Deficiency of Biogenic Amines Modulates the Activity of Hypoglossal Nerve in the Reserpine Model of Parkinson's Disease
- PMID: 33801475
- PMCID: PMC8001069
- DOI: 10.3390/cells10030531
Deficiency of Biogenic Amines Modulates the Activity of Hypoglossal Nerve in the Reserpine Model of Parkinson's Disease
Abstract
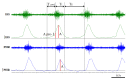
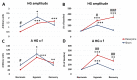
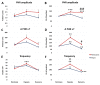
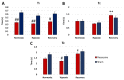
The underlying cause of respiratory impairments appearing in Parkinson's disease (PD) is still far from being elucidated. To better understand the pathogenesis of respiratory disorders appearing in PD, we studied hypoglossal (HG) and phrenic (PHR) motoneuron dysfunction in a rat model evoked with reserpine administration. After reserpine, a decrease in the baseline amplitude and minute HG activity was noted, and no depressive phase of the hypoxic ventilatory response was observed. The pre-inspiratory time of HG activity along with the ratio of pre-inspiratory time to total respiratory cycle time and the ratio of pre-inspiratory to inspiratory amplitude were significantly reduced during normoxia, hypoxia, and recovery compared to sham rats. We suggest that the massive depletion of not only dopamine, but above all noradrenaline and serotonin in the brainstem observed in our study, has an impact on the pre-inspiratory activity of the HG. The shortening of the pre-inspiratory activity of the HG in the reserpine model may indicate a serious problem with maintaining the correct diameter of the upper airways in the preparation phase for inspiratory effort and explain the development of obstructive sleep apnea in some PD patients. Therapies involving the supplementation of amine depletion other than dopamine should be considered.
Keywords: Parkinson’s diseases; biogenic amines; hypoglossal nerve; hypoxia; phrenic nerve; reserpine model.
Conflict of interest statement
The authors declare no conflict of interest.
Figures

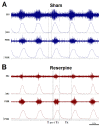
References
-
- da Silva Córneo E., de Bem Silveira G., Scussel R., Borges Correa M.E.A., da Silva Abel J., Luiz G.P., Feuser P.E., Silveira P.C.L., Machado-de-Ávila R.A. Effects of gold nanoparticles administration through behavioral and oxidative parameters in animal model of Parkinson’s disease. Colloids Surf. B Biointerfaces. 2020;196:111302. doi: 10.1016/j.colsurfb.2020.111302. - DOI - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

