Short-term effects of ambient air pollution and outdoor temperature on biomarkers of myocardial damage, inflammation and oxidative stress in healthy adults
- PMID: 33778346
- PMCID: PMC7939428
- DOI: 10.1097/EE9.0000000000000078
Short-term effects of ambient air pollution and outdoor temperature on biomarkers of myocardial damage, inflammation and oxidative stress in healthy adults
Abstract
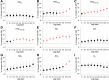
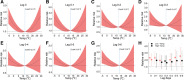
The mechanisms whereby ambient air pollution and temperature changes promote cardiac events remain incompletely described. Seventy-three nonsmoking healthy adults (mean age 23.3, SD 5.4 years) were followed with up to four repeated visits across 15 months in Beijing in 2014-2016. Biomarkers relevant to myocardial damage (high-sensitivity cardiac troponin I [hs-cTnI]), inflammation (growth differentiation factor-15 [GDF-15]), and oxidative stress (8-hydroxy-2'-deoxyguanosine [8-OHdG]) were measured at each visit, while ambient air pollution and temperature were monitored throughout the study. Linear mixed-effects models coupled with distributed lag nonlinear models were used to assess the impacts of each exposure measure on study outcomes. During follow-up, average daily concentrations of fine particulate matter and outdoor temperature were 62.9 µg/m3 (8.1-331.0 µg/m3) and 10.1 °C (-6.5°C to 29.5°C). Serum hs-cTnI levels were detectable in 18.2% of blood samples, with 27.4% of individuals having ≥1 detectable values. Higher levels of ambient particulates and gaseous pollutants (per interquartile range) up to 14 days before clinical visits were associated with significant alterations in hs-cTnI levels of 22.9% (95% CI, 6.4, 39.4) to 154.7% (95% CI, 94.4, 215.1). These changes were accompanied by elevations of circulating GDF-15 and urinary 8-OHdG levels. Both low (5th percentile, -2.5 °C) and high (95th percentile, 24.8°C) outdoor temperatures, with breakpoint at ~13.0°C as the reference level, were also associated with elevations of hs-cTnI levels. Short-term exposure to ambient air pollution and temperature was associated with cardiac troponin, a biomarker of myocardial damage, along with increased inflammation and oxidative stress responses. These findings extend our understanding of the biological mechanisms linking pervasive environmental exposure to adverse cardiac events.
Keywords: Air pollution; Cardiac troponin; Myocardial damage; Temperature.
Copyright © 2019 The Authors. Published by Wolters Kluwer Health, Inc. on behalf of Environmental Epidemiology. All rights reserved.
Conflict of interest statement
The author/authors declares/declare that they have no conflicts of interest with regard to the content of this report. The results reported herein correspond to specific aims of grant 81773381 to investigator Wei Huang from National Natural Science Foundation of China. This work was (also) supported by grants from National Natural Science Foundation of China (81470025) and Peking University Health Science Center-University of Michigan Health System Joint Institute for Clinical and Translational Research, and Peking University Infrastructure Fund for Interdisciplinary Studies (2013-3-02).
Figures



Similar articles
-
Ambient Air Pollution Is Associated With HDL (High-Density Lipoprotein) Dysfunction in Healthy Adults.Arterioscler Thromb Vasc Biol. 2019 Mar;39(3):513-522. doi: 10.1161/ATVBAHA.118.311749. Arterioscler Thromb Vasc Biol. 2019. PMID: 30700134
-
Extreme Levels of Air Pollution Associated With Changes in Biomarkers of Atherosclerotic Plaque Vulnerability and Thrombogenicity in Healthy Adults.Circ Res. 2019 Mar;124(5):e30-e43. doi: 10.1161/CIRCRESAHA.118.313948. Circ Res. 2019. PMID: 30661461
-
Part 2. Association of daily mortality with ambient air pollution, and effect modification by extremely high temperature in Wuhan, China.Res Rep Health Eff Inst. 2010 Nov;(154):91-217. Res Rep Health Eff Inst. 2010. PMID: 21446212
-
[Breathing: Ambient Air Pollution and Health - Part II].Pneumologie. 2019 Jun;73(6):347-373. doi: 10.1055/a-0895-6494. Epub 2019 Jun 11. Pneumologie. 2019. PMID: 31185518 Review. German.
-
Ambient particulate air pollution and circulating C-reactive protein level: A systematic review and meta-analysis.Int J Hyg Environ Health. 2019 Jun;222(5):756-764. doi: 10.1016/j.ijheh.2019.05.005. Epub 2019 May 16. Int J Hyg Environ Health. 2019. PMID: 31103472
Cited by
-
Associations between short-term exposure to PM2.5 and cardiomyocyte injury in myocardial infarction survivors in North Carolina.Open Heart. 2022 Jun;9(1):e001891. doi: 10.1136/openhrt-2021-001891. Open Heart. 2022. PMID: 35750420 Free PMC article.
-
Association of Ambient Air Pollution and Temperature Exposure with Placental Abruption: A Nested Case-Control Study Based on Live Birth Registrations.Environ Health Perspect. 2025 Apr;133(3-4):47013. doi: 10.1289/EHP14714. Epub 2025 Apr 29. Environ Health Perspect. 2025. PMID: 40138323 Free PMC article.
-
The associations between short-term exposure to ambient particulate matter and hospitalizations for osteoporotic fracture in Hangzhou: a time-stratified case-crossover study.Arch Osteoporos. 2022 Dec 5;18(1):4. doi: 10.1007/s11657-022-01192-9. Arch Osteoporos. 2022. PMID: 36469172
-
Maternal preconceptional and prenatal exposure to El Niño Southern Oscillation levels and child mortality: a multi-country study.Nat Commun. 2024 Jul 17;15(1):6034. doi: 10.1038/s41467-024-50467-x. Nat Commun. 2024. PMID: 39019882 Free PMC article.
-
Intermediate- and long-term associations between air pollution and ambient temperature and glycated hemoglobin levels in women of child bearing age.Environ Int. 2022 Jul;165:107298. doi: 10.1016/j.envint.2022.107298. Epub 2022 May 14. Environ Int. 2022. PMID: 35597113 Free PMC article.
References
-
- Claeys MJ, Rajagopalan S, Nawrot TS, Brook RD. Climate and environmental triggers of acute myocardial infarction. Eur Heart J 201738955–960 - PubMed
-
- Rajagopalan S, Al-Kindi SG, Brook RD. Air pollution and cardiovascular disease: JACC state-of-the-art review. J Am Coll Cardiol 2018722054–2070 - PubMed
LinkOut - more resources
Full Text Sources
Research Materials
