Lymphaticovenous Anastomosis Supermicrosurgery Decreases Oxidative Stress and Increases Antioxidant Capacity in the Serum of Lymphedema Patients
- PMID: 33917571
- PMCID: PMC8038828
- DOI: 10.3390/jcm10071540
Lymphaticovenous Anastomosis Supermicrosurgery Decreases Oxidative Stress and Increases Antioxidant Capacity in the Serum of Lymphedema Patients
Abstract
Background: Excess lymphedematous tissue causes excessive oxidative stress in lymphedema. Lymphaticovenous anastomosis (LVA) supermicrosurgery is currently emerging as the first-line surgical intervention for lymphedema. No data are available regarding the changes in serum proteins correlating to oxidative stress and antioxidant capacity before and after LVA.
Methods: A total of 26 patients with unilateral lower limb lymphedema confirmed by lymphoscintigraphy were recruited, and venous serum samples were collected before (pre-LVA) and after LVA (post-LVA). In 16 patients, the serum proteins were identified by isobaric tags for relative and absolute quantitation-based quantitative proteomic analysis with subsequent validation of protein expression by enzyme-linked immunosorbent assay. An Oxidative Stress Panel Kit was used on an additional 10 patients. Magnetic resonance (MR) volumetry was used to measure t limb volume six months after LVA.
Results: This study identified that catalase (CAT) was significantly downregulated after LVA (pre-LVA vs. post-LVA, 2651 ± 2101 vs. 1448 ± 593 ng/mL, respectively, p = 0.033). There were significantly higher levels of post-LVA serum total antioxidant capacity (pre-LVA vs. post-LVA, 441 ± 81 vs. 488 ± 59 µmole/L, respectively, p = 0.031) and glutathione peroxidase (pre-LVA vs. post-LVA, 73 ± 20 vs. 92 ± 29 U/g, respectively, p = 0.018) than pre-LVA serum. In addition, after LVA, there were significantly more differences between post-LVA and pre-LVA serum levels of CAT (good outcome vs. fair outcome, -2593 ± 2363 vs. 178 ± 603 ng/mL, respectively, p = 0.021) and peroxiredoxin-2 (PRDX2) (good outcome vs. fair outcome, -7782 ± 7347 vs. -397 ± 1235 pg/mL, respectively, p = 0.037) in those patients with good outcomes (≥40% volume reduction in MR volumetry) than those with fair outcomes (<40% volume reduction in MR volumetry).
Conclusions: The study revealed that following LVA, differences in some specific oxidative stress markers and antioxidant capacity can be found in the serum of patients with lymphedema.
Keywords: Enzyme-linked immunosorbent assay (ELISA); LVA; antioxidant; iTRAQ; lymphaticovenous anastomosis; lymphedema; lymphovenous bypass (LVB); oxidative stress; reactive oxygen species (ROS).
Conflict of interest statement
None of the authors has a financial interest in any of the products, devices, or drugs mentioned in this manuscript. The authors declare no conflict of interest.
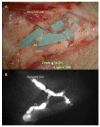
Figures

Similar articles
-
Lower Limb Lymphedema Patients Can Still Benefit from Supermicrosurgical Lymphaticovenous Anastomosis (LVA) after Vascularized Lymph Node Flap Transfer (VLNT) as Delayed Lymphatic Reconstruction-A Retrospective Cohort Study.J Clin Med. 2021 Jul 15;10(14):3121. doi: 10.3390/jcm10143121. J Clin Med. 2021. PMID: 34300287 Free PMC article.
-
Impact of retrograde anastomosis during supermicrosurgical lymphaticovenous anastomosis for cancer-related lower limb lymphedema: A retrospective cohort propensity-score-matched outcome analysis.Int J Surg. 2022 Aug;104:106720. doi: 10.1016/j.ijsu.2022.106720. Epub 2022 Jun 17. Int J Surg. 2022. PMID: 35724806
-
Supermicrosurgical Lymphaticovenous Anastomosis as Alternative Treatment Option for Moderate-to-Severe Lower Limb Lymphedema.J Am Coll Surg. 2020 Feb;230(2):216-227. doi: 10.1016/j.jamcollsurg.2019.10.007. Epub 2019 Oct 23. J Am Coll Surg. 2020. PMID: 31655173
-
Lymphaticovenous Anastomosis for Lower Extremity Lymphedema: A Systematic Review.Indian J Plast Surg. 2020 Mar;53(1):17-24. doi: 10.1055/s-0040-1709372. Epub 2020 Apr 17. Indian J Plast Surg. 2020. PMID: 32367914 Free PMC article. Review.
-
Lymphatic venous anastomosis (LVA) for treatment of secondary arm lymphedema. A prospective study of 11 LVA procedures in 10 patients with breast cancer related lymphedema and a critical review of the literature.Breast Cancer Res Treat. 2009 Jan;113(2):199-206. doi: 10.1007/s10549-008-9932-5. Epub 2008 Feb 13. Breast Cancer Res Treat. 2009. PMID: 18270813 Review.
Cited by
-
Recovery of Dysregulated Genes in Cancer-Related Lower Limb Lymphedema After Supermicrosurgical Lymphaticovenous Anastomosis - A Prospective Longitudinal Cohort Study.J Inflamm Res. 2022 Feb 4;15:761-773. doi: 10.2147/JIR.S350421. eCollection 2022. J Inflamm Res. 2022. PMID: 35153500 Free PMC article.
-
Peripheral T cell profiling reveals downregulated exhaustion marker and increased diversity in lymphedema post-lymphatic venous anastomosis.iScience. 2023 May 6;26(6):106822. doi: 10.1016/j.isci.2023.106822. eCollection 2023 Jun 16. iScience. 2023. PMID: 37250774 Free PMC article.
-
Outcomes of Lymphovenous Anastomosis for Lower Extremity Lymphedema: A Systematic Review.Plast Reconstr Surg Glob Open. 2022 Oct 7;10(10):e4529. doi: 10.1097/GOX.0000000000004529. eCollection 2022 Oct. Plast Reconstr Surg Glob Open. 2022. PMID: 36225843 Free PMC article.
-
Modern approaches to lymphatic surgery: a narrative review.Transl Breast Cancer Res. 2025 Jan 21;6:6. doi: 10.21037/tbcr-24-49. eCollection 2025. Transl Breast Cancer Res. 2025. PMID: 39980814 Free PMC article. Review.
-
Vascular Endothelial Growth Factor C (VEGF-C) Sensitizes Lymphatic Endothelial Cells to Oxidative-Stress-Induced Apoptosis through DNA Damage and Mitochondrial Dysfunction: Implications for Lymphedema.Int J Mol Sci. 2024 Jul 17;25(14):7828. doi: 10.3390/ijms25147828. Int J Mol Sci. 2024. PMID: 39063073 Free PMC article.
References
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources
Research Materials
Miscellaneous

