Co-Opting Host Receptors for Targeted Delivery of Bioconjugates-From Drugs to Bugs
- PMID: 33803208
- PMCID: PMC7963163
- DOI: 10.3390/molecules26051479
Co-Opting Host Receptors for Targeted Delivery of Bioconjugates-From Drugs to Bugs
Abstract
Bioconjugation has allowed scientists to combine multiple functional elements into one biological or biochemical unit. This assembly can result in the production of constructs that are targeted to a specific site or cell type in order to enhance the response to, or activity of, the conjugated moiety. In the case of cancer treatments, selectively targeting chemotherapies to the cells of interest limit harmful side effects and enhance efficacy. Targeting through conjugation is also advantageous in delivering treatments to difficult-to-reach tissues, such as the brain or infections deep in the lung. Bacterial infections can be more selectively treated by conjugating antibiotics to microbe-specific entities; helping to avoid antibiotic resistance across commensal bacterial species. In the case of vaccine development, conjugation is used to enhance efficacy without compromising safety. In this work, we will review the previously mentioned areas in which bioconjugation has created new possibilities and advanced treatments.
Keywords: antibiotics; antibody–drug conjugates; bioconjugation; conjugated vaccines; drug delivery; nanoparticles; targeted vaccines; vaccines.
Conflict of interest statement
The authors declare no conflict of interest. The funders had no role in the writing of the manuscript.
Figures
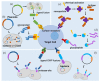
Similar articles
-
Bioconjugation in Drug Delivery: Practical Perspectives and Future Perceptions.Methods Mol Biol. 2019;2000:125-182. doi: 10.1007/978-1-4939-9516-5_11. Methods Mol Biol. 2019. PMID: 31148014 Review.
-
Controlled antibody/(bio-) conjugation of inorganic nanoparticles for targeted delivery.Adv Drug Deliv Rev. 2013 May;65(5):677-88. doi: 10.1016/j.addr.2012.12.003. Epub 2012 Dec 29. Adv Drug Deliv Rev. 2013. PMID: 23280372 Review.
-
In vivo targeted delivery of nanoparticles for theranosis.Acc Chem Res. 2011 Oct 18;44(10):1018-28. doi: 10.1021/ar2000138. Epub 2011 Aug 18. Acc Chem Res. 2011. PMID: 21851104 Review.
-
Antibody-conjugated nanoparticles for therapeutic applications.Curr Med Chem. 2012;19(19):3103-27. doi: 10.2174/092986712800784667. Curr Med Chem. 2012. PMID: 22612698 Review.
-
Towards the next generation of biomedicines by site-selective conjugation.Chem Soc Rev. 2016 Mar 21;45(6):1691-719. doi: 10.1039/c4cs00388h. Chem Soc Rev. 2016. PMID: 26796469 Review.
References
Publication types
MeSH terms
Substances
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

