AI-based analysis of CT images for rapid triage of COVID-19 patients
- PMID: 33888856
- PMCID: PMC8062628
- DOI: 10.1038/s41746-021-00446-z
AI-based analysis of CT images for rapid triage of COVID-19 patients
Abstract
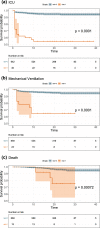
The COVID-19 pandemic overwhelms the medical resources in the stressed intensive care unit (ICU) capacity and the shortage of mechanical ventilation (MV). We performed CT-based analysis combined with electronic health records and clinical laboratory results on Cohort 1 (n = 1662 from 17 hospitals) with prognostic estimation for the rapid stratification of PCR confirmed COVID-19 patients. These models, validated on Cohort 2 (n = 700) and Cohort 3 (n = 662) constructed from nine external hospitals, achieved satisfying performance for predicting ICU, MV, and death of COVID-19 patients (AUROC 0.916, 0.919, and 0.853), even on events happened two days later after admission (AUROC 0.919, 0.943, and 0.856). Both clinical and image features showed complementary roles in prediction and provided accurate estimates to the time of progression (p < 0.001). Our findings are valuable for optimizing the use of medical resources in the COVID-19 pandemic. The models are available here: https://github.com/terryli710/COVID_19_Rapid_Triage_Risk_Predictor .
Conflict of interest statement
The authors declare no competing interests.
Figures




Update of
-
CT-based Rapid Triage of COVID-19 Patients: Risk Prediction and Progression Estimation of ICU Admission, Mechanical Ventilation, and Death of Hospitalized Patients.medRxiv [Preprint]. 2020 Nov 6:2020.11.04.20225797. doi: 10.1101/2020.11.04.20225797. medRxiv. 2020. Update in: NPJ Digit Med. 2021 Apr 22;4(1):75. doi: 10.1038/s41746-021-00446-z. PMID: 33173894 Free PMC article. Updated. Preprint.
References
-
- WHO. Weekly Epidemiological and Operational updates October. https://www.who.int/docs/default-source/coronaviruse/situation-reports/2... (2020).
-
- Harvard Business Review. We need to relocate ICU patients out of Covid-19 hotspots. https://hbr.org/2020/06/we-need-to-relocate-icu-patients-out-of-covid-19... (2020).
-
- BBC News. Coronavirus: thousands of extra hospital beds and staff. https://www.bbc.com/news/uk-51989183 (2020).
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

