On Structure-Function Relationships in the Female Human Urethra: A Finite Element Model Approach
- PMID: 33782810
- PMCID: PMC8376757
- DOI: 10.1007/s10439-021-02765-4
On Structure-Function Relationships in the Female Human Urethra: A Finite Element Model Approach
Abstract
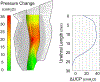
Remarkably little is known about urethral striated and smooth muscle and vascular plexus contributions to maintaining continence or initiating micturition. We therefore developed a 3-D, multiphysics, finite element model, based on sequential MR images from a 23-year-old nulliparous heathy woman, to examine the effect of contracting one or more individual muscle layers on the urethral closure pressure (UCP). The lofted urethra turned out to be both curved and asymmetric. The model results led us to reject the current hypothesis that the striated and smooth muscles contribute equally to UCP. While a simulated contraction of the outer (circular) striated muscle increased closure pressure, a similar contraction of the large inner longitudinal smooth muscle both reduced closure pressure and shortened urethral length, suggesting a role in initiating micturition. When age-related atrophy of the posterior striated muscle was simulated, a reduced and asymmetric UCP distribution developed in the transverse plane. Lastly, a simple 2D axisymmetric model of the vascular plexus and lumen suggests arteriovenous pressure plays and important role in helping to maintain luminal closure in the proximal urethra and thereby functional urethral length. More work is needed to examine interindividual differences and validate such models in vivo.
Keywords: Arteriovenous anastomoses; Finite element model; Smooth muscle; Striated muscle; Urethra; Urethral closure pressure; Vascular plexus.
© 2021. Biomedical Engineering Society.
Conflict of interest statement
Conflict of Interest
Authors declare that they have no conflict of interest.
Figures

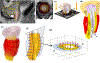
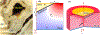
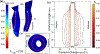

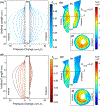

References
-
- Abé H, Hayashi K, and Sato M. Data Book on Mechanical Properties of Living Cells, Tissues, and Organs. Tokyo: Springer Japan, 1996, 37–39 pp.
-
- Backman KA URODYNAMICS-THE HYDRODYNAMICS OF MICTURITION IN NORMAL FEMALE SUBJECTS. Acta Neurol. Scand 42:79–85, 2009. - PubMed
-
- Brandão S, Parente M, Silva E, Da Roza T, Mascarenhas T, Leitão J, Cunha J, Natal Jorge R, and Nunes RG. Pubovisceralis Muscle Fiber Architecture Determination: Comparison Between Biomechanical Modeling and Diffusion Tensor Imaging. Ann. Biomed. Eng 45:1255–1265, 2017. - PubMed
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

