Spontaneous regression of lung metastases after transarterial chemoembolization for hepatocellular carcinoma
- PMID: 33948129
- PMCID: PMC8081867
- DOI: 10.1016/j.radcr.2021.03.027
Spontaneous regression of lung metastases after transarterial chemoembolization for hepatocellular carcinoma
Erratum in
-
Erratum regarding missing Declaration of Competing Interest statements in previously published articles.Radiol Case Rep. 2022 Sep 28;17(12):4934. doi: 10.1016/j.radcr.2022.08.055. eCollection 2022 Dec. Radiol Case Rep. 2022. PMID: 36311873 Free PMC article.
Abstract
Spontaneous regressions of primary and/or metastatic lesions have been rarely reported in hepatocellular carcinoma (HCC). Herein, we report the case of a 71-year-old man with HCC, focusing on shape changes of lung metastases over time. Lung metastasis of HCC was histologically diagnosed by percutaneous computed tomography (CT)-guided needle biopsy after the treatment of primary HCC lesion. Lung lesions had been observed on enhanced contrast computed tomography for >3 years without any local or systemic treatment for them. During this period, treatments including surgical procedure for relapsed bladder cancer and transarterial chemoembolization for HCC were performed. Metastatic lung lesions immediately regressed after these treatments. Therefore, accumulation of such cases may help elucidate spontaneous regression mechanisms in primary HCC or its lung metastases.
Keywords: Computed tomography-guided needle biopsy; Hepatocellular carcinoma; Lung metastases; Spontaneous regression; Transarterial chemoembolization.
© 2021 The Authors. Published by Elsevier Inc. on behalf of University of Washington.
Figures

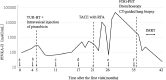


References
Publication types
LinkOut - more resources
Full Text Sources
Other Literature Sources

