Differences in obstetrical care and outcomes associated with the proportion of the obstetrician's shift completed
- PMID: 33812810
- PMCID: PMC8486887
- DOI: 10.1016/j.ajog.2021.03.033
Differences in obstetrical care and outcomes associated with the proportion of the obstetrician's shift completed
Abstract
Background: Understanding and improving obstetrical quality and safety is an important goal of professional societies, and many interventions such as checklists, safety bundles, educational interventions, or other culture changes have been implemented to improve the quality of care provided to obstetrical patients. Although many factors contribute to delivery decisions, a reduced workload has addressed how provider issues such as fatigue or behaviors surrounding impending shift changes may influence the delivery mode and outcomes.
Objective: The objective was to assess whether intrapartum obstetrical interventions and adverse outcomes differ based on the temporal proximity of the delivery to the attending's shift change.
Study design: This was a secondary analysis from a multicenter obstetrical cohort in which all patients with cephalic, singleton gestations who attempted vaginal birth were eligible for inclusion. The primary exposure used to quantify the relationship between the proximity of the provider to their shift change and a delivery intervention was the ratio of time from the most recent attending shift change to vaginal delivery or decision for cesarean delivery to the total length of the shift. Ratios were used to represent the proportion of time completed in the shift by normalizing for varying shift lengths. A sensitivity analysis restricted to patients who were delivered by physicians working 12-hour shifts was performed. Outcomes chosen included cesarean delivery, episiotomy, third- or fourth-degree perineal laceration, 5-minute Apgar score of <4, and neonatal intensive care unit admission. Chi-squared tests were used to evaluate outcomes based on the proportion of the attending's shift completed. Adjusted and unadjusted logistic models fitting a cubic spline (when indicated) were used to determine whether the frequency of outcomes throughout the shift occurred in a statistically significant, nonlinear pattern RESULTS: Of the 82,851 patients eligible for inclusion, 47,262 (57%) had ratio data available and constituted the analyzable sample. Deliveries were evenly distributed throughout shifts, with 50.6% taking place in the first half of shifts. There were no statistically significant differences in the frequency of cesarean delivery, episiotomy, third- or fourth-degree perineal lacerations, or 5-minute Apgar scores of <4 based on the proportion of the shift completed. The findings were unchanged when evaluated with a cubic spline in unadjusted and adjusted logistic models. Sensitivity analyses performed on the 22.2% of patients who were delivered by a physician completing a 12-hour shift showed similar findings. There was a small increase in the frequency of neonatal intensive care unit admissions with a greater proportion of the shift completed (adjusted P=.009), but the findings did not persist in the sensitivity analysis.
Conclusion: Clinically significant differences in obstetrical interventions and outcomes do not seem to exist based on the temporal proximity to the attending physician's shift change. Future work should attempt to directly study unit culture and provider fatigue to further investigate opportunities to improve obstetrical quality of care, and additional studies are needed to corroborate these findings in community settings.
Keywords: adverse perinatal outcomes; obstetrical interventions; provider fatigue; quality improvement; quality of care; shift change.
Copyright © 2021 Elsevier Inc. All rights reserved.
Conflict of interest statement
DISCLOSURE: The authors report no conflict of interest.
Figures


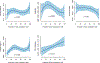

References
-
- Patient safety and quality improvement. 2019. (Accessed November 12, 2019, at www.smfm.org/safety.)
-
- Safe reduction of primary cesarean birth (+AIM) bundle. 2015. (Accessed November 12, 2019, at https://safehealthcareforeverywoman.org/patient-safety-bundles/safe-redu....)
-
- Barber EL, Eisenberg DL, Grobman WA. Type of attending obstetrician call schedule and changes in labor management and outcome. Obstetrics and Gynecology 2011;118:1371–6. - PubMed
-
- Yee L, Liu LY, Grobman WA. Relationship between obstetricians’ cognitive and affective traits and delivery outcomes among women with a prior cesarean. Am J Obstet Gynecol 2015;213:413.e1-7. - PubMed
Publication types
MeSH terms
Grants and funding
- U10 HD040500/HD/NICHD NIH HHS/United States
- UG1 HD027869/HD/NICHD NIH HHS/United States
- UG1 HD040560/HD/NICHD NIH HHS/United States
- UG1 HD053097/HD/NICHD NIH HHS/United States
- UG1 HD027915/HD/NICHD NIH HHS/United States
- U10 HD040485/HD/NICHD NIH HHS/United States
- U10 HD034116/HD/NICHD NIH HHS/United States
- U10 HD027869/HD/NICHD NIH HHS/United States
- U10 HD027917/HD/NICHD NIH HHS/United States
- UG1 HD040485/HD/NICHD NIH HHS/United States
- U10 HD040560/HD/NICHD NIH HHS/United States
- UG1 HD040500/HD/NICHD NIH HHS/United States
- U10 HD040512/HD/NICHD NIH HHS/United States
- U10 HD040545/HD/NICHD NIH HHS/United States
- U10 HD053118/HD/NICHD NIH HHS/United States
- UL1 RR024989/RR/NCRR NIH HHS/United States
- K12 HD050121/HD/NICHD NIH HHS/United States
- U10 HD040544/HD/NICHD NIH HHS/United States
- UL1 TR002548/TR/NCATS NIH HHS/United States
- UL1 RR025764/RR/NCRR NIH HHS/United States
- UG1 HD034116/HD/NICHD NIH HHS/United States
- UG1 HD040544/HD/NICHD NIH HHS/United States
- UG1 HD034208/HD/NICHD NIH HHS/United States
- UG1 HD040512/HD/NICHD NIH HHS/United States
- U10 HD027915/HD/NICHD NIH HHS/United States
- UG1 HD040545/HD/NICHD NIH HHS/United States
- U10 HD034208/HD/NICHD NIH HHS/United States
- U10 HD053097/HD/NICHD NIH HHS/United States
- U10 HD021410/HD/NICHD NIH HHS/United States
- U10 HD036801/HD/NICHD NIH HHS/United States
- U24 HD036801/HD/NICHD NIH HHS/United States
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

