Cause-Specific Mortality Among Survivors From T1N0M0 Renal Cell Carcinoma: A Registry-Based Cohort Study
- PMID: 33777747
- PMCID: PMC7988093
- DOI: 10.3389/fonc.2021.604724
Cause-Specific Mortality Among Survivors From T1N0M0 Renal Cell Carcinoma: A Registry-Based Cohort Study
Abstract
Objective: More T1N0M0 renal cell carcinoma (RCC) is detected and the prognosis has improved, but, the current focus on non-RCC-related mortality is superficial. We investigated cause-specific mortality and its temporal patterns after an RCC diagnosis.
Methods: In the Surveillance, Epidemiology, and End Results-18 database, patients with T1N0M0 RCC treated with partial nephrectomy (PN) or radical nephrectomy (RN) during 2000-15 were identified. Standardized mortality ratios (SMRs) for cause of death were calculated. Risk predictors for each cause-specific mortality were investigated using the Fine and Gray sub-distribution model.
Results: In all, 68,612 eligible patients were pooled. A total of 14,047 (20.5%) patients had died (cardiovascular disease [CVD], 28.3%; other non-cancer-related diseases, 20.3%; RCC, 18.7%; other cancer types, 16.3%; non-disease events, 16.1%) during follow-up. Heart disease, diabetes mellitus, and cerebrovascular disease were the primary causes of non-RCC-related mortality within 1 year after the diagnosis. The greatest proportion of death (39.0%) occurred within 1-5 years after the diagnosis, mostly due to RCC itself, followed by heart disease. However, >5 years after the diagnosis, heart disease became the leading cause of death. Compared with the general US population, a 21% (SMR, 1.21; 95%CI 1.19-1.23) increased risk of all-mortality was observed; RCC patients had a higher risk of heart disease-related death within 5-10 years (SMR, 1.10; 95%CI 1.04-1.17) and >10 years (1.12; 1.02-1.22) after the diagnosis. Older age and RN increased the death risk of CVD and RCC-specific mortality. Although a larger tumor diameter increased the risk of RCC-specific death, this was not a significant predictor for CVD. Moreover, for T1N0M0 RCC tumors of diameter >4 cm, there was no significant difference in CVD incidence for RN vs. PN.
Conclusions: RCC-specific mortality is a common challenge for the prognosis. Importantly, a large proportion and higher SMRs of other non-RCC-related diseases (especially CVD) should not be disregarded for the better holistic management of survivors of local RCC. Targeted prevention strategies for non-RCC-related death could lead to significant reductions in mortality for RCC survivors.
Keywords: competing mortality; long-term survival; prognosis; renal cell carcinoma; standardized mortality ratio.
Copyright © 2021 Wang, Wang, Zhu, Liu, Li and Zeng.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
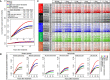



References
LinkOut - more resources
Full Text Sources
Other Literature Sources

