Attributable mortality of acute respiratory distress syndrome: a systematic review, meta-analysis and survival analysis using targeted minimum loss-based estimation
- PMID: 33863829
- PMCID: PMC10318350
- DOI: 10.1136/thoraxjnl-2020-215950
Attributable mortality of acute respiratory distress syndrome: a systematic review, meta-analysis and survival analysis using targeted minimum loss-based estimation
Abstract
Background: Although acute respiratory distress syndrome (ARDS) is associated with high mortality, its direct causal link with death is unclear. Clarifying this link is important to justify costly research on prevention of ARDS.
Objective: To estimate the attributable mortality, if any, of ARDS.
Design: First, we performed a systematic review and meta-analysis of observational studies reporting mortality of critically ill patients with and without ARDS matched for underlying risk factor. Next, we conducted a survival analysis of prospectively collected patient-level data from subjects enrolled in three intensive care unit (ICU) cohorts to estimate the attributable mortality of critically ill septic patients with and without ARDS using a novel causal inference method.
Results: In the meta-analysis, 44 studies (47 cohorts) involving 56 081 critically ill patients were included. Mortality was higher in patients with versus without ARDS (risk ratio 2.48, 95% CI 1.86 to 3.30; p<0.001) with a numerically stronger association between ARDS and mortality in trauma than sepsis. In the survival analysis of three ICU cohorts enrolling 1203 critically ill patients, 658 septic patients were included. After controlling for confounders, ARDS was found to increase the mortality rate by 15% (95% CI 3% to 26%; p=0.015). Significant increases in mortality were seen for severe (23%, 95% CI 3% to 44%; p=0.028) and moderate (16%, 95% CI 2% to 31%; p=0.031), but not for mild ARDS.
Conclusions: ARDS has a direct causal link with mortality. Our findings provide information about the extent to which continued funding of ARDS prevention trials has potential to impart survival benefit.
Prospero registration number: CRD42017078313.
Keywords: ARDS; clinical epidemiology; critical care.
© Author(s) (or their employer(s)) 2021. No commercial re-use. See rights and permissions. Published by BMJ.
Conflict of interest statement
Competing interests: AMKC is a cofounder and stock holder of and serves on the Scientific Advisory Board for Proterris, which develops therapeutic uses for carbon monoxide. He also has a use patent on carbon monoxide. He served as a consultant for an advisory board meeting of Teva Pharmaceutical Industries, July 2018. RMB serves on the Advisory Board for Merck. LEF reports clinical trials support from Asahi Kasei Pharma America. None declared: LKT, KH, CO, ID, JSH, EJS, DRP, LG-E, AH, MPV, JWH and IIS.
Figures


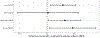
References
-
- National Heart L, and Blood Institute website. Lung Diseases [Available from: https://www.nhlbi.nih.gov/science/lung-diseases accessed September 7, 2018.
-
- Injury PEToAL. PETAL Network [Available from: http://petalnet.org/ accessed September 7, 2018.
-
- Ferring M, Vincent J. Is outcome from ARDS related to the severity of respiratory failure? European Respiratory Journal 1997;10(6):1297–300. - PubMed
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
