Association of Delirium during Critical Illness With Mortality: Multicenter Prospective Cohort Study
- PMID: 33929361
- PMCID: PMC8542584
- DOI: 10.1213/ANE.0000000000005544
Association of Delirium during Critical Illness With Mortality: Multicenter Prospective Cohort Study
Abstract
Background: The temporal association of delirium during critical illness with mortality is unclear, along with the associations of hypoactive and hyperactive motoric subtypes of delirium with mortality. We aimed to evaluate the relationship of delirium during critical illness, including hypoactive and hyperactive motoric subtypes, with mortality in the hospital and after discharge up to 1 year.
Methods: We analyzed a prospective cohort study of adults with respiratory failure and/or shock admitted to university, community, and Veterans Affairs hospitals. We assessed patients using the Richmond Agitation-Sedation Scale and the Confusion Assessment Method for the intensive care unit (ICU) and defined the motoric subtype according to the corresponding Richmond Agitation-Sedation Scale if delirium was present. We used Cox proportional hazard models, adjusted for baseline characteristics, coma, and daily hospital events, to determine whether delirium on a given day predicted mortality the following day in patients in the hospital and also to determine whether delirium presence and duration predicted mortality after discharge up to 1 year in patients who survived to hospital discharge. We performed similar analyses for hypoactive and hyperactive subtypes of delirium.
Results: Among 1040 critically ill patients, 214 (21%) died in the hospital and 204 (20%) died out-of-hospital by 1 year. Delirium was common, occurring in 740 (71%) patients for a median (interquartile range [IQR]) of 4 (2-7) days. Hypoactive delirium occurred in 733 (70%) patients, and hyperactive occurred in 185 (18%) patients, with a median (IQR) of 3 (2-7) days and 1 (1-2) days, respectively. Delirium on a given day (hazard ratio [HR], 2.87; 95% confidence interval [CI], 1.32-6.21; P = .008), in particular the hypoactive subtype (HR, 3.35; 95% CI, 1.51-7.46; P = .003), was independently associated with an increased risk of death the following day in the hospital. Hyperactive delirium was not associated with an increased risk of death in the hospital (HR, 4.00; 95% CI, 0.49-32.51; P = .19). Among hospital survivors, neither delirium presence (HR, 1.01; 95% CI, 0.82-1.24; P = .95) nor duration (HR, 0.99; 95% CI, 0.97-1.01; P = .56), regardless of motoric subtype, was associated with mortality after hospital discharge up to 1 year.
Conclusions: Delirium during critical illness is associated with nearly a 3-fold increased risk of death the following day for patients in the hospital but is not associated with mortality after hospital discharge. This finding appears primarily driven by the hypoactive motoric subtype. The independent relationship between delirium and mortality occurs early during critical illness but does not persist after hospital discharge.
Trial registration: ClinicalTrials.gov NCT00392795 NCT00400062.
Copyright © 2021 International Anesthesia Research Society.
Conflict of interest statement
Conflicts of Interest: See Disclosures at the end of the article.
Figures
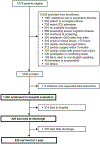

References
-
- Milbrandt EB, Deppen S, Harrison PL, et al. Costs associated with delirium in mechanically ventilated patients. Crit Care Med. 2004;32(4):955–962. - PubMed
-
- Ouimet S, Kavanagh BP, Gottfried SB, Skrobik Y. Incidence, risk factors and consequences of ICU delirium. Intensive Care Med. 2007;33(1):66–73. - PubMed

