Sexism-Related Stigma Affects Pain Perception
- PMID: 33854543
- PMCID: PMC8019650
- DOI: 10.1155/2021/6612456
Sexism-Related Stigma Affects Pain Perception
Abstract
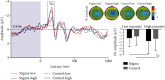
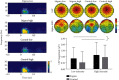
People with stigmatized characteristics tend to be devalued by others in a given society. The negative experiences related to stigma cause individuals to struggle as they would if they were in physical pain and bring various negative outcomes in the way that physical pain does. However, it is unclear whether stigma related to one's identity would affect their perception of physical pain. To address this issue, using sexism-related paradigms, we found that females had reduced pain threshold/tolerance in the Cold Pressor Test (Experiment 1) and an increased rating for nociceptive laser stimuli with fixed intensity (Experiment 2). Additionally, we observed that there was a larger laser-evoked N1, an early laser-evoked P2, and a larger magnitude of low-frequency component in laser-evoked potentials (LEPs) in the stigma condition than in the control condition (Experiment 3). Our study provides behavioral and electrophysiological evidence that sexism-related stigma affects the pain perception of females.
Copyright © 2021 Ming Zhang et al.
Conflict of interest statement
The authors declare that there is no conflict of interest regarding the publication of this paper.
Figures



Similar articles
-
Focal Mechanical Vibration Does not Change Laser-Pain Perception and Laser-Evoked Potentials: A Pilot Study.Pain Pract. 2017 Jan;17(1):25-31. doi: 10.1111/papr.12417. Epub 2016 Feb 19. Pain Pract. 2017. PMID: 26892176 Clinical Trial.
-
Cortical inhibition of laser pain and laser-evoked potentials by non-nociceptive somatosensory input.Eur J Neurosci. 2015 Oct;42(7):2407-14. doi: 10.1111/ejn.13035. Epub 2015 Aug 24. Eur J Neurosci. 2015. PMID: 26227011
-
Effects of aging on laser evoked potentials.Muscle Nerve. 2015 May;51(5):736-42. doi: 10.1002/mus.24458. Epub 2015 Mar 31. Muscle Nerve. 2015. PMID: 25212497
-
Cortical integration of bilateral nociceptive signals: when more is less.Pain. 2019 Mar;160(3):724-733. doi: 10.1097/j.pain.0000000000001451. Pain. 2019. PMID: 30507784
-
The Analgesic Effect of Oxytocin in Humans: A Double-Blind, Placebo-Controlled Cross-Over Study Using Laser-Evoked Potentials.J Neuroendocrinol. 2016 Apr;28(4):10.1111/jne.12347. doi: 10.1111/jne.12347. J Neuroendocrinol. 2016. PMID: 26660859 Free PMC article. Clinical Trial.
Cited by
-
Endometriosis in later life: an intersectional analysis from the perspective of epistemic injustice.Med Health Care Philos. 2025 Mar;28(1):151-159. doi: 10.1007/s11019-024-10245-4. Epub 2024 Dec 20. Med Health Care Philos. 2025. PMID: 39704896 Free PMC article.
-
The dual facilitatory and inhibitory effects of social pain on physical pain perception.iScience. 2024 Jan 18;27(2):108951. doi: 10.1016/j.isci.2024.108951. eCollection 2024 Feb 16. iScience. 2024. PMID: 38323007 Free PMC article.
-
A Narrative Review of the Current Research in Cancer-Related Pain Inequities: The Necessity of Applying Intersectionality to Advance Cancer Pain Research.Cancer Control. 2024 Jan-Dec;31:10732748241274256. doi: 10.1177/10732748241274256. Cancer Control. 2024. PMID: 39172777 Free PMC article. Review.
-
The alterations in event-related potential responses to pain empathy in breast cancer survivors treated with chemotherapy.Front Psychol. 2022 Sep 23;13:942036. doi: 10.3389/fpsyg.2022.942036. eCollection 2022. Front Psychol. 2022. PMID: 36211858 Free PMC article.
-
Autism, menstruation and mental health- a scoping review and a call to action.Front Glob Womens Health. 2025 Jun 25;6:1531934. doi: 10.3389/fgwh.2025.1531934. eCollection 2025. Front Glob Womens Health. 2025. PMID: 40635787 Free PMC article.
References
-
- Goffman E. Stigma: Notes on the Management of Spoiled Identity. New York: Simon & Schuster; 1963.
-
- Richman L. S., Martin J., Guadagno J. Stigma-based rejection and the detection of signs of acceptance. Social Psychological and Personality Science. 2015;7(1):53–60. doi: 10.1177/1948550615598376. - DOI
-
- Owens M., Okunbor J., Rainey R., et al. (279) The impact of disease-specific internalized stigma on depressive symptoms, pain catastrophizing, pain interference, and alcohol use in people living with HIV and chronic pain (PLWH-CP) Journal of Pain. 2017;18(4):p. S45. doi: 10.1016/j.jpain.2017.02.172. - DOI
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

