Postdischarge thromboembolic outcomes and mortality of hospitalized patients with COVID-19: the CORE-19 registry
- PMID: 33824972
- PMCID: PMC8032474
- DOI: 10.1182/blood.2020010529
Postdischarge thromboembolic outcomes and mortality of hospitalized patients with COVID-19: the CORE-19 registry
Abstract
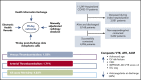
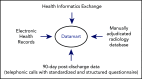
Thromboembolic events, including venous thromboembolism (VTE) and arterial thromboembolism (ATE), and mortality from subclinical thrombotic events occur frequently in coronavirus disease 2019 (COVID-19) inpatients. Whether the risk extends postdischarge has been controversial. Our prospective registry included consecutive patients with COVID-19 hospitalized within our multihospital system from 1 March to 31 May 2020. We captured demographics, comorbidities, laboratory parameters, medications, postdischarge thromboprophylaxis, and 90-day outcomes. Data from electronic health records, health informatics exchange, radiology database, and telephonic follow-up were merged. Primary outcome was a composite of adjudicated VTE, ATE, and all-cause mortality (ACM). Principal safety outcome was major bleeding (MB). Among 4906 patients (53.7% male), mean age was 61.7 years. Comorbidities included hypertension (38.6%), diabetes (25.1%), obesity (18.9%), and cancer history (13.1%). Postdischarge thromboprophylaxis was prescribed in 13.2%. VTE rate was 1.55%; ATE, 1.71%; ΑCM, 4.83%; and MB, 1.73%. Composite primary outcome rate was 7.13% and significantly associated with advanced age (odds ratio [OR], 3.66; 95% CI, 2.84-4.71), prior VTE (OR, 2.99; 95% CI, 2.00-4.47), intensive care unit (ICU) stay (OR, 2.22; 95% CI, 1.78-2.93), chronic kidney disease (CKD; OR, 2.10; 95% CI, 1.47-3.0), peripheral arterial disease (OR, 2.04; 95% CI, 1.10-3.80), carotid occlusive disease (OR, 2.02; 95% CI, 1.30-3.14), IMPROVE-DD VTE score ≥4 (OR, 1.51; 95% CI, 1.06-2.14), and coronary artery disease (OR, 1.50; 95% CI, 1.04-2.17). Postdischarge anticoagulation was significantly associated with reduction in primary outcome (OR, 0.54; 95% CI, 0.47-0.81). Postdischarge VTE, ATE, and ACM occurred frequently after COVID-19 hospitalization. Advanced age, cardiovascular risk factors, CKD, IMPROVE-DD VTE score ≥4, and ICU stay increased risk. Postdischarge anticoagulation reduced risk by 46%.
© 2021 by The American Society of Hematology.
Conflict of interest statement
Conflict-of-interest disclosure: S.L.A. is a current equity holder in Bristol-Myers Squibb and C4 Therapeutics. A.C.S. has consulting for Janssen, Boehringer Ingelheim, Bayer, Bristol-Myers Squibb, Portola, and ATLAS Group and received research funding from Janssen and Boehringer Ingelheim. M.M. has consulted for Bayer and Pfizer and received support for congress attendance from Bayer, Pfizer, and Leo. E.A. has consulted for Bayer and received support for congress attendance from Bayer and Boehringer Ingelheim. The remaining authors declare no competing financial interests.
Figures
References
-
- Spyropoulos AC, Weitz JI. Hospitalized COVID-19 patients and venous thromboembolism: a perfect storm. Circulation. 2020;142(2):129-132. - PubMed
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials
Miscellaneous