Treatment of anemia in difficult-to-manage patients with chronic kidney disease
- PMID: 33777493
- PMCID: PMC7983023
- DOI: 10.1016/j.kisu.2020.12.006
Treatment of anemia in difficult-to-manage patients with chronic kidney disease
Abstract
The management of anemia of chronic kidney disease (CKD) is often challenging. In particular, for patients with underlying inflammation, comorbid type 2 diabetes or cancer, those hospitalized, and recipients of a kidney transplant, the management of anemia may be suboptimal. Responsiveness to iron and/or erythropoiesis-stimulating agents, the mainstay of current therapy, may be reduced and the risk of adverse reactions to treatment is increased in these difficult-to-manage patients with anemia of CKD. This review discusses the unique patient and disease characteristics leading to complications and suboptimal treatment response. New treatment options in clinical development, such as hypoxia-inducible factor-prolyl hydroxylase (HIF-PH) inhibitors, may be particularly useful for difficult-to-treat patients. In clinical studies, HIF-PH inhibitors provided increased hemoglobin levels and improved iron utilization in anemic patients with non-dialysis-dependent and dialysis-dependent CKD, and preliminary data suggest that HIF-PH inhibitors may be equally effective in patients with or without underlying inflammation. The availability of new treatment options, including HIF-PH inhibitors, may improve treatment outcomes in difficult-to-manage patients with anemia of CKD.
Keywords: anemia; cancer; chronic kidney disease; hospitalization; hypoxia-inducible factor-prolyl hydroxylase inhibitor; inflammation; kidney transplantation; type 2 diabetes.
© 2021 International Society of Nephrology. Published by Elsevier Inc. All rights reserved.
Figures
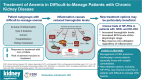


References
-
- Kidney Disease Improving Global Outcomes KDIGO clinical practice guideline for anemia in chronic kidney disease. Kidney Int Suppl. 2012;2:283–287.
-
- Faich G., Strobos J. Sodium ferric gluconate complex in sucrose: safer intravenous iron therapy than iron dextrans. Am J Kidney Dis. 1999;33:464–470. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources

