Co-infection in critically ill patients with COVID-19: an observational cohort study from England
- PMID: 33861190
- PMCID: PMC8289210
- DOI: 10.1099/jmm.0.001350
Co-infection in critically ill patients with COVID-19: an observational cohort study from England
Abstract
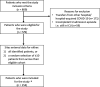
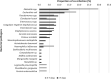
Introduction. During previous viral pandemics, reported co-infection rates and implicated pathogens have varied. In the 1918 influenza pandemic, a large proportion of severe illness and death was complicated by bacterial co-infection, predominantly Streptococcus pneumoniae and Staphylococcus aureus.Gap statement. A better understanding of the incidence of co-infection in patients with COVID-19 infection and the pathogens involved is necessary for effective antimicrobial stewardship.Aim. To describe the incidence and nature of co-infection in critically ill adults with COVID-19 infection in England.Methodology. A retrospective cohort study of adults with COVID-19 admitted to seven intensive care units (ICUs) in England up to 18 May 2020, was performed. Patients with completed ICU stays were included. The proportion and type of organisms were determined at <48 and >48 h following hospital admission, corresponding to community and hospital-acquired co-infections.Results. Of 254 patients studied (median age 59 years (IQR 49-69); 64.6 % male), 139 clinically significant organisms were identified from 83 (32.7 %) patients. Bacterial co-infections/ co-colonisation were identified within 48 h of admission in 14 (5.5 %) patients; the commonest pathogens were Staphylococcus aureus (four patients) and Streptococcus pneumoniae (two patients). The proportion of pathogens detected increased with duration of ICU stay, consisting largely of Gram-negative bacteria, particularly Klebsiella pneumoniae and Escherichia coli. The co-infection/ co-colonisation rate >48 h after admission was 27/1000 person-days (95 % CI 21.3-34.1). Patients with co-infections/ co-colonisation were more likely to die in ICU (crude OR 1.78,95 % CI 1.03-3.08, P=0.04) compared to those without co-infections/ co-colonisation.Conclusion. We found limited evidence for community-acquired bacterial co-infection in hospitalised adults with COVID-19, but a high rate of Gram-negative infection acquired during ICU stay.
Keywords: COVID-19; ICU; antibiotic resistance; co-infection.
Conflict of interest statement
Professor Lim reports grants from National Institute for Health Research (NIHR), grants from Pfizer, outside the submitted work. Paul Dark is funded by NIHR Manchester BRC as sub-theme lead in Respiratory Infections.
Figures
References
-
- WHO WHO Covid-19 Dashboard 2020 [02/06/20]. Available from. https://covid19.who.int/?gclid=CjwKCAjw8df2BRA3EiwAvfZWaJWnmCWZBUjJdJZGV...
Publication types
MeSH terms
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical
Miscellaneous

