Ocular coloboma-a comprehensive review for the clinician
- PMID: 33746210
- PMCID: PMC8302742
- DOI: 10.1038/s41433-021-01501-5
Ocular coloboma-a comprehensive review for the clinician
Abstract
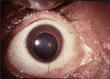
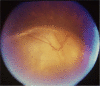
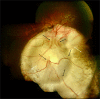
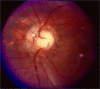
Typical ocular coloboma is caused by defective closure of the embryonal fissure. The occurrence of coloboma can be sporadic, hereditary (known or unknown gene defects) or associated with chromosomal abnormalities. Ocular colobomata are more often associated with systemic abnormalities when caused by chromosomal abnormalities. The ocular manifestations vary widely. At one extreme, the eye is hardly recognisable and non-functional-having been compressed by an orbital cyst, while at the other, one finds minimalistic involvement that hardly affects the structure and function of the eye. In the fundus, the variability involves the size of the coloboma (anteroposterior and transverse extent) and the involvement of the optic disc and fovea. The visual acuity is affected when coloboma involves disc and fovea, or is complicated by occurrence of retinal detachment, choroidal neovascular membrane, cataract, amblyopia due to uncorrected refractive errors, etc. While the basic birth anomaly cannot be corrected, most of the complications listed above are correctable to a great extent. Current day surgical management of coloboma-related retinal detachments has evolved to yield consistently good results. Cataract surgery in these eyes can pose a challenge due to a combination of microphthalmos and relatively hard lenses, resulting in increased risk of intra-operative complications. Prophylactic laser retinopexy to the border of choroidal coloboma appears to be an attractive option for reducing risk of coloboma-related retinal detachment. However, a majority of the eyes have the optic disc within the choroidal coloboma, thus making it difficult to safely administer a complete treatment.
摘要: 典型的眼组织缺损是由胚胎裂闭合不全引起的。眼组织缺损可以为偶发、遗传性 (已知或未知的基因缺陷)或与染色体异常有关。眼组织缺损多与染色体异常引起的全身异常有关。眼部表现差异多样。比如被眼眶囊肿压迫时, 其中一眼几乎无法视物、视觉功能丧失, 而另一只眼的结构和功能却丝毫不受影响。眼底的变异性则涉及到组织缺损的大小(前后和横向的范围)以及视盘和黄斑中心凹的受累程度。当组织缺损累及视盘和黄斑的中心凹时, 或合并视网膜脱离、脉络膜新生血管膜、白内障、因屈光不正引起的弱视等, 则会影响视力。虽然眼组织先天性异常无法治疗, 但上述大多数并发症在很大程度上是可以治疗的。目前, 组织缺损相关性视网膜脱离的手术治疗已经取得了良好的效果。但由于先天性小眼球和相对坚硬的晶状体, 白内障手术具有一定的挑战性, 从而增加了术中并发症的风险。脉络膜缺损边缘的预防性激光光凝治疗对于降低组织缺损相关性视网膜脱离的发病风险是一种不错的选择。然而, 大部分患眼的视盘都在脉络膜的缺损范围内, 因此很难安全的进行完整的治疗。.
© 2021. The Author(s).
Conflict of interest statement
The authors declare no competing interests.
Figures


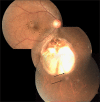
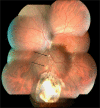
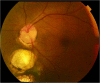
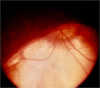
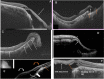
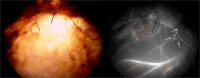
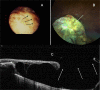


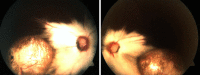
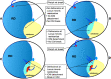
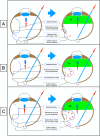

References
-
- Duke-Elder S. Anomalous closure of embryonal cleft—typical colobomata. In: System of ophthalmology. St Louis: CV Mosby company; 1963. p. 456–88.
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

