ICU Patients' Antibiotic Exposure and Triazole-Resistance in Invasive Candidiasis: Parallel Analysis of Aggregated and Individual Data
- PMID: 33828482
- PMCID: PMC8019904
- DOI: 10.3389/fphar.2021.586893
ICU Patients' Antibiotic Exposure and Triazole-Resistance in Invasive Candidiasis: Parallel Analysis of Aggregated and Individual Data
Abstract
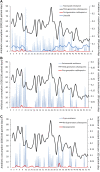
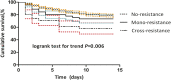
Background: The relationship between antibiotic use and the incidence of triazole-resistant phenotypes of invasive candidiasis (IC) in critically ill patients is unclear. Different methodologies on determining this relationship may yield different results. Methods: A retrospective multicenter observational analysis was conducted to investigate exposure to antibiotics and the incidence of non-duplicate clinical isolates of Candida spp. resistant to fluconazole, voriconazole, or both during November 2013 to April 2018, using two different methodologies: group-level (time-series analysis) and individual-patient-level (regression analysis and propensity-score adjusting). Results: Of 393 identified Candida spp. from 388 critically ill patients, there were three phenotypes of IC identified: fluconazole-resistance (FR, 63, 16.0%); voriconazole-resistance (VR, 46, 11.7%); and cross-resistance between fluconazole and voriconazole (CR, 32, 8.1%). Exposure to several antibacterial agents with activity against the anaerobic gastrointestinal flora, especially third-generation cefalosporins (mainly cefoperazone/sulbactam and ceftriaxone), but not triazoles, have an immediate effect (time lag = 0) on subsequent ICU-acquired triazole-resistant IC in the group-level (p < 0.05). When the same patient database was analyzed at the individual-patient-level, we found that exposure to many antifungal agents was significantly associated with triazole-resistance (fluconazole [adjusted odds ratio (aOR) = 2.73] or caspofungin [aOR = 11.32] on FR, voriconazole [aOR = 2.87] on CR). Compared to the mono-triazole-resistant phenotype, CR IC has worse clinical outcomes (14-days mortality) and a higher level of resistance. Conclusion: Group-level and individual-patient-level analyses of antibiotic-use-versus-resistance relations yielded distinct but valuable results. Antibacterials with antianaerobic activity and antifungals might have "indirect" and "direct" effect on triazole-resistant IC, respectively.
Keywords: critical illness; drug resistance; fungal; invasive candidiasis; regression analysis; time series analysis.
Copyright © 2021 Wang, Zhang, McGuire, Hollingworth, Van Driel, Cao, Wang and Dong.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures
References
-
- de Micheli M., Bille J., Schueller C., Sanglard D. (2002). A common drug-responsive element mediates the upregulation of the candida albicans abc transporters cdr1 and cdr2, two genes involved in antifungal drug resistance. Mol. Microbiol. 43, 1197–1214. 10.1046/j.1365-2958.2002.02814.x - DOI - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources
Miscellaneous

