The Incidence of Epstein-Barr Virus-Positive Diffuse Large B-Cell Lymphoma: A Systematic Review and Meta-Analysis
- PMID: 33917961
- PMCID: PMC8068359
- DOI: 10.3390/cancers13081785
The Incidence of Epstein-Barr Virus-Positive Diffuse Large B-Cell Lymphoma: A Systematic Review and Meta-Analysis
Abstract
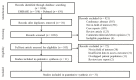
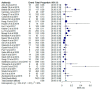
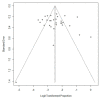
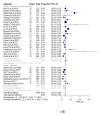
The worldwide prevalence of Epstein-Barr virus-positive (EBV+) diffuse large B-cell lymphoma (DLBCL) is undetermined. There is no clearly defined cut-off for EBV-encoded RNA (EBER) positivity in tumor cells by in-situ hybridization. The purpose of this study was to establish the proportions of EBV+ DLBCL patients and influence of the different cut-offs for EBER positivity, geographical location, and age on the prevalence of EBV+ DLBCL. PubMed and EMBASE were searched for studies published up to May 28, 2020 that reported proportions of EBER positivity in immunocompetent and de novo DLBCL patients. The pooled proportions were computed by an inverse variance method for calculating the weights and the DerSimonian-Laird method. Multiple subgroup analyses were conducted to explore any heterogeneity. Thirty-one studies (8249 patients) were included. The pooled proportion of EBV+ DLBCL was 7.9% (95% CI, 6.2-10.0%) with significant heterogeneity among studies (p < 0.001). The prevalence of EBV+ DLBCL was significantly higher in Asia and South America compared with Western countries (p < 0.01). The cut-offs for EBER positivity (10%, 20%, 50%) and patients' age (≥50 years vs. <50 years) did not significantly affect the prevalence (p ≥ 0.10). EBV+ DLBCL is rare with a pooled proportion of 7.9% in patients with DLBCL and the geographic heterogeneity was confirmed.
Keywords: immunohistochemistry; in situ hybridization; lymphoma; meta-analysis; systematic review.
Conflict of interest statement
The authors declare no conflict of interest.
Figures


Similar articles
-
Clinical impact of serum survivin positivity and tissue expression of EBV-encoded RNA in diffuse large B-cell lymphoma patients treated with rituximab-CHOP.Oncotarget. 2017 Feb 21;8(8):13782-13791. doi: 10.18632/oncotarget.14636. Oncotarget. 2017. PMID: 28099151 Free PMC article. Clinical Trial.
-
[Prevalence and clinico-pathological characteristics in patients with Epstein-Barr virus-positive diffuse large B-cell lymphoma in a high complexity hospital in Cali, Columbia].Rev Esp Patol. 2019 Jul-Sep;52(3):139-146. doi: 10.1016/j.patol.2019.01.002. Epub 2019 Mar 23. Rev Esp Patol. 2019. PMID: 31213254 Spanish.
-
Epstein-Barr Virus-Positive Diffuse Large B-Cell Lymphoma: Is It Different between Over and Under 50 Years of Age?Asian Pac J Cancer Prev. 2016;17(4):2285-9. doi: 10.7314/apjcp.2016.17.4.2285. Asian Pac J Cancer Prev. 2016. PMID: 27221931
-
Epstein-Barr virus-positive diffuse large B-cell lymphomas of the elderly.Adv Anat Pathol. 2011 Sep;18(5):349-55. doi: 10.1097/PAP.0b013e318229bf08. Adv Anat Pathol. 2011. PMID: 21841405 Review.
-
EBV-positive diffuse large B-cell lymphoma of the elderly: 2016 update on diagnosis, risk-stratification, and management.Am J Hematol. 2016 May;91(5):529-37. doi: 10.1002/ajh.24370. Am J Hematol. 2016. PMID: 27093913 Review.
Cited by
-
Estimating the global burden of Epstein-Barr virus-related cancers.J Cancer Res Clin Oncol. 2022 Jan;148(1):31-46. doi: 10.1007/s00432-021-03824-y. Epub 2021 Oct 27. J Cancer Res Clin Oncol. 2022. PMID: 34705104 Free PMC article. Review.
-
Estimating the prevalence of Epstein-Barr virus in primary gastric lymphoma: a systematic review and meta-analysis.Infect Agent Cancer. 2023 Feb 10;18(1):8. doi: 10.1186/s13027-023-00482-2. Infect Agent Cancer. 2023. PMID: 36765388 Free PMC article.
-
A Rare Case of Systemic Epstein-Barr Virus-Positive Diffuse Large B-Cell Lymphoma With Hemophagocytic Lymphohistiocytosis in an Immunocompetent Young Man: Potential Diagnostic Pitfall and Therapeutic Challenge.J Med Cases. 2024 Nov;15(11):347-353. doi: 10.14740/jmc4314. Epub 2024 Oct 10. J Med Cases. 2024. PMID: 39421223 Free PMC article.
-
Nanotechnology Frontiers in γ-Herpesviruses Treatments.Int J Mol Sci. 2021 Oct 22;22(21):11407. doi: 10.3390/ijms222111407. Int J Mol Sci. 2021. PMID: 34768838 Free PMC article. Review.
-
Epstein-Barr Virus-Positive Not Otherwise Specified (EBV+ NOS) Lymphoma Presentation of Primary Bone Tumor Underlying a Pathological Fracture.Cureus. 2022 Jun 26;14(6):e26340. doi: 10.7759/cureus.26340. eCollection 2022 Jun. Cureus. 2022. PMID: 35903563 Free PMC article.
References
-
- Oyama T., Yamamoto K., Asano N., Oshiro A., Suzuki R., Kagami Y., Morishima Y., Takeuchi K., Izumo T., Mori S., et al. Age-related EBV-associated B-cell lymphoproliferative disorders constitute a distinct clinicopathologic group: A study of 96 patients. Clin. Cancer Res. Off. J. Am. Assoc. Cancer Res. 2007;13:5124–5132. doi: 10.1158/1078-0432.CCR-06-2823. - DOI - PubMed
-
- Nakamura S., Jaffe E., Swerdlow S. EBV positive diffuse large B-cell lymphoma of the elderly. In: Swerdlow S., Campo E., Harris N., editors. WHO Classification of Tumours of Haematopoietic and Lymphoid Tissues. International Agency for Research on Cancer; Lyon, France: 2008.
Publication types
Grants and funding
LinkOut - more resources
Full Text Sources
Other Literature Sources

