also from the brain, pancreas, and adipose tissue.
Keywords: adipose; brain; chylomicrons; gut peptides; pancreas; very-low density lipoproteins.
© The Author(s) 2021. Published by Oxford University Press on behalf of the Endocrine Society. All rights reserved. For permissions, please e-mail: journals.permissions@oup.com.
Figures
Similar articles
-
Regulation of intestinal lipid and lipoprotein metabolism by the proglucagon-derived peptides glucagon like peptide 1 and glucagon like peptide 2.Curr Opin Lipidol. 2018 Apr;29(2):95-103. doi: 10.1097/MOL.0000000000000495. Curr Opin Lipidol. 2018. PMID: 29432213 Free PMC article. Review.
-
New and emerging regulators of intestinal lipoprotein secretion.Atherosclerosis. 2014 Apr;233(2):608-615. doi: 10.1016/j.atherosclerosis.2013.12.047. Epub 2014 Jan 21. Atherosclerosis. 2014. PMID: 24534456 Review.
-
Central Nervous System Regulation of Intestinal Lipoprotein Metabolism by Glucagon-Like Peptide-1 via a Brain-Gut Axis.Arterioscler Thromb Vasc Biol. 2015 May;35(5):1092-100. doi: 10.1161/ATVBAHA.114.304873. Epub 2015 Feb 12. Arterioscler Thromb Vasc Biol. 2015. PMID: 25675997
-
GLP-1 attenuates intestinal fat absorption and chylomicron production via vagal afferent nerves originating in the portal vein.Mol Metab. 2022 Nov;65:101590. doi: 10.1016/j.molmet.2022.101590. Epub 2022 Sep 5. Mol Metab. 2022. PMID: 36067913 Free PMC article.
-
Regulation of glucagon-like peptide-1-(7-36) amide, peptide YY, and neurotensin secretion by neurotransmitters and gut hormones in the isolated vascularly perfused rat ileum.Endocrinology. 1995 Nov;136(11):5182-8. doi: 10.1210/endo.136.11.7588257. Endocrinology. 1995. PMID: 7588257
Cited by
-
Glucagon-Like-Peptide-2 Stimulates Lacteal Contractility and Enhances Chylomicron Transport in the Presence of an Intact Enteric Nervous System.Gastro Hep Adv. 2024 Jun 29;3(7):954-964. doi: 10.1016/j.gastha.2024.06.009. eCollection 2024. Gastro Hep Adv. 2024. PMID: 39286622 Free PMC article.
-
Tracers and Imaging of Fatty Acid and Energy Metabolism of Human Adipose Tissues.Physiology (Bethesda). 2024 Mar 1;39(2):0. doi: 10.1152/physiol.00012.2023. Epub 2023 Dec 19. Physiology (Bethesda). 2024. PMID: 38113392 Free PMC article. Review.
-
The chylomicron saga: time to focus on postprandial metabolism.Front Endocrinol (Lausanne). 2024 Jan 18;14:1322869. doi: 10.3389/fendo.2023.1322869. eCollection 2023. Front Endocrinol (Lausanne). 2024. PMID: 38303975 Free PMC article. Review.
-
GLP-2 regulation of intestinal lipid handling.Front Physiol. 2024 Feb 14;15:1358625. doi: 10.3389/fphys.2024.1358625. eCollection 2024. Front Physiol. 2024. PMID: 38426205 Free PMC article. Review.
-
Fibroblast growth factor 21: update on genetics and molecular biology.Curr Opin Lipidol. 2025 Apr 1;36(2):88-95. doi: 10.1097/MOL.0000000000000960. Epub 2024 Oct 23. Curr Opin Lipidol. 2025. PMID: 39450972 Free PMC article. Review.
References
-
- Xiao C, Dash S, Morgantini C, Hegele RA, Lewis GF. Pharmacological targeting of the atherogenic dyslipidemia complex: the next Frontier in CVD prevention beyond lowering LDL cholesterol. Diabetes. 2016;65(7):1767-1778. - PubMed
-
- Stahel P, Xiao C, Hegele RA, Lewis GF. The atherogenic dyslipidemia complex and novel approaches to cardiovascular disease prevention in diabetes. Can J Cardiol. 2018;34(5):595-604. - PubMed
-
- Xiao C, Stahel P, Carreiro AL, Buhman KK, Lewis GF. Recent advances in triacylglycerol mobilization by the gut. Trends Endocrinol Metab. 2018;29(3):151-163. - PubMed
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

