First-line surgery in prolactinomas: lessons from a long-term follow-up study in a tertiary referral center
- PMID: 33847973
- PMCID: PMC8572196
- DOI: 10.1007/s40618-021-01569-6
First-line surgery in prolactinomas: lessons from a long-term follow-up study in a tertiary referral center
Abstract
Context: Although consensus guidelines recommend dopamine agonists (DAs) as the first-line approach in prolactinomas, some patients may opt instead for upfront surgery, with the goal of minimizing the need for continuation of DAs over the long term. While this approach can be recommended in selected patients with a microprolactinoma, the indication for upfront surgery in macroprolactinomas remains controversial, with limited long-term data in large cohorts. We aimed at elucidating whether first-line surgery is equally safe and effective for patients with micro- or macroprolactinomas not extending beyond the median carotid line (i.e., Knosp grade ≤ 1).
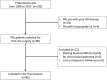
Methodology: Retrospective study of patients with prolactinomas Knosp grade ≤ 1 treated with upfront surgery. The primary endpoint was patients' dependence on DAs at last follow-up. The secondary endpoint was postoperative complications. Independent risk factors for long-term dependence on DAs were analyzed.
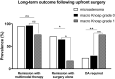
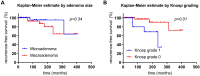
Results: A microadenoma was noted in 45 patients (52%) and a macroadenoma in 41 (48%), with 17 (20%) harboring a Knosp grade 1 prolactinoma. Median follow-up was 80 months. First-line surgery resulted in long-term remission in 31 patients (72%) with a microprolactinoma and in 18 patients (45%) with a macroprolactinoma (p = 0.02). DA therapy was ultimately required in 11 patients (24%) with microadenomas vs. 20 (49%) with macroadenomas (p = 0.03). As for the latter, DA was required in 13 patients (76%) with Knosp grade 1 macroadenomas vs. 7 patients (29%) with Knosp grade 0 macroadenomas (p = 0.004). There was no mortality, and morbidity was minimal. Knosp grade 1 prolactinomas (OR 7.3, 95% CI 1.4-37.7, p = 0.02) but not adenoma size (i.e., macroprolactinomas) were an independent predictor of long-term dependence on DAs.
Conclusions: First-line surgery in patients with microprolactinomas or macroprolactinomas Knosp grade 0 resulted in a good chance of non-dependency on DA therapy. However, in patients with prolactinomas Knosp grade 1, first-line surgery cannot be recommended, as adjuvant DA therapy after surgery is required in the majority of them over the long term.
Keywords: Dopamine agonists; Knosp grading; Long-term outcome; Macroadenoma; Microadenoma; Primary surgical therapy; Prolactinoma.
© 2021. The Author(s).
Conflict of interest statement
This work has not been previously published and is not under consideration for publication anywhere else. The authors report no conflicts of interest concerning the materials or methods used in this study or the findings specified in this paper.
Figures

References
MeSH terms
Substances
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Research Materials

