Difference in Resident Versus Attending Perspective of Competency and Autonomy During Arthroscopic Rotator Cuff Repairs
- PMID: 33748637
- PMCID: PMC7963494
- DOI: 10.2106/JBJS.OA.20.00014
Difference in Resident Versus Attending Perspective of Competency and Autonomy During Arthroscopic Rotator Cuff Repairs
Abstract
A noted deficiency in orthopaedic resident education is a lack of intraoperative autonomy; however, no studies exist evaluating this issue. The purpose of this study was to determine whether there is a difference between resident and attending perception of resident competency and autonomy during arthroscopic rotator cuff repairs and whether increased perceived competency leads to more autonomy.
Methods: This study included 21 orthopaedic residents and 7 attendings from a single residency program. A survey was developed that included the previously validated Ottawa Surgical Competency Operating Room Evaluation (O-SCORE) and implemented novel arthroscopic rotator cuff repair questions concerning 5 key procedural steps determined by attendings. The survey assessed resident and attending perception of percent opportunity given and percent completed of each step and whether the resident could complete the surgery independently. Paired comparisons were conducted using the Wilcoxon signed-rank test. Agreement between residents and attendings was calculated using a linear-weighted Gwet's AC2. A secondary analysis investigated resident perception of autonomy stratified by attending perception of competency using Kruskal-Wallis tests.
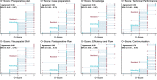
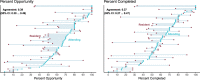
Results: One hundred forty-two surveys were completed over one academic year. Residents reported a 4-point higher median O-SCORE (34) than attendings (30; p < 0.01; agreement = 0.63). Residents perceived less opportunity compared with attendings, with a median opportunity to complete each step of 54% vs. 70% (p < 0.01; agreement = 0.39). Residents also perceived lower percent completed of the key steps compared with attendings, with medians of 52% vs. 61% (p < 0.01; agreement = 0.37). Resident perceived opportunity increased with higher attending reported O-SCOREs (p < 0.01) and percent completion of the key steps (p < 0.01). No statistically significant increase in perceived opportunity was observed the with post-graduate year (PGY) level (p = 0.35).
Discussion: This study demonstrated a significant difference in perception between residents and attendings regarding resident competency and autonomy during arthroscopic rotator cuff repairs. It also demonstrated that with increasing attending perception of competency, there was an increasing resident perception of autonomy, but there was no statistically significant difference of perceived autonomy based on the PGY-level.
Copyright © 2021 The Authors. Published by The Journal of Bone and Joint Surgery, Incorporated. All rights reserved.
Conflict of interest statement
Disclosure: The Disclosure of Potential Conflicts of Interest forms are provided with the online version of the article (http://links.lww.com/JBJSOA/A210).
Figures
References
-
- Hamdorf JM, Hall JC. Acquiring surgical skills. Br J Surg. 2000;87(1):28-37. - PubMed
-
- Hashimoto DA, Bynum WEt, Lillemoe KD, Sachdeva AK. See more, do more, teach more: surgical resident autonomy and the transition to independent practice. Acad Med. 2016;91(6):757-60. - PubMed
-
- Mattar SG, Alseidi AA, Jones DB, Jeyarajah DR, Swanstrom LL, Aye RW, Wexner SD, Martinez JM, Ross SB, Awad MM, Franklin ME, Arregui ME, Schirmer BD, Minter RM. General surgery residency inadequately prepares trainees for fellowship: results of a survey of fellowship program directors. Ann Surg. 2013;258(3):440-9. - PubMed
-
- Atesok K, Mabrey JD, Jazrawi LM, Egol KA. Surgical simulation in orthopaedic skills training. J Am Acad Orthop Surg. 2012;20(7):410-22. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources
