Perceived Financial Barriers to Cervical Cancer Screening and Associated Cost Burden Among Low-Income, Under-Screened Women
- PMID: 33851854
- PMCID: PMC8558088
- DOI: 10.1089/jwh.2020.8807
Perceived Financial Barriers to Cervical Cancer Screening and Associated Cost Burden Among Low-Income, Under-Screened Women
Abstract
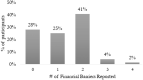
Background: Despite screening's effectiveness in reducing cervical cancer incidence and mortality, disparities in cervical cancer screening uptake remain, with lower rates documented among uninsured and low-income individuals. We examined perceived financial barriers to, and the perceived cost burden of, cervical cancer screening. Materials and Methods: We surveyed 702 low-income, uninsured or publicly insured women ages 25-64 years in North Carolina, U.S., who were not up to date on cervical cancer screening according to national guidelines. Participants were asked about perceived financial barriers to screening and how much they perceived screening would cost. We used multivariable logistic regression to assess the sociodemographic predictors of perceived financial barriers. Results: Seventy-two percent of participants perceived financial barriers to screening. Screening appointment costs (71%) and follow-up/future treatment costs (44%) were most commonly reported, followed by lost pay due to time missed from work (6%) and transportation costs (5%). In multivariable analysis, being uninsured (vs. publicly insured), younger (25-34 vs. 50-64 years), White (vs. Black), and not reporting income data were associated with perceiving screening costs and future treatment costs as barriers to screening. Participants reported wide-ranging estimates of the perceived out-of-pocket cost of screening ($0-$1300), with a median expected cost of $245. Conclusions: The majority of our sample of low-income women perceived substantial financial barriers to screening, particularly related to screening appointment costs and potential follow-up/future treatment costs. Providing greater cost transparency and access to financial assistance may reduce perceived financial barriers to screening, potentially increasing screening uptake among this underserved population. Clinicaltrials.gov registration number NCT02651883.
Keywords: cancer screening; cervical cancer; financial barriers; health disparities; human papillomavirus; under-screened populations.
Conflict of interest statement
J.S.S. has received research grants and consultancies from Hologic, Becton Dickenson, and Trovagene for the past 5 years. A.C.D.M. has had some conference travel expenses covered by Hologic in the last 5 years. S.B.W. has received research grants from Pfizer paid to her institution for unrelated work. All other authors declare no conflicts of interest.
Figures


References
-
- CDC. HPV-Associated Cervical Cancer Rates by Race and Ethnicity. Available at: https://www.cdc.gov/cancer/hpv/statistics/cervical.htm. Published 2019. Updated August 2, 2019. Accessed October 17, 2019.
-
- Beavis AL, Gravitt PE, Rositch AF. Hysterectomy-corrected cervical cancer mortality rates reveal a larger racial disparity in the United States. Cancer 2017;123:1044–1050. - PubMed
-
- Dalton HJ, Farley JH. Racial disparities in cervical cancer: Worse than we thought. Cancer 2017;123:915–916. - PubMed
-
- Leyden WA, Manos MM, Geiger AM, et al. Cervical cancer in women with comprehensive health care access: Attributable factors in the screening process. J Natl Cancer Inst 2005;97:675–683. - PubMed
Publication types
MeSH terms
Associated data
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

