A Mobile Phone-Based Intervention to Reduce Mental Health Problems in Health Care Workers During the COVID-19 Pandemic (PsyCovidApp): Randomized Controlled Trial
- PMID: 33909587
- PMCID: PMC8133164
- DOI: 10.2196/27039
A Mobile Phone-Based Intervention to Reduce Mental Health Problems in Health Care Workers During the COVID-19 Pandemic (PsyCovidApp): Randomized Controlled Trial
Abstract
Background: The global health emergency generated by the COVID-19 pandemic is posing an unprecedented challenge to health care workers, who are facing heavy workloads under psychologically difficult situations. Mental mobile Health (mHealth) interventions are now being widely deployed due to their attractive implementation features, despite the lack of evidence about their efficacy in this specific population and context.
Objective: The aim of this trial is to evaluate the effectiveness of a psychoeducational, mindfulness-based mHealth intervention to reduce mental health problems in health care workers during the COVID-19 pandemic.
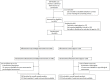
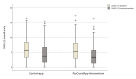
Methods: We conducted a blinded, parallel-group, controlled trial in Spain. Health care workers providing face-to-face health care to patients with COVID-19 were randomly assigned (1:1) to receive the PsyCovidApp intervention (an app targeting emotional skills, healthy lifestyle behavior, burnout, and social support) or a control app (general recommendations about mental health care) for 2 weeks. The participants were blinded to their group allocation. Data were collected telephonically at baseline and after 2 weeks by trained health psychologists. The primary outcome was a composite of depression, anxiety, and stress (overall score on the Depression Anxiety Stress Scale-21 [DASS-21]). Secondary outcomes were insomnia (Insomnia Severity Index), burnout (Maslach Burnout Inventory Human Services Survey), posttraumatic stress (Davidson Trauma Scale), self-efficacy (General Self-Efficacy Scale), and DASS-21 individual scale scores. Differences between groups were analyzed using general linear modeling according to an intention-to-treat protocol. Additionally, we measured the usability of the PsyCovidApp (System Usability Scale). The outcome data collectors and trial statisticians were unaware of the treatment allocation.
Results: Between May 14 and July 25, 2020, 482 health care workers were recruited and randomly assigned to PsyCovidApp (n=248) or the control app (n=234). At 2 weeks, complete outcome data were available for 436/482 participants (90.5%). No significant differences were observed between the groups at 2 weeks in the primary outcome (standardized mean difference -0.04; 95% CI -0.11 to 0.04; P=.15) or in the other outcomes. In our prespecified subgroup analyses, we observed significant improvements among health care workers consuming psychotropic medications (n=79) in the primary outcome (-0.29; 95% CI -0.48 to -0.09; P=.004), and in posttraumatic stress, insomnia, anxiety, and stress. Similarly, among health care workers receiving psychotherapy (n=43), we observed improvements in the primary outcome (-0.25; 95% CI -0.49 to -0.02; P=.02), and in insomnia, anxiety, and stress. The mean usability score of PsyCovidApp was high (87.21/100, SD 12.65). After the trial, 208/221 participants in the intervention group (94.1%) asked to regain access to PsyCovidApp, indicating high acceptability.
Conclusions: In health care workers assisting patients with COVID-19 in Spain, PsyCovidApp, compared with a control app, reduced mental health problems at 2 weeks only among health care workers receiving psychotherapy or psychotropic medications.
Trial registration: ClinicalTrials.gov NCT04393818; https://clinicaltrials.gov/ct2/show/NCT04393818.
Keywords: COVID-19; app; health care workers; mHealth; mental health; randomized controlled trial.
