TRANSHIATAL ESOPHAGECTOMY IN SQUAMOUS CELL CARCINOMA OF THE ESOPHAGUS: WHAT ARE THE BEST INDICATIONS?
- PMID: 33759957
- PMCID: PMC7983525
- DOI: 10.1590/0102-672020200004e1567
TRANSHIATAL ESOPHAGECTOMY IN SQUAMOUS CELL CARCINOMA OF THE ESOPHAGUS: WHAT ARE THE BEST INDICATIONS?
Abstract
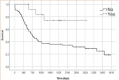
Background: Overall survival in patients who underwent transhiatal esophagectomy submitted or not to neoadjuvant therapy. Southern Brazil has one of the highest incidences of esophageal squamous cell carcinoma in the world. Transthoracic esophagectomy allows more complete abdominal and thoracic lymphadenectomy than transhiatal. However, this one is associated with less morbidity.
Aim: To analyze the outcomes and prognostic factors of squamous esophageal cancer treated with transhiatal procedure.
Methods: All patients selected for transhiatal approach were included as a potentially curative treatment and overall survival, operative time, lymph node analysis and use of neoadjuvant therapy were analyzed.
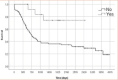
Results: A total of 96 patients were evaluated. The overall 5-year survival was 41.2%. Multivariate analysis showed that operative time and presence of positive lymph nodes were both associated with a worse outcome, while neoadjuvant therapy was associated with better outcome. The negative lymph-node group had a 5-year survival rate of 50.2%.
Conclusion: Transhiatal esophagectomy can be safely used in patients with malnutrition degree that allows the procedure, in those with associated respiratory disorders and in the elderly. It provides considerable long-term survival, especially in the absence of metastases to local lymph nodes. The wider use of neoadjuvant therapy has the potential to further increase long-term survival.
Racional:: O sul do Brasil tem uma das maiores incidências de carcinoma epidermoide do esôfago no mundo. A esofagectomia transtorácica permite linfadenectomia abdominal e torácica mais completa do que a transhiatal. No entanto, esta está associado à menor morbidade.
Objetivo:: Analisar os desfechos e fatores prognósticos do câncer epidermoide do esôfago que foram tratados com procedimento transhiatal.
Métodos:: Foram incluídos todos os pacientes selecionados para abordagem transhiatal como tratamento potencialmente curativo correlacionando sobrevida geral, tempo operatório, análise de linfonodos e uso de terapia neoadjuvante.
Resultados:: Foram avaliados 96 pacientes. A sobrevida geral em cinco anos foi de 41,2%. A análise multivariada mostrou que o tempo operatório e a presença de linfonodos positivos foram associados a pior resultado, enquanto a terapia neoadjuvante contribuiu para melhor resultado. O grupo de linfonodos negativos teve taxa de sobrevivência em cinco anos de 50,2%.
Conclusão:: A esofagectomia transhiatal pode ser empregada com segurança em pacientes que apresentem desnutrição com grau que permita o procedimento, nos com distúrbios respiratórios associados e nos idosos. Proporciona sobrevida em longo prazo considerável, especialmente na ausência de metástases para linfonodos locais. O uso mais amplo da terapia neoadjuvante tem o potencial de aumentar ainda mais a sobrevida em longo prazo.
Conflict of interest statement
Figures
Similar articles
-
Radical transhiatal esophagectomy with two-field lymphadenectomy and endodissection for distal esophageal adenocarcinoma.World J Surg. 1997 Oct;21(8):822-31. doi: 10.1007/pl00024609. World J Surg. 1997. PMID: 9327673
-
An audit of surgical outcomes of esophageal squamous cell carcinoma.Eur J Cardiothorac Surg. 2007 Mar;31(3):536-44. doi: 10.1016/j.ejcts.2006.12.002. Epub 2007 Jan 11. Eur J Cardiothorac Surg. 2007. PMID: 17222561
-
Perioperative outcomes of single-port mediastinoscope-assisted transhiatal esophagectomy for thoracic esophageal cancer.Dis Esophagus. 2017 Oct 1;30(10):1-8. doi: 10.1093/dote/dox047. Dis Esophagus. 2017. PMID: 28859387
-
Transhiatal esophagectomy.Surg Clin North Am. 2005 Jun;85(3):593-610. doi: 10.1016/j.suc.2005.01.009. Surg Clin North Am. 2005. PMID: 15927654 Review.
-
The Value of Lymphadenectomy Post-Neoadjuvant Therapy in Carcinoma Esophagus: a Review.Indian J Surg Oncol. 2020 Sep;11(3):538-548. doi: 10.1007/s13193-020-01156-w. Epub 2020 Aug 3. Indian J Surg Oncol. 2020. PMID: 33013140 Free PMC article. Review.
Cited by
-
The impact of geriatric nutritional risk index on esophageal squamous cell carcinoma patients with neoadjuvant therapy followed by esophagectomy.Front Nutr. 2022 Oct 20;9:983038. doi: 10.3389/fnut.2022.983038. eCollection 2022. Front Nutr. 2022. PMID: 36337651 Free PMC article.
-
CERVICAL ESOPHAGOGASTRIC ANASTOMOSIS FISTULA FOLLOWING ESOPHAGECTOMY: A PROBLEM WITH NO SOLUTION?Arq Bras Cir Dig. 2022 Jan 5;34(3):e1619. doi: 10.1590/0102-672020210002e1619. eCollection 2022. Arq Bras Cir Dig. 2022. PMID: 35019131 Free PMC article. No abstract available.
-
THYLENETETRAHYDROFOLATE REDUCTASE GENE POLYMORPHISMS AND SUSCEPTIBILITY TO ESOPHAGEAL CANCER: A CASE-CONTROL STUDY.Arq Bras Cir Dig. 2022 Sep 9;35:e1684. doi: 10.1590/0102-672020220002e1684. eCollection 2022. Arq Bras Cir Dig. 2022. PMID: 36102491 Free PMC article.
-
CHARACTERIZATION OF THE PSYCHOLOGICAL TYPOLOGY IN ESOPHAGEAL CANCER PATIENTS.Arq Bras Cir Dig. 2023 Jan 9;35:e1715. doi: 10.1590/0102-672020220002e1715. eCollection 2023. Arq Bras Cir Dig. 2023. PMID: 36629692 Free PMC article.
-
THE ESOPHAGEAL, GASTRIC, AND COLORECTAL TUMORS AND THE ESOPHAGOGASTRODUODENOSCOPIES AND COLONOSCOPIES BY THE BRAZILIAN UNIFIED HEALTH SYSTEM: WHAT IS THE IMPORTANCE?Arq Bras Cir Dig. 2022 Jun 24;35:e1661. doi: 10.1590/0102-672020210002e1661. eCollection 2022. Arq Bras Cir Dig. 2022. PMID: 35766606 Free PMC article.
References
-
- Blencowe NS, Strong S, McNair AGK, Brookes ST, Crosby T, Griffin SM. Reporting of short-term clinical outcomes after esophagectomy a systematic review. Ann Surg. 2012;255(4):658–666. - PubMed
-
- Bogoevski D, Bockhorn M, Koenig A, Reeh M, von Loga K, Sauter G. How radical should surgery be for early esophageal cancer. World J Surg. 2011;35(6):1311–1320. - PubMed
-
- Boshier PR, Anderson O, Hanna GB. Transthoracic versus transhiatal esophagectomy for the treatment of esophagogastric cancer a meta-analysis. Ann Surg. 2011;254(6):894–906. - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Medical

