High Expression of Solute Carrier Family 2 Member 1 (SLC2A1) in Cancer Cells Is an Independent Unfavorable Prognostic Factor in Pediatric Malignant Peripheral Nerve Sheath Tumor
- PMID: 33810575
- PMCID: PMC8065586
- DOI: 10.3390/diagnostics11040598
High Expression of Solute Carrier Family 2 Member 1 (SLC2A1) in Cancer Cells Is an Independent Unfavorable Prognostic Factor in Pediatric Malignant Peripheral Nerve Sheath Tumor
Abstract
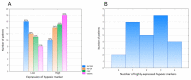
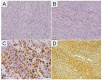
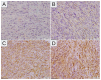
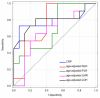
Malignant peripheral nerve sheath tumor (MPNST) in children is a rare mesenchymal malignancy developing predominantly in the setting of neurofibromatosis type 1. The prognosis in advanced MPNST is poor therefore new prognostic markers are highly needed for optimal therapeutic decisions. In many solid tumors, the bidirectional interactions between hypoxia and inflammation in the tumor microenvironment via functions of tumor-associated cells, like neutrophils, lymphocytes and macrophages, have been investigated recently. There is no data whether in MPNST hypoxic microenvironment may translate into systemic inflammation, which is a well-established factor for worse prognosis in cancer patients. Therefore, we investigated the prognostic significance of markers of tumor hypoxia and systemic inflammation in 26 pediatric malignant peripheral nerve sheath tumors (MPNST). Tumor tissue microarrays were stained for hypoxia-inducible factor-1α (HIF1A), solute carrier family 2 member 1 (SLC2A1, also known as glucose transporter 1 (GLUT1)), carbonic anhydrase 9 (CA9), and vascular endothelial growth factor A (VEGFA) and classified into low- or high-expression groups. Baseline complete blood counts and C-reactive protein (CRP) levels were collected for all cases. Neutrophil-to-lymphocyte ratio (NLR), platelet-to-lymphocyte ratio (PLR), and lymphocyte-to-monocyte ratio (LMR) were calculated from age-adjusted complete blood count parameters. Both 10-year RFS and OS were significantly lower in patients with high NLR values (17% vs. 75%, p = 0.009, q = 0.018; and 31% vs. 100%, p = 0.0077, q = 0.014; respectively). Ten-year-OS was significantly lower in patients with high expression of SLC2A1 (20.00% vs. 94%, p < 0.001, log-rank), high expression of HIF1A (23% vs. 79%, p = 0.016, log-rank), and CRP higher than 31 mg/L (11% vs. 82%, p = 0.003, q = 0.009). Cox's proportional hazard regression analysis revealed that high expression of SLC2A1 (HR = 3.31, 95% CI = 1.08-10.09, p = 0.036) and VEGFA (HR = 4.40, 95% CI = 0.95-20.34, p = 0.058) were the independent factors predicting relapse, whereas high SLC2A1 was identified as the independent risk factor for death (HR = 12.20, 95% CI = 2.55-58.33, p = 0.002). Patients with high expression of hypoxic markers and low or high NLR/CRP values had the highest events rate, patients with low hypoxic markers and high NLR/CRP had intermediate events rate, while patients with low hypoxic markers and low NLR/CRP had the lowest events rate. SLC2A1 and VEGFA are promising novel prognostic factors in pediatric MPNST. Correlations between hypoxic and systemic inflammatory markers suggest the interplay between local tumor hypoxia and systemic inflammation.
Keywords: carbonic anhydrase 9; hypoxia-inducible factor-1α; lymphocyte-to-monocyte ratio; malignant peripheral nerve sheath tumor; markers of systemic inflammation; markers of tumor hypoxia; neutrophil-to-lymphocyte ratio; platelet-to-lymphocyte ratio; solute carrier family 2 member 1; vascular endothelial growth factor.
Conflict of interest statement
The authors declare no conflict of interest.
Figures







Similar articles
-
[Relationship between preoperative inflammatory indexes and prognosis of patients with rectal cancer and establishment of prognostic nomogram prediction model].Zhonghua Zhong Liu Za Zhi. 2022 May 23;44(5):402-409. doi: 10.3760/cma.j.cn112152-20200630-00612. Zhonghua Zhong Liu Za Zhi. 2022. PMID: 35615796 Chinese.
