Physiological and Immunological Causes of the Susceptibility of Chronic Inflammatory Patients to COVID-19 Infection: Focus on Diabetes
- PMID: 33746897
- PMCID: PMC7971178
- DOI: 10.3389/fendo.2021.576412
Physiological and Immunological Causes of the Susceptibility of Chronic Inflammatory Patients to COVID-19 Infection: Focus on Diabetes
Abstract
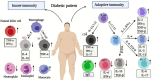
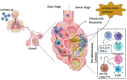
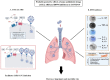
The coronavirus disease 2019 (COVID-19) pandemic has recently emerged, which was then spread rapidly in more than 190 countries worldwide so far. According to the World Health Organization, 3,232,062 global cases of COVID-19 were confirmed on April 30th with a mortality rate of 3.4%. Notably, the symptoms are almost similar to those of flu such as fever, cough, and fatigue. Unfortunately, the global rates of morbidity and mortality caused by this disease are more and still increasing on a daily basis. The rates for patients suffering from inflammatory diseases like diabetes, is even further, due to their susceptibility to the pathogenesis of COVID-19. In this review, we attempted to focus on diabetes to clarify the physiological and immunological characteristics of diabetics before and after the infection with COVID-19. We hope these conceptions could provide a better understanding of the mechanisms involved in COVID-19 susceptibility and increase the awareness of risk to motivate behavior changes in vulnerable people for enhancing the prevention. Up to now, the important role of immune responses, especially the innate ones, in the development of the worst signs in COVID-19 infection have been confirmed. Therefore, to better control patients with COVID-19, it is recommended to consider a history of chronic inflammatory diseases as well as the way of controlling immune response in these patients.
Keywords: ACE2; COVID-19; chronic inflammatory disease; diabetes; immune responses.
Copyright © 2021 Rahmani-Kukia and Abbasi.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
References
-
- Gorbalenya AE. Severe acute respiratory syndrome-related coronavirus–The species and its viruses, a statement of the Coronavirus Study Group. BioRxiv (2020) 937862:1–16. 10.1101/2020.02.07.937862v1 - DOI
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

