The Multidimensional Assessment for Pediatric Patients in Radiotherapy (M.A.P.-RT) Tool for Customized Treatment Preparation: RADAR Project
- PMID: 33854964
- PMCID: PMC8039366
- DOI: 10.3389/fonc.2021.621690
The Multidimensional Assessment for Pediatric Patients in Radiotherapy (M.A.P.-RT) Tool for Customized Treatment Preparation: RADAR Project
Abstract
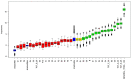
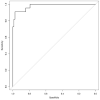
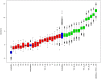
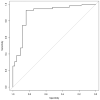
Aims: Pediatric patients may experience considerable distress during radiotherapy. Combining psychological interventions with standard therapies can reduce the need for sedation. The RADAR Project aims to use a systematic method of recording data that can reveal patients' difficulties and fragility during treatment. In this context, the aim of our study was to investigate the ability of a multidimensional assessment tool (M.A.P.-RT schedule) to predict the need for sedation during radiotherapy. The schedule, which is administered during the first evaluation, was created to collect information on patients and their families in a standardized way. Materials and Methods: The study enrolled pediatric patients (aged 0-18 years or 18-21 with cognitive impairment). Data were collected by means of the M.A.P.-RT module; this explores various thematic areas, and is completed by the radiation oncologist, psychologist and nurse during their first evaluation. Features were selected by means of the Boruta method (random forest classifier), and the totals of the significant partial scores on each subsection of the module were inserted into a logistic model in order to test for their correlation with the use of anesthesia and with the frequency of psychological support. The results of logistic regression (LR) were used to identify the best predictors. The AUC was used to identify the best threshold for the scores in the evaluation. Results: A total of 99 patients were considered for this analysis. The feature that best predicted both the need for anesthesia and the frequency of psychological support was the total score (TS), the AUC of the ROC being 0.9875 for anesthesia and 0.8866 for psychological support. Conclusion: During the first evaluation, the M.A.P.-RT form can predict the need for anesthesia in pediatric patients, and is a potential tool for personalizing therapeutic and management procedures.
Keywords: anesthesia; children; distress; pediatrics; psychological support; radiotherapy.
Copyright © 2021 Chiesa, Marconi, Dinapoli, Sanfilippo, Ruggiero, Mastronuzzi, Panza, Serra, Massaccesi, Cacchione, Beghella Bartoli, Chieffo, Gambacorta, Valentini and Balducci.
Conflict of interest statement
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Figures


References
-
- Pisani P, Buzzoni C, Crocetti E, Dal Maso L, Rondelli R, Alessi D. Italian Cancer Figures - Report 2012 Cancer in children and adolescents AIRTUM Working Group and AIEOP Working Group. Epidemiol Prev. (2013) 37:1–296. - PubMed
LinkOut - more resources
Full Text Sources
Other Literature Sources