-
Glucose Transporter 1 (SLC2A1) and Vascular Endothelial Growth Factor A (VEGFA) Predict Survival After Resection of Colorectal Cancer Liver Metastasis.Ann Surg. 2016 Jan;263(1):138-45. doi: 10.1097/SLA.0000000000001109. Ann Surg. 2016. PMID: 25563886
-
Regulation of pH by Carbonic Anhydrase 9 Mediates Survival of Pancreatic Cancer Cells With Activated KRAS in Response to Hypoxia.Gastroenterology. 2019 Sep;157(3):823-837. doi: 10.1053/j.gastro.2019.05.004. Epub 2019 May 9. Gastroenterology. 2019. PMID: 31078621
-
Prognostic role of elevated preoperative systemic inflammatory markers in localized soft tissue sarcoma.Cancer Biomark. 2016;16(3):333-42. doi: 10.3233/CBM-160571. Cancer Biomark. 2016. PMID: 26835589 Review.
-
Systemic Inflammatory Markers for Predicting Overall Survival in Patients with Osteosarcoma: A Systematic Review and Meta-Analysis.Mediators Inflamm. 2021 Oct 21;2021:3456629. doi: 10.1155/2021/3456629. eCollection 2021. Mediators Inflamm. 2021. PMID: 34720749 Free PMC article.
Cited by
-
Identification of a m6A-related ferroptosis signature as a potential predictive biomarker for lung adenocarcinoma.BMC Pulm Med. 2023 Apr 18;23(1):128. doi: 10.1186/s12890-023-02410-x. BMC Pulm Med. 2023. PMID: 37072786 Free PMC article.
-
Transcriptional Responses of Different Brain Cell Types to Oxygen Decline.Brain Sci. 2024 Mar 30;14(4):341. doi: 10.3390/brainsci14040341. Brain Sci. 2024. PMID: 38671993 Free PMC article.
-
The Role of ER Stress-Related Phenomena in the Biology of Malignant Peripheral Nerve Sheath Tumors.Int J Mol Sci. 2021 Aug 30;22(17):9405. doi: 10.3390/ijms22179405. Int J Mol Sci. 2021. PMID: 34502310 Free PMC article. Review.
-
Specifically Targeted Transport of Plasma Membrane Transporters: From Potential Mechanisms for Regulating Cell Health or Disease to Applications.Membranes (Basel). 2021 Sep 27;11(10):736. doi: 10.3390/membranes11100736. Membranes (Basel). 2021. PMID: 34677502 Free PMC article. Review.
-
The hypoxia-associated genes in immune infiltration and treatment options of lung adenocarcinoma.PeerJ. 2023 Aug 7;11:e15621. doi: 10.7717/peerj.15621. eCollection 2023. PeerJ. 2023. PMID: 37576511 Free PMC article.
References
-
- Noesel M.M., Orbach D., Brennan B., Kelsey A., Zanetti I., Salvo G.L., Gaze M.N., Craigie R.J., McHugh K., Francotte N., et al. Outcome and prognostic factors in pediatric malignant peripheral nerve sheath tumors: An analysis of the European Pediatric Soft Tissue Sarcoma Group (EpSSG) NRSTS-2005 prospective study. Pediatr. Blood Cancer. 2019;66:e27833. doi: 10.1002/pbc.27833. - DOI - PubMed
-
- Martin E., Coert J.H., Flucke U.E., Slooff W.B.M., van de Sande M.A.J., van Noesel M.M., Grünhagen D.J., Wijnen M.H.W.A., Verhoef C. Neurofibromatosis-associated malignant peripheral nerve sheath tumors in children have a worse prognosis: A nationwide cohort study. Pediatr. Blood Cancer. 2020;67:e28138. doi: 10.1002/pbc.28138. - DOI - PubMed
-
- Meister M.T., Scheer M., Hallmen E., Stegmaier S., Vokuhl C., Kalle T., Fuchs J., Münter M., Niggli F., Ladenstein R., et al. Malignant peripheral nerve sheath tumors in children, adolescents, and young adults: Treatment results of five Cooperative Weichteilsarkom Studiengruppe (CWS) trials and one registry. J. Surg. Oncol. 2020;122:1337–1347. doi: 10.1002/jso.26153. - DOI - PubMed
-
- Krawczyk M.A., Karpinsky G., Izycka-Swieszewska E., Gabrych A., Kunc M., Fatyga A., Garstka M., Styczewska M., Sokolewicz E.M., Szlagatys-Sidorkiewicz A., et al. Immunohistochemical assessment of cyclin D1 and p53 is associated with survival in childhood malignant peripheral nerve sheath tumor. Cancer Biomark. 2019;24:351–361. doi: 10.3233/CBM-181572. - DOI - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
Molecular Biology Databases
Research Materials
Miscellaneous

