Analgesic Effect of Noninvasive Brain Stimulation for Neuropathic Pain Patients: A Systematic Review
- PMID: 33751453
- PMCID: PMC8119533
- DOI: 10.1007/s40122-021-00252-1
Analgesic Effect of Noninvasive Brain Stimulation for Neuropathic Pain Patients: A Systematic Review
Abstract
Introduction: The objective of this review is to systematically summarize the consensus on best practices for different NP conditions of the two most commonly utilized noninvasive brain stimulation (NIBS) technologies, repetitive transcranial magnetic stimulation (rTMS), and transcranial direct current stimulation (tDCS).
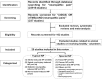
Methods: PubMed was searched according to the predetermined keywords and criteria. Only English language studies and studies published up to January 31, 2020 were taken into consideration. Meta-analyses, reviews, and systematic reviews were excluded first, and those related to animal studies or involving healthy volunteers were also excluded. Finally, 29 studies covering 826 NP patients were reviewed.
Results: The results from the 24 enrolled studies and 736 NP patients indicate that rTMS successfully relieved the pain symptoms of 715 (97.1%) NP patients. Also, five studies involving 95 NP patients (81.4%) also showed that tDCS successfully relieved NP. In the included studied, the M1 region plays a key role in the analgesic treatment of NIBS. The motor evoked potentials (MEPs), the 10-20 electroencephalography system (EEG 10/20 system), and neuro-navigation methods are used in clinical practice to locate therapeutic targets. Based on the results of the review, the stimulation parameters of rTMS that best induce an analgesic effect are a stimulation frequency of 10-20 Hz, a stimulation intensity of 80-120% of RMT, 1000-2000 pulses, and 5-10 sessions, and the most effective parameters of tDCS are a current intensity of 2 mA, a session duration of 20-30 min, and 5-10 sessions.
Conclusions: Our systematically reviewed the evidence for positive and negative responses to rTMS and tDCS for NP patient care and underscores the analgesic efficacy of NIBS in patients with NP. The treatment of NP should allow the design of optimal treatments for individual patients.
Keywords: Neuropathic pain; Noninvasive brain stimulation; Repetitive transcranial magnetic stimulation; Review; Transcranial direct current stimulation.
Figures


References
-
- Lefaucheur JP, André-Obadia N, Antal A, et al. Evidence-based guidelines on the therapeutic use of repetitive transcranial magnetic stimulation (rTMS) Clin Neurophysiol. 2014;125(11):2150–2206. - PubMed
-
- Gilron I, Baron R, Jensen T. Neuropathic pain: principles of diagnosis and treatment. Mayo Clin Proc. 2015;90(4):532–545. - PubMed
-
- Costa B, Ferreira I, Trevizol A, Thibaut A, Fregni F. Emerging targets and uses of neuromodulation for pain. Expert Rev Neurother. 2019;19(2):109–118. - PubMed
-
- Reincke H, Nelson KR. Duchenne de Boulogne: electrodiagnosis of poliomyelitis. Muscle Nerve. 1990;13(1):56–62. - PubMed
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

