Effect of caudal bupivacaine alone and with adjuvant fentanyl and nalbuphine to minimize the catheter-related bladder discomfort after tubeless percutaneous nephrolithotomy: A prospective randomized study
- PMID: 33840935
- PMCID: PMC8022066
- DOI: 10.4103/joacp.JOACP_285_18
Effect of caudal bupivacaine alone and with adjuvant fentanyl and nalbuphine to minimize the catheter-related bladder discomfort after tubeless percutaneous nephrolithotomy: A prospective randomized study
Abstract
Background and aims: Catheter-related bladder discomfort (CRBD) is a major cause of postoperative morbidity following urological procedures. The aim of this study was to compare the effect of caudal bupivacaine alone and with adjuvant fentanyl and nalbuphine to minimize the severity of CRBD after tubeless percutaneous nephrolithotomy (PCNL).
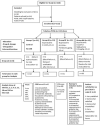
Material and methods: A randomized prospective study was conducted on one hundred thirty-two (American society of Anaesthesiologist physical status I to II) patients who presented for tubeless PCNL under general anesthesia. Patients were randomly divided into four groups control (C), bupivacaine (B), bupivacaine-fentanyl (BF), and bupivacaine-nalbuphine (BN) by using computer-generated codes. All patients received local infiltration at the procedure site while Groups B, BF, and BN received caudal epidural block (CEB) under ultrasound guidance after conclusion of the procedure. Groups B, BF, and BN received bupivacaine alone, bupivacaine-fentanyl, and bupivacaine-nalbuphine, respectively, for CEB. Patients were monitored 24 h for CRBD scale, visual analogue score (VAS), and duration of analgesia at 30 min, 1, 2, 4, 6, 12, 18, and 24 h intervals. The analgesics were supplemented if the CRBD score was >2 and VAS was ≥4. Student t-test, analysis of variance, and Chi-square test were applied for quantitative, within group occurrence, and qualitative analysis respectively.
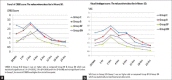
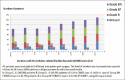
Results: The CRBD scores were considerably lower in the Groups BF and BN as compared to Groups C and B during the first four hours. The duration of analgesia was significantly prolonged in Group BN (475 ± 47 min) versus BF (320 ± 68 min) versus B (104 ± 40 min) versus C (26 ± 14 min).
Conclusions: The severity of CRBD can be reduced with CEB. The effect of CEB can be prolonged with the addition of opioid.
Keywords: Bupivacaine; catheter-related bladder discomfort; caudal epidural block; fentanyl; nalbuphine.
Copyright: © 2021 Journal of Anaesthesiology Clinical Pharmacology.
Conflict of interest statement
There are no conflicts of interest.
Figures

References
-
- Binhas M, Motamed C, Hawajri N, Yiou R, Marty J. Predictors of catheter-related bladder discomfort in the post-anaesthesia care unit. Ann Fr Anesth Reanim. 2011;30:122–5. - PubMed
-
- Agarwal A, Yadav G, Gupta D, Singh PK, Singh U. Evaluation of intra-operative tramadol for prevention of catheter-related bladder discomfort: A prospective, randomized, double-blind study. Br J Anaesth. 2008;101:506–10. - PubMed
-
- Zhang Z, Cao Z, Xu C, Wang H, Zhang C, Pan A, et al. Solifenacin is able to improve the irritative symptoms after transurethral resection of bladder tumors. Urology. 2014;84:117–21. - PubMed
LinkOut - more resources
Full Text Sources
Miscellaneous
