Diabetes Insipidus: Pathogenesis, Diagnosis, and Clinical Management
- PMID: 33786230
- PMCID: PMC7996474
- DOI: 10.7759/cureus.13523
Diabetes Insipidus: Pathogenesis, Diagnosis, and Clinical Management
Abstract
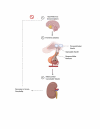
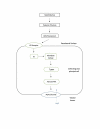
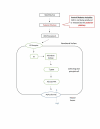
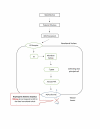
Diabetes insipidus (DI) is an endocrine condition involving the posterior pituitary peptide hormone, antidiuretic hormone (ADH). ADH exerts its effects on the distal convoluted tubule and collecting duct of the nephron by upregulating aquaporin-2 channels (AQP2) on the cellular apical membrane surface. DI is marked by expelling excessive quantities of highly dilute urine, extreme thirst, and craving for cold water. The two main classifications of DI are central diabetes insipidus (CDI), characterized by a deficiency of the posterior pituitary gland to release ADH, and nephrogenic diabetes insipidus (NDI), characterized by the terminal distal convoluted tubule and collecting duct resistance to ADH. The two less common classifications include dipsogenic DI, characterized by excessive thirst due to a low osmotic threshold, and gestational DI, characterized by increased concentration of placental vasopressinase during pregnancy. Treatment of DI is dependent on the disease classification, but severe complications may arise if not tended to appropriately. The most important step in symptom management is maintaining fluid intake ahead of fluid loss with emphasis placed on preserving the quality of life. The most common treatment of CDI and gestational DI is the administration of synthetic ADH, desmopressin (DDAVP). Nephrogenic treatment, although more challenging, requires discontinuation of medications as well as maintaining a renal-friendly diet to prevent hypernatremia. Treatment of dipsogenic DI is mainly focused on behavioral therapy aimed at regulating water intake and/or administration of antipsychotic pharmaceutical therapy. Central and nephrogenic subtypes of DI share a paradoxical treatment in thiazide diuretics.
Keywords: antidiuretic hormone; central diabetes insipidus; diabetes insipidus; dipsogenic diabetes insipidus; gestational diabetes insipidus; nephrogenic diabetes insipidus; vasopressin.
Copyright © 2021, Mutter et al.
Conflict of interest statement
The authors have declared that no competing interests exist.
Figures
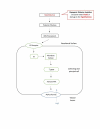
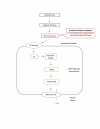
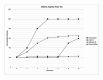
References
-
- Diabetes insipidus. Christ-Crain M, Bichet DG, Fenske WK, Goldman MB, Rittig S, Verbalis JG, Verkman AS. Nat Rev Primers. 2019;5:54. - PubMed
-
- Antidiuretic hormone: normal and disordered function. Robertson GL. Endocrinology. 2001;30:671–694. - PubMed
-
- Hickey J. The Clinical Practice of Neurological and Neurosurgical Nursing. Philadelphia, PA: Lippincott Williams & Wilkins; Fluid and metabolic disorders in neuroscience patients; pp. 195–205.
-
- Neuroimaging of central diabetes insipidus—when, how and findings. Adams NC, Farrell TP, O’Shea A. Neuroradiology. 2018;60:995–1012. - PubMed
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources
