How to Choose a Shunt for Patients with Normal Pressure Hydrocephalus: A Short Guide to Selecting the Best Shunt Assembly
- PMID: 33803977
- PMCID: PMC7999679
- DOI: 10.3390/jcm10061210
How to Choose a Shunt for Patients with Normal Pressure Hydrocephalus: A Short Guide to Selecting the Best Shunt Assembly
Abstract
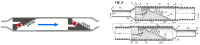
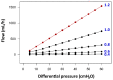
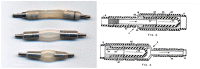
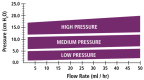
Most patients with hydrocephalus are still managed with the implantation of a cerebrospinal fluid (CSF) shunt in which the CSF flow is regulated by a differential-pressure valve (DPV). Our aim in this review is to discuss some basic concepts in fluid mechanics that are frequently ignored but that should be understood by neurosurgeons to enable them to choose the most adequate shunt for each patient. We will present data, some of which is not provided by manufacturers, which may help neurosurgeons in selecting the most appropriate shunt. To do so, we focused on the management of patients with idiopathic "normal-pressure hydrocephalus" (iNPH), as one of the most challenging scenarios, in which the combination of optimal technology, patient characteristics, and knowledge of fluid mechanics can significantly modify the surgical results. For a better understanding of the available hardware and its evolution over time, we will have a second look at the design of the first DPV and the reasons why additional devices were incorporated to control for shunt overdrainage and its related complications. We try to persuade the reader that a clear understanding of the physical concepts of the CSF and shunt dynamics is key to understand the pathophysiology of iNPH and to improve its treatment.
Keywords: antisiphon device; differential-pressure valves; fluid mechanics; hydrocephalus; normal-pressure hydrocephalus; shunt overdrainage.
Conflict of interest statement
The authors report no conflict of interest concerning the materials or methods used in this study or the findings and opinions specified in this paper.
Figures




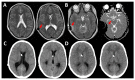
References
-
- Aschoff A. In-Depth View: Functional Characteristics of CSF Shunt Devices (Pros and Cons) In: Di Rocco C., Pang D., Rutka J.T., editors. Textbook of Pediatric Neurosurgery. Springer International Publishing; Cham, Switzerland: 2017. pp. 1–40. - DOI
-
- Furlanetti L.L., Ballestero M.F.M., De Oliveira R.S. Shunt Technology in Pediatric Neurosurgery: Current options and Scientific Evidence. Arch. Pediatric. Neurosurg. 2020;2:e342020. doi: 10.46900/apn.v2i2(May-August).34. - DOI
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources

