Testicular, Spermatic Cord, and Scrotal Soft Tissue Sarcomas: Treatment Outcomes and Patterns of Failure
- PMID: 33746565
- PMCID: PMC7954631
- DOI: 10.1155/2021/8824301
Testicular, Spermatic Cord, and Scrotal Soft Tissue Sarcomas: Treatment Outcomes and Patterns of Failure
Abstract
Introduction: Paratesticular sarcomas are defined as tumors that arise within the scrotum and include the subsites of epididymis, spermatic cord, and tunica vaginalis and represent the most common type of GU sarcoma. The mainstay of treatment is often surgical resection, combined with histology specific chemotherapy and radiotherapy. Due to the rare nature of the disease, there are limited data to guide management. We present our single-institution retrospective experience regarding the management and treatment of paratesticular sarcomas.
Materials and methods: We queried our oncology registry database for patients treated for testicular, spermatic cord, and scrotal soft tissue sarcomas between 1971 and 2017. Patients in this series had pathological confirmation of a sarcoma diagnosis by a sarcoma-specialized pathologist. Only patients with localized disease were included in this analysis with the exception of patients with a diagnosis of rhabdomyosarcoma where patients with both localized and metastatic disease were included on this study.
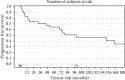
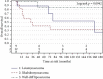
Results: A total of 34 patients were included in this retrospective analysis. The median was 24 (range, 5-78), and the median tumor size was 6.25 cm. Twenty-six patients had localized disease (76.6%) at the time of diagnosis. A predominance of patients had tumors involving the spermatic cord (45.5%), and the most common histology was rhabdomyosarcoma (35.3%), leiomyosarcoma (26.5%), and well-differentiated liposarcoma (23.5%). The median follow-up was 71.0 months (range, 2.5-534.4 months). A total of 7 patients experienced an isolated local failure (20.6%), four patients developed distant metastatic disease (11.8%), and one patient (2.9%) with synovial sarcoma of the spermatic cord experienced a regional recurrence. The median progression-free survival (PFS) was 99.6 months, 95% CI (45.8-534.3 months), with a three-year PFS rate of 71%, 95% CI (53%-83%), and a 5-year PFS rate of 64% (range, 46%-78%). We did not find any statistically significant associations based on surgery type (p=0.15), the use of chemotherapy, (p=0.36), or final margin status (p=0.21). Two patients who were treated with preoperative radiotherapy had significant wound healing complication with chronic sinus tracts, though these patients did not experience a local recurrence.
Conclusions: We provide a characterization of the natural history and treatment patterns of paratesticular sarcomas. While effective at reducing a local recurrence, preoperative radiotherapy was associated with significant toxicity. As a result, we prefer the use of postoperative radiotherapy in patients as clinically indicated. We did not find any specific treatment patterns associated with an improvement in clinical outcomes.
Copyright © 2021 Varun K. Chowdhry et al.
Conflict of interest statement
The authors report no conflicts of interest with this work.
Figures
References
-
- Gomez-Rivera F., Shellenberger T. D., Sturgis E. M. Genitourinary sarcomas. In: Rollock R. E., Randall R. L., O’Sullivan B., editors. Sarcoma Oncology: Multidisciplinary Approach. Raleigh, NC, USA: PMPHUA; 2019. pp. 229–230.
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials