Income-related health inequality among Chinese adults during the COVID-19 pandemic: evidence based on an online survey
- PMID: 33902603
- PMCID: PMC8072088
- DOI: 10.1186/s12939-021-01448-9
Income-related health inequality among Chinese adults during the COVID-19 pandemic: evidence based on an online survey
Abstract
Background: Partial- or full-lockdowns, among other interventions during the COVID-19 pandemic, may disproportionally affect people (their behaviors and health outcomes) with lower socioeconomic status (SES). This study examines income-related health inequalities and their main contributors in China during the pandemic.
Methods: The 2020 China COVID-19 Survey is an anonymous 74-item survey administered via social media in China. A national sample of 10,545 adults in all 31 provinces, municipalities, and autonomous regions in mainland China provided comprehensive data on sociodemographic characteristics, awareness and attitudes towards COVID-19, lifestyle factors, and health outcomes during the lockdown. Of them, 8448 subjects provided data for this analysis. Concentration Index (CI) and Corrected CI (CCI) were used to measure income-related inequalities in mental health and self-reported health (SRH), respectively. Wagstaff-type decomposition analysis was used to identify contributors to health inequalities.
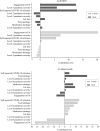
Results: Most participants reported their health status as "very good" (39.0%) or "excellent" (42.3%). CCI of SRH and mental health were - 0.09 (p < 0.01) and 0.04 (p < 0.01), respectively, indicating pro-poor inequality in ill SRH and pro-rich inequality in ill mental health. Income was the leading contributor to inequalities in SRH and mental health, accounting for 62.7% (p < 0.01) and 39.0% (p < 0.05) of income-related inequalities, respectively. The COVID-19 related variables, including self-reported family-member COVID-19 infection, job loss, experiences of food and medication shortage, engagement in physical activity, and five different-level pandemic regions of residence, explained substantial inequalities in ill SRH and ill mental health, accounting for 29.7% (p < 0.01) and 20.6% (p < 0.01), respectively. Self-reported family member COVID-19 infection, experiencing food and medication shortage, and engagement in physical activity explain 9.4% (p < 0.01), 2.6% (the summed contributions of experiencing food shortage (0.9%) and medication shortage (1.7%), p < 0.01), and 17.6% (p < 0.01) inequality in SRH, respectively (8.9% (p < 0.01), 24.1% (p < 0.01), and 15.1% (p < 0.01) for mental health).
Conclusions: Per capita household income last year, experiences of food and medication shortage, self-reported family member COVID-19 infection, and physical activity are important contributors to health inequalities, especially mental health in China during the COVID-19 pandemic. Intervention programs should be implemented to support vulnerable groups.
Keywords: COVID-19; China; Health inequality; Mental health; Socioeconomic status.
Conflict of interest statement
None declared.
Figures
References
-
- World Health Organization . Ten threats to global health in 2019. 2019.
-
- World Health Organization . Weekly epidemiological update - 9 March 2021. Geneva: World Health Organization; 2021.
-
- Qian Y, Fan W. Who loses income during the COVID-19 outbreak? Evidence from China. Res Soc Stratif Mobil. 2020;68:100522.
Publication types
MeSH terms
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical