Validation of a Clinical Decision Rule to Predict Abuse in Young Children Based on Bruising Characteristics
- PMID: 33852003
- PMCID: PMC8047759
- DOI: 10.1001/jamanetworkopen.2021.5832
Validation of a Clinical Decision Rule to Predict Abuse in Young Children Based on Bruising Characteristics
Erratum in
-
Error in Figure Legend.JAMA Netw Open. 2021 Sep 1;4(9):e2130136. doi: 10.1001/jamanetworkopen.2021.30136. JAMA Netw Open. 2021. PMID: 34505892 Free PMC article. No abstract available.
Abstract
Importance: Bruising caused by physical abuse is the most common antecedent injury to be overlooked or misdiagnosed as nonabusive before an abuse-related fatality or near-fatality in a young child. Bruising occurs from both nonabuse and abuse, but differences identified by a clinical decision rule may allow improved and earlier recognition of the abused child.
Objective: To refine and validate a previously derived bruising clinical decision rule (BCDR), the TEN-4 (bruising to torso, ear, or neck or any bruising on an infant <4.99 months of age), for identifying children at risk of having been physically abused.
Design, setting, and participants: This prospective cross-sectional study was conducted from December 1, 2011, to March 31, 2016, at emergency departments of 5 urban children's hospitals. Children younger than 4 years with bruising were identified through deliberate examination. Statistical analysis was completed in June 2020.
Exposures: Bruising characteristics in 34 discrete body regions, patterned bruising, cumulative bruise counts, and patient's age. The BCDR was refined and validated based on these variables using binary recursive partitioning analysis.
Main outcomes and measures: Injury from abusive vs nonabusive trauma was determined by the consensus judgment of a multidisciplinary expert panel.
Results: A total of 21 123 children were consecutively screened for bruising, and 2161 patients (mean [SD] age, 2.1 [1.1] years; 1296 [60%] male; 1785 [83%] White; 1484 [69%] non-Hispanic/Latino) were enrolled. The expert panel achieved consensus on 2123 patients (98%), classifying 410 (19%) as abuse and 1713 (79%) as nonabuse. A classification tree was fit to refine the rule and validated via bootstrap resampling. The resulting BCDR was 95.6% (95% CI, 93.0%-97.3%) sensitive and 87.1% (95% CI, 85.4%-88.6%) specific for distinguishing abuse from nonabusive trauma based on body region bruised (torso, ear, neck, frenulum, angle of jaw, cheeks [fleshy], eyelids, and subconjunctivae), bruising anywhere on an infant 4.99 months and younger, or patterned bruising (TEN-4-FACESp).
Conclusions and relevance: In this study, an affirmative finding for any of the 3 BCDR TEN-4-FACESp components in children younger than 4 years indicated a potential risk for abuse; these results warrant further evaluation. Clinical application of this tool has the potential to improve recognition of abuse in young children with bruising.
Conflict of interest statement
Figures
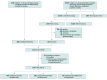


Comment in
-
To Recognize Child Physical Abuse Early, Frontline Clinicians Need Subspecialty Expertise.JAMA Netw Open. 2021 Apr 1;4(4):e215947. doi: 10.1001/jamanetworkopen.2021.5947. JAMA Netw Open. 2021. PMID: 33852006 No abstract available.
References
-
- US Department of Health and Human Services, Administration for Children and Families, Administration on Children, Youth and Families, Children’s Bureau . Child maltreatment. 2018. Accessed September 25, 2020. https://www.acf.hhs.gov/cb/report/child-maltreatment-2018
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