©Maria Antònia Fiol-DeRoque, Maria Jesús Serrano-Ripoll, Rafael Jiménez, Rocío Zamanillo-Campos, Aina María Yáñez-Juan, Miquel Bennasar-Veny, Alfonso Leiva, Elena Gervilla, M Esther García-Buades, Mauro García-Toro, Pablo Alonso-Coello, Guadalupe Pastor-Moreno, Isabel Ruiz-Pérez, Carolina Sitges, Javier García-Campayo, Joan Llobera-Cánaves, Ignacio Ricci-Cabello. Originally published in JMIR mHealth and uHealth (https://mhealth.jmir.org), 18.05.2021.
Conflict of interest statement
Conflicts of Interest: MJSR, AMYJ, MBV, MEGB, MGT, CS, RJ, EG, and JGC developed the contents of the intervention. All other authors have no conflicts to declare.
Figures


References
-
- COVID-19 Weekly Epidemiological Update. World Health Organization. 2020. Nov 15, [2021-05-11]. https://www.who.int/publications/m/item/weekly-epidemiological-update---....
-
- Kang L, Li Y, Hu S, Chen M, Yang C, Yang BX, Wang Y, Hu J, Lai J, Ma X, Chen J, Guan L, Wang G, Ma H, Liu Z. The mental health of medical workers in Wuhan, China dealing with the 2019 novel coronavirus. Lancet Psychiatry. 2020 Mar;7(3):e14. doi: 10.1016/S2215-0366(20)30047-X. http://europepmc.org/abstract/MED/32035030 - DOI - PMC - PubMed
-
- Serrano-Ripoll MJ, Meneses-Echavez JF, Ricci-Cabello I, Fraile-Navarro D, Fiol-deRoque MA, Pastor-Moreno G, Castro A, Ruiz-Pérez Isabel, Zamanillo Campos R, Gonçalves-Bradley Daniela C. Impact of viral epidemic outbreaks on mental health of healthcare workers: a rapid systematic review and meta-analysis. J Affect Disord. 2020 Dec 01;277:347–357. doi: 10.1016/j.jad.2020.08.034. http://europepmc.org/abstract/MED/32861835 - DOI - PMC - PubMed
-
- Kisely S, Warren N, McMahon L, Dalais C, Henry I, Siskind D. Occurrence, prevention, and management of the psychological effects of emerging virus outbreaks on healthcare workers: rapid review and meta-analysis. BMJ. 2020 May 05;369:m1642. doi: 10.1136/bmj.m1642. http://www.bmj.com/lookup/pmidlookup?view=long&pmid=32371466 - DOI - PMC - PubMed
-
- Bandyopadhyay S, Baticulon RE, Kadhum M, Alser M, Ojuka DK, Badereddin Y, Kamath A, Parepalli SA, Brown G, Iharchane S, Gandino S, Markovic-Obiago Z, Scott S, Manirambona E, Machhada A, Aggarwal A, Benazaize L, Ibrahim M, Kim D, Tol I, Taylor EH, Knighton A, Bbaale D, Jasim D, Alghoul H, Reddy H, Abuelgasim H, Saini K, Sigler A, Abuelgasim L, Moran-Romero M, Kumarendran M, Jamie NA, Ali O, Sudarshan R, Dean R, Kissyova R, Kelzang S, Roche S, Ahsan T, Mohamed Y, Dube AM, Gwini GP, Gwokyala R, Brown R, Papon MRKK, Li Z, Ruzats SS, Charuvila S, Peter N, Khalidy K, Moyo N, Alser O, Solano A, Robles-Perez E, Tariq A, Gaddah M, Kolovos S, Muchemwa FC, Saleh A, Gosman A, Pinedo-Villanueva R, Jani A, Khundkar R. Infection and mortality of healthcare workers worldwide from COVID-19: a systematic review. BMJ Glob Health. 2020 Dec;5(12) doi: 10.1136/bmjgh-2020-003097. https://gh.bmj.com/lookup/pmidlookup?view=long&pmid=33277297 - DOI - PMC - PubMed
Publication types
MeSH terms
Associated data
LinkOut - more resources
Full Text Sources
Other Literature Sources
Medical

