Shared decision making and patients satisfaction with strabismus care-a pilot study
- PMID: 33771137
- PMCID: PMC7995717
- DOI: 10.1186/s12911-021-01469-y
Shared decision making and patients satisfaction with strabismus care-a pilot study
Abstract
Background: Strabismus is a complex disease that has various treatment approaches each with its own advantages and drawbacks. In this context, shared decisions making (SDM) is a communication process with the provider sharing all the relevant treatment alternatives, all the benefits, and risks of each procedure, while the patient shares all the preferences and values regarding his/her choices. In that way, SDM is a bidirectional process that goes beyond the typical informed consent. Therefore, it is known a little of the extent to which SDM influences the satisfaction with the treatment outcome along with strabismus patients. To study this correlation, an SDM-Q-9 questionnaire was provided within surgical consultations where treatment decisions were made; the SDM-Q-9 aims to assess the relationship between the post-operative patient's satisfaction and their SMD score.
Methods: The study is considered a prospective observational pilot study. Eligible patients were adult patients diagnosed with strabismus, who had multiple treatment options, were given at the right of choice without being driven into a physician's preference. Ninety-three strabismus patients were asked to fill out the SDM-Q-9 questionnaire related to their perception of SDM during the entire period of strabismus treatment. After the treatment, patients were asked to rate their satisfaction level with the surgical outcome as excellent, good, fair, and poor. Descriptive statistics and the linear regression statistical tests (Spearman, Mann Whitney U, and Kriskal-Wallis) were used as analysis tools.
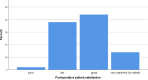
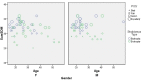
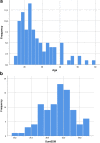
Results: The average age of the participants was 24, where 50.6% were women. The mean SDM-Q-9 score among patients was 32 (IQR = 3). The postoperative patient satisfaction was rated as being excellent by 16 (17.2%) patients, good by 38 (40.9%), fair by 32 (34.4%), and poor by 7 patients (7.5%). Data analysis by linear regression statistical tests showed a positive correlation between the SDM-Q-9 score and the patient satisfaction related to the surgery outcome (B = 0.005, p < 0.001). Criteria in assessing patients' satisfaction were age, gender, and strabismus type. A positive correlation between SDM and real satisfaction (r = 0.834, p < 0.01) was found with age, and no significant relationship was found while taking into consideration the responder's gender and the strabismus type.
Conclusions: Assessing patient satisfaction after choosing a treatment for strabismus method helped us evaluate the gaps in constructive dialogue that would lead to a positive outcome for both patient and clinician. The correlation between the SDM process and the patients' satisfaction with surgery outcome, adjusted by age, has been established. These findings can serve as a springboard to further communicative improvements related to the SDM process and between patients and physicians, thereby consequently leading to patients' satisfaction raise in strabismus care. The study underlines the importance of further analysis and validation of on-ground interactions among the adolescent and adult patients and the clinicians across the strabismus management trajectory. A multicentral study and its validation will follow.
Keywords: Adult strabismus; Patient satisfaction; Patient-centered care; Physician–patient communication; Shared decision making.
Conflict of interest statement
The authors declare that they have no competing interests.
Figures

References
-
- Stager DR, Sr, Stager DR, Jr, Beauchamp GR. Treament option for adult strabismus. Therapy. 2007;4(3):311–317. doi: 10.2217/14750708.4.3.307. - DOI
-
- Sackett DL, Rosenberg WM, Gray JA, Haynes RB, Richardson WS. Evidence based medicine: what it is and what it isn't. 1996. Clin Orthop Relat Res. 2007;455:3–5. - PubMed
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources

