Change in Kidney Function and 2-Year Mortality After Transcatheter Aortic Valve Replacement
- PMID: 33769507
- PMCID: PMC7998079
- DOI: 10.1001/jamanetworkopen.2021.3296
Change in Kidney Function and 2-Year Mortality After Transcatheter Aortic Valve Replacement
Abstract
Importance: Chronic kidney disease (CKD) is prevalent in the population of patients undergoing transcatheter aortic valve replacement (TAVR). Data on the association of TAVR with kidney function are scarce, as are data on the relationship between changes in kidney function after TAVR and mortality.
Objective: To describe the changes in kidney function (both periprocedural and at steady state) after TAVR and to explore the association of TAVR with midterm mortality.
Design, setting, and participants: This single-center, retrospective cohort study was conducted at a public, tertiary academic medical center, which serves as a regional referral center for valvular heart interventions. Consecutive cases of patients undergoing TAVR from November 5, 2008, to December 31, 2019, were included in the study, with available baseline and post-TAVR data on kidney function.
Exposures: Steady state (1 month) change in kidney function after TAVR. Significant improvement or deterioration in renal function was defined as a greater than or equal to 10% change in estimated glomerular filtration rate (eGFR).
Main outcomes and measures: Overall mortality at 2-year follow-up.
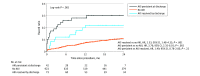
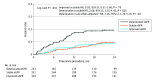
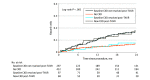
Results: A total of 894 patients (mean [SD] age, 82.2 [7.1] years; 452 women ([51.2%]) were evaluated. A total of 362 patients (40.5%) were treated from 2017 to 2019, 348 patients (38.9%) were treated from 2013 to 2016, and 184 patients (20.5%) were treated from 2008 and 2012. Patients had a mean (SD) Society of Thoracic Surgeons (STS) score of 5.2% (4.0%) and a mean (SD) eGFR of 65.1 (23.1) mL/min/1.73 m2. Acute kidney injury occurred in 115 (11.1%) patients by 48 hours, of whom 73 (63.5%) resolved by discharge. One month after TAVR, eGFR improved by at least 10% in 329 patients (36.8%) and deteriorated by at least 10% in 233 patients (26.1%). Overall, CKD stage remained stable or improved in 720 patients (80.6%), and only 5 patients (0.97%) progressed to stage 5 CKD 1 month after TAVR. A deterioration of 10% or greater in eGFR 1 month after TAVR was associated with a hazard ratio of 2.16 (95% CI, 1.24-5.24; P = .04) at 2-year mortality. Patients who showed CKD status resolution (eGFR improvement to >60 mL/min/1.73 m2 after TAVR) had a similar 2-year mortality to those with baseline eGFR greater than 60 mL/min/1.73 m2 and vice versa. Factors associated with steady state CKD status resolution after TAVR included lower STS score, higher left ventricular ejection fraction, higher baseline eGFR, no acute kidney injury at discharge from the TAVR admission, and lower contrast-eGFR ratio.
Conclusions and relevance: In this cohort study, kidney outcomes after TAVR were reassuring; greater than 80% of patients showed stable or improved kidney function 1 month after the procedure. Improvement in kidney function was associated with a lower 2-year mortality, whereas deterioration in kidney function was associated with increased mortality. Our data suggest that cardiorenal syndrome was a possible cause of CKD in patients in need of TAVR and that there was potential for improvement in both renal and cardiac function after this procedure.
Conflict of interest statement
Figures
Comment in
-
Can Transcatheter Aortic Valve Replacement Cure Cardiorenal Syndrome?JAMA Netw Open. 2021 Mar 1;4(3):e213753. doi: 10.1001/jamanetworkopen.2021.3753. JAMA Netw Open. 2021. PMID: 33769503 No abstract available.
References
-
- Gargiulo G, Capodanno D, Sannino A, et al. Moderate and severe preoperative chronic kidney disease worsen clinical outcomes after transcatheter aortic valve implantation: meta-analysis of 4992 patients. Circ Cardiovasc Interv. 2015;8(2):e002220. doi: 10.1161/CIRCINTERVENTIONS.114.002220 - DOI - PubMed
-
- Allende R, Webb JG, Munoz-Garcia AJ, et al. Advanced chronic kidney disease in patients undergoing transcatheter aortic valve implantation: insights on clinical outcomes and prognostic markers from a large cohort of patients. Eur Heart J. 2014;35(38):2685-2696. doi: 10.1093/eurheartj/ehu175 - DOI - PubMed
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous

