Association of CYP2B6 Genetic Variation with Efavirenz and Nevirapine Drug Resistance in HIV-1 Patients from Botswana
- PMID: 33758532
- PMCID: PMC7981136
- DOI: 10.2147/PGPM.S289471
Association of CYP2B6 Genetic Variation with Efavirenz and Nevirapine Drug Resistance in HIV-1 Patients from Botswana
Erratum in
-
Erratum: Association of CYP2B6 Genetic Variation with Efavirenz and Nevirapine Drug Resistance in HIV-1 Patients from Botswana [Corrigendum].Pharmgenomics Pers Med. 2021 Mar 31;14:395. doi: 10.2147/PGPM.S312741. eCollection 2021. Pharmgenomics Pers Med. 2021. PMID: 33833550 Free PMC article.
Abstract
Purpose: CYP2B6 liver enzyme metabolizes the two non-nucleoside reverse transcriptase inhibitors Efavirenz (EFV) and Nevirapine (NVP) used in the antiretroviral therapy (ART) regimens for HIV-infected individuals. Polymorphisms of the CYP2B6 gene influence drug levels in plasma and possibly virological outcomes. The aim of this study was to explore the potential impact of CYP2B6 genotype and haplotype variation on the risk of developing EFV/NVP drug resistance mutations (DRMs) in HIV-1 patients receiving EFV-/NVP-containing regimens in Botswana.
Patients and methods: Participants were a sub-sample of a larger study (Tshepo study) conducted in Gaborone, Botswana, among HIV-infected individuals taking EFV/NVP containing ART. Study samples were retrieved and assigned to cases (with DRMs) and controls (without DRMs). Four single-nucleotide polymorphisms (SNPs) in the CYP2B6 gene (-82T>C; 516G>T; 785A>G; 983T>C) were genotyped, the haplotypes reconstructed, and the metabolic score assigned. The possible association between drug resistance and several independent factors (baseline characteristics and CYP2B6 genotypes) was assessed by Binary Logistic Regression (BLR) analysis. EFV/NVP resistance status and CYP2B6 haplotypes were also analyzed using Z-test, chi-square and Fisher's exact test statistics.
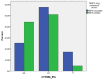
Results: Two hundred and twenty-seven samples were analysed (40 with DRMs, 187 without DRMs). BLR analysis showed an association between EFV/NVP resistance and CYP2B6 516G allele (OR: 2.26; 95% CI: 1.27-4.01; P=0.005). Moreover, haplotype analysis revealed that the proportion of EFV/NVP-resistant infections was higher among CYP2B6 fast than extensive/slow metabolizers (30.8% vs 16.8%; P=0.035), with the 516G allele more represented in the haplotypes of fast than extensive/slow metabolizers (100.0% vs 53.8%; P<0.001).
Conclusion: We demonstrated that the CYP2B6 516G allele, and even more when combined in fast metabolic haplotypes, is associated with the presence of EFV/NVP resistance, strengthening the need to assess the CYP2B6 genetic profiles in HIV-infected patients in order to improve the virologic outcomes of NNRTI containing ART.
Keywords: ART; CYP2B6 gene; HIV; drug resistance selection; fast metabolizers.
© 2021 Maseng et al.
Conflict of interest statement
The authors report no conflicts of interest in this work.
Figures
References
-
- UNAIDS, 2020. UNAIDS data. 2020. Available from: https://www.unaids.org/sites/default/files/media_asset/2020_aids-data-bo.... Accessed March8, 2021.
-
- WHO, World Health Organization. Antiretroviral therapy coverage estimates by WHO region. 2020. Available from: https://apps.who.int/gho/data/view.main.23300REGION?lang=en. Accessed September15, 2020.
-
- WHO, World Health Organization. HIV drug resistance report 2019. 2019. Available from: https://www.who.int/hiv/pub/drugresistance/hivdr-report-2019/en/. Accessed September15, 2020.
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources