Clinical and volumetric predictors of local control after robotic stereotactic radiosurgery for cerebral metastases: active systemic disease may affect local control in the brain
- PMID: 33885238
- PMCID: PMC7877264
- DOI: 10.2478/raon-2020-0065
Clinical and volumetric predictors of local control after robotic stereotactic radiosurgery for cerebral metastases: active systemic disease may affect local control in the brain
Abstract
Background: The aim of the study was to assess the association between physical and biological dose normalized to volume of the metastatic tumor as well as clinical factors with local control in patients with brain metastases who underwent robotic stereotactic radiosurgery.
Patients and methods: A cohort of 69 patients consecutively treated with robotic radiosurgery between 2011 and 2016 was analyzed. The patients were treated with either single fraction radiosurgery or hypofractionated regimens. Biologically effective dose (BED) was calculated assuming alpha/beta value = 10 and both physical dose and BED were normalized to the tumor volume to allow dose-volume effect evaluation. Moreover, clinical and treatment-related variables were evaluated to asses association with local control.
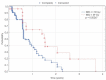
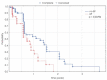
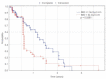
Results: A total of 133 tumors were irradiated and their volumes ranged between 0.001 and 46.99 cm3. Presence of extracranial progression was associated with worse local control whereas higher total dose, BED10 > 59 Gy and single metastasis predicted statistically significantly better local outcome. BED10/cm3 > 36 Gy, and BED2 > 60 Gy negatively affected local control in univariate analysis. In multivariate analysis performed on all these variables, presence of a single metastasis, BED10 > 59 Gy and extracranial progression retained their significance. Excluding a priori the BED2/ cm3 parameter resulted with a Cox model confirming significance of all remaining variables.
Conclusions: Hypofractionated treatment schemes have similar efficiency to single fraction treatment in terms of local control and the effect depends on BED irrespective of fractionation schedule. Effective control of extracranial sites of the disease is associated with higher probability of local control in the brain which in turn is consistently lower in patients with multiple lesions.
Keywords: brain metastases; local control; radiobiology; radiosurgery.
© 2021 Sławomir Blamek, Magdalena Stankiewicz, Bogusław Maciejewski, published by Sciendo.
Figures

Similar articles
-
A Dose-Volume Response Model for Brain Metastases Treated With Frameless Single-Fraction Robotic Radiosurgery: Seeking to Better Predict Response to Treatment.Technol Cancer Res Treat. 2017 Jun;16(3):344-351. doi: 10.1177/1533034616685025. Epub 2016 Dec 27. Technol Cancer Res Treat. 2017. PMID: 28027696 Free PMC article.
-
Impact of 2-staged stereotactic radiosurgery for treatment of brain metastases ≥ 2 cm.J Neurosurg. 2018 Aug;129(2):366-382. doi: 10.3171/2017.3.JNS162532. Epub 2017 Sep 22. J Neurosurg. 2018. PMID: 28937324
-
Postoperative hypofractionated stereotactic brain radiation (HSRT) for resected brain metastases: improved local control with higher BED10.J Neurooncol. 2018 Sep;139(2):449-454. doi: 10.1007/s11060-018-2885-6. Epub 2018 May 10. J Neurooncol. 2018. PMID: 29749569
-
Congress of Neurological Surgeons Systematic Review and Evidence-Based Guidelines on the Role of Whole Brain Radiation Therapy in Adults With Newly Diagnosed Metastatic Brain Tumors.Neurosurgery. 2019 Mar 1;84(3):E159-E162. doi: 10.1093/neuros/nyy541. Neurosurgery. 2019. PMID: 30629211
-
Tumor Control Probability of Radiosurgery and Fractionated Stereotactic Radiosurgery for Brain Metastases.Int J Radiat Oncol Biol Phys. 2021 May 1;110(1):53-67. doi: 10.1016/j.ijrobp.2020.10.034. Epub 2020 Dec 31. Int J Radiat Oncol Biol Phys. 2021. PMID: 33390244 Review.
Cited by
-
Factors associated with the local control of brain metastases: a systematic search and machine learning application.BMC Med Inform Decis Mak. 2024 Jun 21;24(1):177. doi: 10.1186/s12911-024-02579-z. BMC Med Inform Decis Mak. 2024. PMID: 38907265 Free PMC article.
References
MeSH terms
LinkOut - more resources
Full Text Sources
Medical
